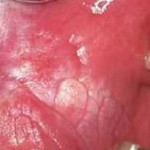
Oral squamous cell carcinoma (OSCC) is the 11th commonest cancer worldwide. There are 369,000 new cases annually with numbers rising. Treatment for patients with early stage disease with no neck nodes is usually surgical. However, there is debate about whether elective neck dissection (END) should be performed at the time of primary tumour removal.
The aim of this trial (the Selective Neck Dissection study, SEND) was to compare local resection with or without END in early mouth cancer, and in a Western population.
Methods
Patients aged ≥16 years with histopathologically confirmed T1/T2 OSCC; no evidence of nodal involvement in the neck (N0); and no cancer of the lip, previous oral/ pharyngeal SCC or other synchronous tumour were randomised using a centralised computer system. Patients were stratified by age (<40, 40–64, 65+years), tumour stage (T1 and T2) and surgeon. Data was also collected from a concurrent cohort of patients who declined participation in the trial had their preferred surgery (observational cohort).
For control patients, resection of the primary tumour was done through the open mouth, without neck incisions or neck surgery. Surgeons aimed for a >5mm clearance of the tumour at all margins and in all planes. Reconstruction was allowed but not if it involved any neck surgery.
The test group had standard END involved harvesting lymph nodes from levels I–IV including levels Ia/b and IIa/b on the same side as the tumour (ipsilateral). However, a level l–lll dissection and exclusion of level IIb could be performed if considered appropriate. In cases of recurrence in the mouth or neck, surgery (further resection and/or neck dissection) could be done according to local practice, with radiotherapy and/or platinum chemotherapy as recommended locally based on national guidelines. Baseline imaging scans were mandatory to detect features suggestive of clinically occult neck metastasis and any patients with these features were excluded. Almost all centres used ultrasound with fine needle aspiration cytology (US-FNAC) to detect neck metastasis at the trial outset with universal use by the trial end.
The primary outcome was overall survival (OS; death from any cause, and those who did not die were censored when last known to be alive). Secondary outcomes included: disease-free survival (DFS); loco-regional recurrence, adverse events (graded as mild, moderate, severe, or life threatening/disabling) occurring up to 6 months post-surgery, Health- related quality of life (assessed using the EORTC-QLQ-C30), NHS resource use.
Recruitment was closed early on the Independent Data Monitoring Committee (IDMC) recommendation as data were consistent with the published Mumbai trial showing benefit for END. Patients were followed up for 5 years.
A meta-analysis of this trial and 5 previously published trials of END was conducted.
Results
- Of 776 eligible screened patients 255 were randomised (Resection only =127; Resection & END =128) 162 were excluded and 359 agreed to be part of the observational cohort (Resection only = 234; Resection & END = 112).
- 7 patients randomised to the resection only group received END and 12 patients randomised to resection & END had resection only.
- 124 patients in the Resection group and 126 patients in the resection & END were flowed up for overall survival and disease-free survival.
- Patients were operated on by 68 surgeons from 27 hospitals across the UK National Cancer Research Network.
- Median follow-up was 57 months (25–75th centile 43–61 months)
- Among the 250 patients, there were 83 deaths (49 due to oral cancer).
- Overall survival (OS) and Disease-Free survival (DFS) for intention to treat and per protocol analyses are shown in the table.
| Resection only | Neck dissection | |
| N = 124 | N = 126 | |
| 5-year OS rates (ITT) | 67.6% | 75.8% |
| 5-year OS rates (per-protocol) | 65.6% | 77.5% |
| 5- year DFS rate (ITT) | 50.9% | 64.4% |
| 5- year DFS rate (per-protocol) | 47.8% | 65.7% |
The percentage of patients with adverse events is shown in the table below
| Adverse events | Resection only | Neck dissection |
| N = 124 | N = 126 | |
| Any | 60.5% | 77.8% |
| Low grade (G1-2) | 46.0% | 57.9% |
| Grade 3- 4 | 14.5% | 19.8% |
- Similar findings were demonstrated in the observational cohort.
- A meta-analysis of 6 RCTs of END in early stage cancer treatment showed
- for overall survival a pooled hazard ratio (HR) = 0.69 (95%CI; 0.55 to 0.87) in favour of END ie. A 31% reduction in the risk of death.
- a disease-free survival HR = 0.67 (95%CI; 0.46 to 0.98), or a 33% reduction in the risk of recurrence/death.
- Health-related quality of life (QoL)scores for both groups were similar with statistically significant differences only seen for dry mouth in END patients suggesting worsening QoL.
Conclusions
The authors concluded: –
SEND and the cumulative evidence show that within a generalisable setting oral cancer patients who have an upfront END have a lower risk of death/recurrence, even with small tumours.
Comments
This important UK multi-centre RCT originally designed to recruit 620 patients had recruitment stopped early by the independent data monitoring committee as preliminary data were consistent with the published Mumbai trial, which showed a benefit for END (D’Cruz et al, 2015) In all 255 patients were randomised with 250 patients providing data for overall survival and disease free survival after 5 years which provided sufficient power for some outcomes.
The trial shows a benefit in terms of overall and disease-free survival in favour of the END group. These findings were also supported by the concurrent cohort of non-randomised patients who were also monitored. In addition to the trial findings a meta-analysis of the 6 RCTS of END for oral squamous cell carcinoma also demonstrating a benefit in favour of END. While END showed better outcomes this group almost had more adverse effects although these were mainly considered to be low grade. With a previous study (Acevedo et al, 2016) indicating that END is a cost effective option there may now be enough evidence to amend existing guidelines regarding END for early stage oral cancer.
Links
Primary Paper
Hutchison IL, Ridout F, Cheung SMY, et al. Nationwide randomised trial evaluating elective neck dissection for early stage oral cancer (SEND study) with meta-analysis and concurrent real-world cohort. Br J Cancer. 2019;121(10):827–836. doi:10.1038/s41416-019-0587-2
Other references
D’Cruz AK, Vaish R, Kapre N, et al. Elective versus Therapeutic Neck Dissection in Node-Negative Oral Cancer. N Engl J Med. 2015;373(6):521–529. doi:10.1056/NEJMoa1506007
Acevedo JR, Fero KE, Wilson B, et al. Cost-Effectiveness Analysis of Elective Neck Dissection in Patients With Clinically Node-Negative Oral Cavity Cancer. J Clin Oncol. 2016;34(32):3886–3891. doi:10.1200/JCO.2016.68.4563
Dental Elf -9th Aug 2019
