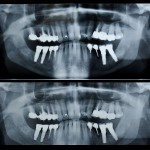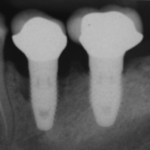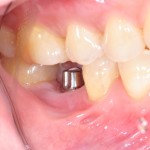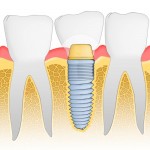
This review comparing the incidence of peri-implant disease with cement- and screw-retained prostheses included 6 RCTs. The findings suggest no difference in level of peri-implant disease with cement- or screw retained prosthesis. However, the studies are small none of them are at low risk of bias. Consequently the findings should be interpreted cautiously.
[read the full story...]