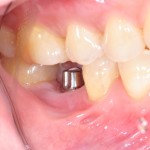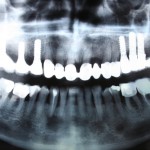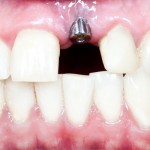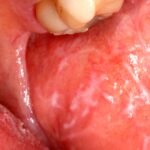
In this blog Rajpal Tattar looks at a review and meta-analysis investigating the correlation between oral lichen planus and peri-implant disease. Only two small observational studies were included so the availabel evidence is very limited.
[read the full story...]