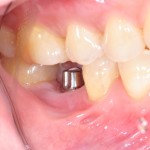
Dental implant treatments is now a well-established approach to tooth replacement with studies demonstrating good long -term survival rates. However, dental implant treatment is not within its problems. Peri-implantitis is a common cause of implant failure with studies suggesting that it might affect between 28-56% of patients. Various approaches to the management of peri-implantitis have been suggested including non-surgical, surgical and regenerative procedures.
The aim of this review was to evaluate the current literature on the surgical treatment of peri-implantitis and assess the effectiveness of treatment modalities (and adjunctive therapies) on peri-implant and periodontal radiographic outcomes.
Methods
Searches were conducted in the Medline, Embase, EBM review, Cochrane Central Register of Control Trials and Cochrane Database of Systematic Reviews. Randomised controlled trials (RCTs) or prospective cohort studies (PCS) with a minimum of 10 patients, 6 months follow up and published in English were considered. Study quality was assessed using a modified CASP checklist categorised as low risk (all the criteria were met), moderate risk (1–2 criteria were missed) or high risk (>2 criteria were missed). The primary outcome was the reduction in BOP in implants treated surgically for peri-implantitis. The secondary outcomes were periodontal probing depth (PPD) and RBL (radiographic bone loss). Meta-analyses were conducted separately for the parameters PPD and RBL
Results
- 16 studies (9 RCTs, 4 comparative prospective studies, 3 single group prospective studies. were included.
- 53% of studies were considered to have a high risk of bias, 35% a moderate risk and 12% at low risk of bias.
- Most studies followed up patients for 12 months (range 6-60 months).
- 44% of the studies involved bone augmentation following mechanical debridement, 38% mechanical debridement combined with surface decontamination, 12% considered mechanical debridement only and 6% of studies examined mechanical debridement with implantoplasty.
- 10 studies (8 RCTs, 2PCS) contributed to a meta-analysis
| Periodontal probing depth reduction
Standardised mean difference mm (95% CI) |
Radiographic bone loss
Standardised mean difference mm (95% CI) |
|
| Surface decontamination | 0.21 (1.70 to 1.27) | 0.54 (0.20 to 1.28) |
| Implantoplasty | 3.33 (4.37 to 2.28) | 3.38 (4.43 to 2.33) |
| Bone augmentation + grafting materials | 0.15 (0.55 to 0.84) | 1.05 (1.80 to 0.31) |
| Bone augmentation + grafting materials + membrane | 0.30 (0.31 to 0.91) | 0.16 (0.56 to 0.24) |
Conclusions
The authors concluded: –
The outcomes of the currently available surgical interventions for peri-implantitis remain unpredictable. There is no reliable evidence to suggest which methods are the most effective. Further randomised- controlled studies are needed to identify the best treatment methods.
Comments
We looked at a previous review of this topic last year (Dental Elf – 5th Jul 2017) which more closely followed the PRISMA reporting guidelines that the current review. Having been conducted over roughly the same time period this review has identified a similar number of studies, although restricting the search to those published in English may have resulted in exclusion of some relevant studies. The earlier review included 3 RCTs compared with 9 RCTs in this new review. The authors used a modified CASP worksheets to assess study quality when given that the well-established Cochrane Risk of tool is now more commonly used to assess this, and the Newcastle-Ottawa Scale or ROBINS-I tool could have been used for the non-randomised studies included.
Only a small number of the included studies were considered to be a low risk of bias which is similar to the earlier review. With increasing numbers of implants being placed there is a potentially larger pool of patients at risk of peri-implantitis so more high quality studies are needed to assess the best management approaches this condition.
Links
Primary Paper
Al‐Kadhim, K. , Pritchard, M. , Farnell, D. , Thomas, D. , Adams, R. and Claydon, N. (2018), Surgical therapy for peri‐implantitis management: a systematic review and meta‐analysis. Oral Surg. . doi:10.1111/ors.12344
Other references
Dental Elf – 5th Jul 2017
Peri-implantitis: lack of high quality studies for surgical regenerative treatment
Dental Elf Peri-implantitis Blogs

[…] post Peri-implantitis: Are surgical treatments effective? appeared first on National Elf […]