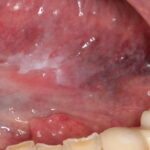
Oral Squamous cell carcinoma (OSCC) is the most common type of oral cancer (Scully and Bagan, 2009). There has been a recent increase in the number of oral squamous cell carcinoma cases in younger patients, particularly those without prior exposure to traditional risk factors such as alcohol and tobacco (Ng et al., 2017). Regional cervical lymph node metastasis is the most crucial prognostic indicator for survival (D’Cruz et al., 2015). T1-2 OSCC with clinically negative nodes (cN0) has a high risk of cervical lymph node metastasis. Despite advanced imaging, 8.5-45% of patients will have occult cervical lymph node metastasis with early T1-2 OSCC (with cN0 neck).
Patients with T1-2 OSCC will receive surgery and radical radiotherapy however when surgery is the first choice, the decision to undertake an elective neck dissection (END) or neck observation (OBS) is centre dependent with no universal consensus. There have been several studies (including randomised control trials) that have aimed to determine which approach is superior however, no significant results have been determined.
Therefore, the primary aim of this study was to conduct a systematic review and meta-analysis of all studies on END and OBS in patients with cT1-2 N0 OSCC.
Methods
Electronic databases of PubMed, Embase and the Cochrane libraries were searched. The title, abstract and full text of all identified articles were independently read by two reviewers. There were a range of inclusion criteria for studies to be included in the meta-analysis such as no prior-treatment before surgery, regular follow-ups and reporting of outcomes of END or OBS.
All included studies were assessed for quality by two independent reviewers. For randomised control trials, the Cochrane risk of bias tool was used and the quality of retrospective studies assessed using the Newcastle-Ottawa Quality Assessment Scale.
Odds ratios of neck nodal recurrence and their 95% confidence intervals were calculated for each study. Hazard ratios with their 95% confidence intervals were used to calculate survival outcomes of disease-free, disease-specific and overall survival. These were extracted from articles or calculated from articles that listed Kaplan-Meier curves. Statistical heterogeneity between studies were calculated using the Cochrane Q test and I2 statistic. Begg’s test and Egger’s test were used to evaluate publication bias.
Results
- 41 studies were included in this review of which 5 were randomized control trials and 36 were retrospective studies. Patients were from 17 countries in 5 continents. The meta-analysis included a total of 5705 patients (2796 END and 2909 OBS).
- The pooled odds ratio suggested END had a smaller risk of neck nodal recurrence compared with OBS (OR 0.45; 95% CI 0.32-0.63; P<0.00001).
- Subgroup analysis demonstrated that in all patients (except those with a primary tumour site of floor of mouth and in studies published after 2010), END treatment did not significantly reduce neck nodal recurrence.
- Overall survival was reported in 17 studies. The random effects model was used to analyse pooled hazard ratios and indicated the overall survival of patients who received END treatment was not improved (HR 0.83; 95% CI 0.67-1.04; p=0.10).
- 12 studies (2195 patients) provided data for a disease-free survival analysis. The fixed effects model was used to assess the pooled hazard ratios which showed the END group had a 48% benefit in disease-free survival compared with the OBS group (HR 0.52; 95% CI 0.42-0.63; P<0.00001).
- 12 studies (2212 patients) had data to analyse the relationship between disease-specific survival and END versus OBS in cT1-2 N0 OSCC. The random effects model demonstrated disease-specific survival was not improved in patients treated with END compared to patients with OBS (HR 0.87; 95% CI 0.48-1.57; p=0.65).
- During sensitivity analysis, studies with significant heterogeneity were excluded which demonstrated that there were no statistically significant differences in the overall survival analysis group or in the disease site-specific analysis group. Begg’s and Egger’s tests demonstrated no noticeable evidence of publication bias.
Conclusions
The authors concluded tha:-
… END may be associated with lower neck nodal recurrence in patients with cT1-T2 N0 OSCC and may confer a DFS benefit to patients with cT1-T2 N0 OSCC…
Comments
Previous studies have drawn limited conclusions in determining the impact of elective neck dissections on prognosis in patients with T1-2 oral squamous cell carcinomas. This well conducted meta-analysis utilised broad searches to maximise study retrieval and used hazard ratios to calculate survival outcomes. Additionally, statistical adjustments were made for studies with significant heterogeneity, identified through sensitivity analysis. The results show that elective neck dissection significantly reduces the risk of neck nodal recurrence in cT1-2 N0 OSCC with those patients having a significantly higher disease-free survival. A similar study (Dental Elf – 29th Jan 2020) compared local resection of T1-2 oral squamous cell carcinoma with or without neck dissection. Their results demonstrated that patients who underwent a neck dissection had improved 5-year overall survival and 5-year disease free survival rates compared to patients with resection alone. A further meta-analysis of randomised control trials involving the use of elective neck dissection demonstrated for overall survival, a reduction in the risk of death and with disease-free survival, a reduction in the risk of recurrence/death.
Links
Primary paper
Cai, H., Zhu, Y., Wang, C., Zhang, Y. & Hou, J. (2020) Neck nodal recurrence and survival of clinical T1-2 N0 oral squamous cell carcinoma in comparison of elective neck dissection versus observation: A meta-analysis. Oral Surgery, Oral Medicine, Oral Pathology and Oral Radiology, 129(4), 296-310.
Other references
D’Cruz, A. K., Vaish, R., Kapre, N., Dandekar, M., Gupta, S., Hawaldar, R., Agarwal, J. P., Pantvaidya, G., Chaukar, D., Deshmukh, A., Kane, S., Arya, S., Ghosh-Laskar, S., Chaturvedi, P., Pai, P., Nair, S., Nair, D. & Badwe, R. (2015) Elective versus Therapeutic Neck Dissection in Node-Negative Oral Cancer. N Engl J Med, 373(6), 521-9.
Ng, J. H., Iyer, N. G., Tan, M. H. & Edgren, G. (2017) Changing epidemiology of oral squamous cell carcinoma of the tongue: A global study. Head Neck, 39(2), 297-304.
Scully, C. & Bagan, J. (2009) Oral squamous cell carcinoma: overview of current understanding of aetiopathogenesis and clinical implications. Oral Dis, 15(6), 388-99.
Dental Elf -29th Jan 2020
Dental Elf – 9th Aug 2019
Picture Credits
By Coronation Dental Specialty Group – Own work, CC BY-SA 4.0, Link
