
People with learning disabilities experience many inequalities in mental health services. Evidence suggests that approximately 2% of people have intellectual disabilities (Hatton et al, 2014) and they are four times more likely to develop mental health problems than the general population.
It’s estimated that:
- Between 20% to 40% of people with learning disabilities will experience symptoms of poor mental health (Taylor et al, 2004)
- Children with learning disabilities account for 14% of all children with mental health problems (Emerson & Hatton, 2007).
People with learning disabilities are a disadvantaged and vulnerable group who are likely to encounter increased psychosocial threats and difficulty accessing mental healthcare.
The ‘No Health without Mental Health’ strategy (Department of Health, 2011) and implementation framework (Department of Health, 2012) set out a vision for improving mental health and wellbeing in England. It highlighted the need to ensure that mainstream services were able to include people with learning disabilities and autism, that staff in these services had appropriate skills and could provide reasonable adjustments to meet the individual needs of this group of people (NHS England, 2015).
This paper, by Jacobs et al, (2015), reviewed research literature into the mental health needs of children with learning disabilities. It examined what is known about services currently provided, and reflected on the perspective of people with learning disabilities and their families to identify what they consider to provide good support and what challenges are experienced.
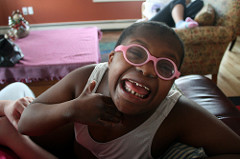
Research tells us that children with learning disabilities are 4 times more likely to develop mental health problems than the general population.
Methods
The scoping technique used allowed a narrative of available research without the quality appraisal and synthesis of systematic reviews (Arskey & O’Malley 2005).
The literature search was conducted using the Psychinfo, Medline, Embase and Social Care Online databases.
The final selection included 34 papers. The majority were papers from peer-reviewed journals in addition to nine reports and two book chapters. The publications used a variety of methods, including:
- mapping exercises
- secondary data analysis
- reviews of epidemiological data
- literature reviews, and
- qualitative and quantitative studies.
The studies were conducted in a wide range of countries; 11 in total including England.
Results
The researchers highlight policies and initiatives aimed at improving mental health services for children with learning disabilities. They draw attention to the high prevalence of poor mental health in children with learning disabilities and the multiple barriers experienced in accessing mental health services.
The study suggests the need for the improvement of services which are described as inadequate and introduces four models from the literature that offer some benefit. They also highlight the lack of evidence as to how these specific models of care would be more appropriate and how they would lead to better outcomes.
The researchers call for more research that link resources to specific models and service user outcomes.
Conclusions
The study draws attention to the need for the expansion and improvement of mental health support available to children with learning difficulties who are experiencing mental health problems.
The researchers found no evidence comparing service models to better outcomes. Children with learning disabilities and mental health problems fall between services and their support is reliant on sporadic community services.
Their review of studies across other countries showed the same lack of support with little evidence to suggest which models worked best. The studies reinforce the findings that children with mental health problems face significant barriers to accessing good support. Similarly, they found that this lack of support was higher in families from different ethnic backgrounds, particularly South Asian communities, who were found to have greater difficulty accessing mental health support.
Strengths and limitations
This study reinforces the need for better mental health support for people with learning disabilities and offers a good literature review on the challenges and barriers to accessing and developing good mental health services.
However, there are some models of service development that have not been considered, like the THRIVE model which suggested an early response at point of referral from the best practitioners (Wolpert et al, 2015). This is not to suggest that the study would have reached a different conclusion, but that there is a need for more research to test these models. At a time, however, when ‘transformation’ of services is at the forefront of change in practice, a contribution to the debate on which models could provide best support would have been invaluable.
Similarly the voices of people with learning disabilities and their families could have had a stronger focus in this study, which would have in turn strengthened their contribution to the transformation of services debate.
This study simply highlights that a negligible change in practice has occurred in the last 14 years, but offers little in developing our thinking on the models of service that might offer a glimpse of what ‘good’ could look like.
Summary
The limitations in research and the need for more in depth studies on the models of support is the main emphasis of the study. The models highlighted should include those that focus on prevention that could enhance our understanding of early intervention and what good support could look like.
The THRIVE model provides a real solution to ensuring that support is offered in a timely way to all at point of referral, with a response from the best practitioners in a multidisciplinary team, which should include the Department of Education who are often the missing partner.
