With an increase in the placement of dental implants over time, their associated complications including peri-implant disease is also projected to increase. Subsequently, there has been a growing interest in the prevention and management of these conditions. The presence or previous history of periodontal disease as a risk factor for peri-implant disease has been studied although the level of association between them has been inconsistent (Dental Elf – 18th February 2019). Recently, oral lichen planus has also been considered as a potential risk factor in the development of peri-implant disease.
The aim of this systematic review and meta-analysis was to investigate the correlation between oral lichen planus and peri-implant disease.
Methods
The Preferred Reporting Items for Systematic Review and Meta-Analyses (PRISMA) were used to inform the methodology of this review. Medline, Embase, Web of Science, the Cochrane Library and Scopus were the databases searched. Only observational human studies in which oral lichen planus and peri-implant diseases were assessed with a follow up period of ≥1 month after implant placement were included. The Newcastle Ottawa Scale and the Agency for Healthcare Research and Quality standards were used to assess the quality and risk of bias respectively. Risk ratios were calculated with 95% confidence intervals and meta-analysis was conducted to quantify the association between oral lichen planus and the risk of peri-implantitis and peri-implant mucositis. Meta-regression was used to investigate potential confounding factors.
Results
- 2 studies (one prospective, one cross-sectional) were included in this review.
- Both studies assessed bone loss, bleeding on probing, clinical attachment levels and probing depths associated with placed implants as well as the presence of peri-implantitis and peri-implant mucositis in patients with and without OLP.
- The follow-up period ranged from 12 to 120 months.
- The outcomes regarding probing depth and bone loss could not be combined because they were reported in different forms.
- Meta-analysis of both studies showed no significant differences in the number of implants with peri-implantitis (RR = 1.49, 95% CI: 0.77–2.90) or per-implant mucositis (RR = 0.88, 95% CI: 53–1.46) between the oral lichen planus and non-oral lichen planus groups.
- Meta-analysis of the 2 studies also showed no significant differences between the oral lichen planus and non-oral lichen planus groups when combining peri-implantitis and peri-implant mucositis into a peri-implant disease group (RR = 1.08, 95% CI: 0.75–1.55).
- Both studies had a low risk of bias and were determined to be high quality.
Conclusions
The authors concluded: –
Available articles regarding the effects of OLP on PIDs remains very limited. Existing evidence does not support OLP as a suspected risk factor for PIDs. Large-scale prospective trials are required to validate the findings.
Comments
This systematic review and meta-analysis determined that oral lichen planus is not a risk factor for peri-implant disease. The two studies included in the review had conducted implant placement during the remission stages of OLP however patients with acute or poorly controlled oral lichen planus may be at greater risk of peri-implant disease. This merits further investigation. Only 2 studies were pooled in this review demonstrating the limited literature currently available and the need for further comprehensive prospective trials to assess the risk between oral lichen planus and peri-implant disease. Therefore, no changes in clinical practice can be recommended based on the current level of evidence.
Links
Primary paper
Xiong, X., Xu, T., Wang, X. et al. Is oral lichen planus a risk factor for peri-implant diseases? A systematic review and meta-analysis. BMC Oral Health 20, 150 (2020). https://doi.org/10.1186/s12903-020-01134-2
Other references
Dental Elf – 18th February 2019
Picture Credits
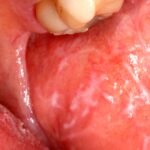
“File:Lichen planus.jpg” by Ian Furst is licensed under CC BY-SA 4.0
