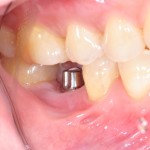
With the increasing use of dental implants are a restorative option there has also been an increase in the number of patients with peri-implant disease. The presence or previous history of periodontal disease as a risk factor for peri-implant disease has been studied although the level of association between them has been inconsistent.
The aim of this review was to a assesses whether dental implants placed in patients with periodontitis have a higher risk of peri-implantitis.
Methods
Searches were conducted in the PubMed, Cochrane Library, the Web of Science and U.S National Institute for Health (U.S. Clinical Trials) databases. observational, case-control, cross-sectional, and prospective or retrospective cohort studies published in English were considered. 3 reviewers independently selected studies, abstracted studies and assessed study quality using the modified Newcastle Ottawa scale for cohort, case-control, and cross-sectional studies. The primary outcome was the peri-implantitis and meta-analysis were conducted with subgroup analysis by study design.
Results
- 19 studies (5 cohort, 2 case-control, 12 cross-sectional) involving a total of 4322 patients and 10,075 implants were included.
- Prevalence of peri-implantitis ranged from 1.66 % to 71.8% in patients and 1.04% to 68% for implants.
- All the cohort and case-control studies were considered to be at low risk of bias, and just 1 cross-sectional study was considered to be at high risk of bias.
- All but two studies reported an association between periodontitis and peri-implantitis
- Meta-analysis (15 studies) found a greater chance of peri-implantitis in patients with periodontitis odds ratio (OR) = 2.29 (95%CI; 1.34-3.24). Results for the difference study designs are shown in table below.
| Study design | No of studies | Odds Ratio (95%CI) |
| Cohort | 2 | 5.15 (-3.35 to 13.65) |
| Case Control | 2 | 22.90 (10.01 to 35.80) |
| Cross-sectional | 11 | 1.74 (1.10 to 2.39) |
Conclusions
The authors concluded: –
This systematic review showed that diagnosis or history of periodontitis was associated with the occurrence of peri-implantitis. However, this association was not observed when only the cohort studies were analysed. Results should be evaluated with caution due to heterogeneity among the included primary studies.
Comments
A previous systematic review by Sgolastra et al (Dental Elf – 16th Jan 2014) looked at the relationship between periodontal disease and peri-implantitis and included 14 prospective cohort studies. While this new review includes 19 studies only 5 of them have been considered to be cohorts and only 4 f them are common to both reviews. The Sgolastra review showed an increase risk of peri-implantitis with periodontally compromised patients with RR= 2.21 (95%CI; 1.42– 3.43). The current review has expressed the outcomes using odds ratio and it is interesting to see the impact of the study designs with best study design included in this review (Cohort) suggesting no association. One of the challenges with conducting review in this area is the variation in the disease definitions for both periodontal disease and peri-implantitis. Higher quality well-reported prospective studies are needed to clarify the risks for patients undergoing implant treatment. There is also a need to agree a set of common outcomes ( http://www.comet-initiative.org/) which include patient focussed outcomes to provide clearer evidence in the future.
Links
Primary Paper
Ferreira SD, Martins CC, Amaral SA, Vieira TR, Albuquerque BN, Cota LOM,Esteves Lima RP, Costa FO. Periodontitis as a risk factor for peri-implantitis: Systematic review and meta-analysis of observational studies. J Dent. 2018Dec;79:1-10. doi: 10.1016/j.jdent.2018.09.010. Epub 2018 Nov 2. Review. PubMed PMID: 30391683.
Other references
Dental Elf – 16th Jan 2014
Periodontitis is a risk factor for dental implant loss and peri-implantitis
Dental Elf – Peri-implantitis blogs