There is a need to build the confidence of mainstream practitioners to understand that the best mainstream support should be available to all, including people with learning disabilities. As well as a need to create an understanding that the reasonable adjustments needed to support effective individual care are a legal requirement.
A stronger evidence base is crucial in strengthening our knowledge on the models of support, if we are to support effective services to meet the mental health needs of people with learning disabilities. This should include models that can prevent poor mental health and enhance the wellbeing of this group.

More evidence is needed on how to help people with learning difficulties achieve good mental health.
Links
Primary paper
Jacobs M, Downie H, Kidd G, Fitzsimmons L, Gibbs S, Melville C. (2016) Mental health services for children and adolescents with learning disabilities: a review of research on experiences of service users and providers. Br J Learn Disabil, 44: 225–232. doi:10.1111/bld.12141 [Abstract]
Other references
Cooper SA, Smiley E, Morrison J, Williamson A, Allan L. (2007) Mental ill-health in adults with intellectual disabilities: Prevalence and associated factors. British Journal of Psychiatry, Vol. 190, pp. 27–35.[PubMed abstact]
Department of Health (2011) No Health without Mental Health: A cross-government mental health outcomes strategy for people of all ages (PDF).
Department of Health (2012). No Health without Mental Health: Implementation Framework.
Emerson E, Hatton C. (2007) Mental health of children and adolescents with intellectual disabilities in Britain. British Journal of Psychiatry, 191 (6): 493–9. [Abstract]
Burke C. (2015) Feeling Down – Improving the mental health of people with learning disabilities (PDF). Foundation for People with Learning Disabilities. [website]
Hatton C, Emerson E, Glover G, Robertson J, Baines S, Christie A. (2014) People with Learning Disabilities in England 2013 (PDF). London: Public Health England.
Wolpert M, Harris R, Jones M, Hodges S, Fuggle P, James R, Wiener A, McKenna C, Law D, Fonagy P. (2014) THRIVE The AFC–Tavistock Model for CAMHS (PDF). CAMHS Press, 2014
NHS England (2015) Transforming Care for People with Learning Disabilities – Next Steps (PDF).
Taylor JL, Hatton C, Dixon L, Douglas C. (2004) Screening for psychiatric symptoms: PAS–ADD Checklist norms for adults with intellectual disabilities. Journal of Intellectual Disability Research, Vol. 48, pp. 37–41. [Abstract]


Hi @craigmelville33 We’ve blogged about yr review on mental health services for children with learning disabilities https://t.co/IHo2MrWuUb
Today Christine Burke @FPLD_Tweets on what good mental health support looks like 4 children w learning disabilities https://t.co/IHo2MrWuUb
Children with learning disabilities and their parents experience many barriers accessing mental health services https://t.co/IHo2MrWuUb
Children w learning disabilities are 4 times more likely to develop mental health problems than general population https://t.co/IHo2MrWuUb
@LearningDisElf so any new services for children with mental health problems must have skills to include those w learning disabilities.
In my early childhood I was in a Kindergarten for children with d too and wanted to develope better too! @learningdiself @chrishattoncedr
Our colleague, Christine Burke’s editorial on mental health support for children with learning disabilities
https://t.co/R9rfpw9v4i
Mental health support for children with learning disabilities https://t.co/pPB2Ea2Ksh via @sharethis @FPLD_tweets @mentalhealth
Review finds scant evidence 2 show which models of mental health support are best 4 children w learning disabilities https://t.co/IHo2MrWuUb
Don’t miss:
#MentalHealth support for #Children with #LearningDisabilities
https://t.co/IHo2MrWuUb
Don’t miss:
#MentalHealth support for #Children with #LearningDisabilities
https://t.co/1W1lGzJDwG by #LearningDisElf
Mental health service providers say lack of resources is main barrier to supporting children w learning disabilities https://t.co/IHo2MrWuUb
Mental health support for children with learning disabilities https://t.co/Lhuk974wbM
https://t.co/B4gOKgR0pq
Mental health support for children with learning disabilities https://t.co/nQADUyQ33T
Christine Burke’s editorial on mental health support for children with learning disabilities https://t.co/0SkGiOFmzK @FDLP_Tweets
[…] Mental health support for children with learning disabilities […]