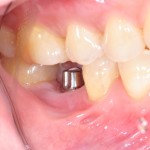
The increasing provision of dental implants has seen a steady increase in peri-implant diseases of mucositis and peri-implantitis. With peri-implantitis frequencies at implant level been reported to be between 1-47%.
The aim of the review was to assess the impact of peri-implant maintenance therapy (PIMT) on the prevention of peri-implant diseases.
Methods
Searches were conducted independently by 3 reviewers in the Medline,Embase, Cochrane Central Register of Controlled Trials, and Cochrane Oral Health Group Trials Register databases. This was supplemented by a manual search of the Journal of Dental Research, Journal of Clinical Periodontology, Journal of Periodontology and the International Journal of Periodontics and Restorative Dentistry from January 2014 up to February 2015.
Prospective or retrospective, randomized or not, cohort or case series trials aimed at showing the incidence or recurrence of peri-implant diseases under a strict regime of PIMT with a minimum of 10 patients and follow up of more than 6 months were considered. Three reviewers independently selected studies and abstracted data with 2 reviewers assessing study quality using the Newcastle-Ottawa Scale (NOS). Meta-analysis was conducted to evaluate the influence of PIMT and other reported variables upon peri-implant diseases.
Results
- 13 studies were included with 10 contributing to the meta-analysis
- At patient level mucositis ranged from 18.5-74.2% and peri-implantitis from 8-28%
- Mucositis was affected by history of periodontitis and mean PIMT at implant and patient levels, respectively.
- Similarly, significant effects of history of periodontal disease were obtained for peri-implantitis for both implant and patient levels.
- Mean PIMT interval was demonstrated to influence the incidence of peri-implantitis at implant but not patient level. PIMT interval showed significance at both levels.
Conclusions
The authors concluded:
Within the limitations of the present systematic review, it can be concluded that implant therapy must not be limited to the placement and restoration of dental implants but to the implementation of PIMT to potentially prevent biologic complications and hence heighten the long-term success rate. Although it must be tailored to a patient’s risk profiling, our findings suggest reason to claim a minimum recall PIMT interval of 5 to 6 mo. Additionally, it must be stressed that even in the establishment of PIMT, biologic complications might occur. Hence, patient-, clinical-, and implant-related factors must be thoroughly explored.
Comments
With increasing use of implants there have been an increasing number of reviews looking at the management of peri-implant disease. One of the earliest was the 2012 Cochrane review by Esposito et al which concluded,
There is no reliable evidence suggesting which could be the most effective interventions for treating peri-implantitis. This is not to say that currently used interventions are not effective.
Since then there have been a number of other reviews looking at different treatment approaches. This new review looks at prevention rather than treatment. While an extensive search has been conducted only a small number of studies could be included while study quality has been assessed there is no indication as to how many of the studies were retrospective. Consequently these results should be interpreted with caution. If peri-implant disease is going to be successfully prevented high quality prospective studies are needed.
Links
Primary paper
Monje A, Aranda L, Diaz KT, Alarcón MA, Bagramian RA, Wang HL, Catena A. Impact of Maintenance Therapy for the Prevention of Peri-implant Diseases: A Systematic Review and Meta-analysis. J Dent Res. 2015 Dec 23. pii: 0022034515622432. [Epub ahead of print] Review. PubMed PMID: 26701350.
Other references
Dental Elf – 26th Oct 2015 – Peri-implant disease: Limited evidence for the use of air polishing
Dental Elf – 22nd Apr 2015 – Peri-implantitis: lack of clarity on best self-management options
Dental Elf – 15th Apr 2015 – Peri-implantitis: a common complication of dental implants?
Dental Elf – 27th Oct 2014 – Peri-implantitis: lack of high quality evidence for surgical approaches
Esposito M, Grusovin MG, Worthington HV. Interventions for replacing missing teeth: treatment of peri-implantitis. Cochrane Database of Systematic Reviews 2012, Issue 1. Art. No.: CD004970. DOI: 10.1002/14651858.CD004970.pub5.

What is the impact of peri-implant maintenance therapy? https://t.co/AmjzXd1dmb
Peri-implant maintenance therapy may reduce biologic complications https://t.co/AmjzXd1dmb
Does peri-implant maintenance therapy reduce biologic complications? https://t.co/AmjzXd1dmb
Limited evidence on impact of peri-implant maintenance therapy https://t.co/AmjzXd1dmb
Does peri-implant maintenance therapy prevent biologic complications? https://t.co/AmjzXcJBXB