
Depression is not the same across the life course, and we still don’t know which treatments work best for different people. There is evidence that older people with depression don’t respond as well to antidepressants as younger patients, so looking for ways of increasing the efficacy of treatments is a worthwhile effort.
The study I’ll be blogging about today was published recently in the American Journal of Psychiatry and investigated the use of combined methylphenidate and citalopram for geriatric depression:
- Methylphenidate may be familiar as a licensed treatment for ADHD in children. It works by inhibiting dopamine reuptake.
- Citalopram is an antidepressant that works by inhibiting serotonin reuptake.
The authors state that the reason for combining the two is to enhance citalopram response. According to the drugs.com entry for the combination of the two medications, “coadministration with methylphenidate may increase the plasma concentrations and effects of selective serotonin reuptake inhibitors (SSRIs)”.
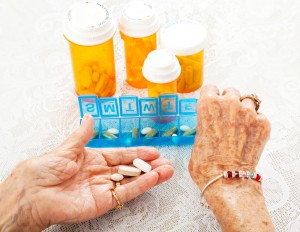
Research shows that antidepressants may be less helpful in older patients.
Methods
This recent study investigated three treatments:
- Methylphenidate plus placebo citalopram
- Citalopram plus placebo methylphenidate
- Combined methylphenidate and citalopram
The hypothesis was that the combination would lead to better (and faster) citalopram response and improvements in mood, function and cognition.
Participants were recruited via telephone screening and subsequent diagnostic interview. To be included in the trial, participants had to be experiencing a current episode of unipolar major depression, a score of 16 or greater on the 24-item Hamilton Depression Rating Scale (HAM-D), and a score of 26 or greater on the mini mental state examination.
Exclusion criteria were history of any psychiatric disorder apart from unipolar major depression with or without anxiety, severe or acute unstable medical illness, acute suicidal or violent behaviour or history of suicide attempt in the past year, or any other diseases of the central nervous system. Patients had to have been free of psychotropic medication for at least two weeks before starting the trial.
The primary outcome was improvement in the HAM-D score. Researchers also analysed the differences in the rate of response by week 4 of treatment (more on this later).
Secondary outcomes were symptoms of anxiety, apathy, medical and vascular risk factors, health-related quality of life, and cognitive performance as measured by a battery of validated cognitive tests. Remission, defined as a score of 6 or smaller on the HAM-D, was also analysed as a secondary outcome.
Participants were randomised using a computer-generated schedule. The researchers also created a guessing scale for study staff to monitor internal validity of the blinding. The accuracy of group guessing was 35%. I thought this was an interesting touch, possibly one that more trials should adopt.
Intervention
The first four weeks of the trial were dedicated to finding the correct dosages of methylphenidate and citalopram for each patient. This also meant that patients who couldn’t tolerate the minimum allowed dosage were discontinued from the trial. The only other medication participants were allowed was lorazepam as a “rescue medication” for anxiety. Participants were given their medication (or placebo) in two identical-looking capsules regardless of treatment condition. Mean dosages were: citalopram-only group (citalopram 35 mg/day); methylphenidate-only group (methylphenidate 16.4 mg/day); combination group (citalopram 32.3 mg/day, methylphenidate 16.2 mg/day).
143 participants entered the trial and were randomised into three groups of 48, 48 and 47 participants respectively. There were significant between-group differences in terms of the proportion of men and women, baseline HAM-D scores, and Cumulative Illness Scale. The researchers therefore attempted to control for this in their statistical analyses.
Dropout rates were high: between 14 and 18 participants from each group (that’s around 30%) discontinued the intervention for one reason or another. The mean time to dropout was around 30 days across groups, which coincides with the end of the dosage titration period.

This was a relatively small trial with high drop out rates.
Results
Findings for the primary outcome
There was a significant difference between groups in the change in HAM-D score from baseline to study end. Unfortunately the authors don’t give us a table with numbers, but we have a graph illustrating the rate of change.
- The change in HAM-D score was greater in the combination treatment group than in either of the other groups
- The rate of improvement was also much faster, especially in the first four weeks of treatment
- The combination group had the highest number and proportion of participants who had remitted:
- 29 of 47 patients in the combination group
- as opposed to 20 of 48 in the citalopram-only group
- and 14 of 48 in the methylphenidate-only group
- The remission rates were:
- 29.8% for those receiving 20 mg/day of citalopram
- 41.9% for those receiving 40 mg/day of citalopram
- 69.2% among those receiving 60 mg/day of citalopram
- There was no clear relationship between methylphenidate dosage and remission.
- The other participants in each group either had a partial response or no response to the treatment:
- There were 15 partial responses and 13 non-responses in the citalopram-only group
- 18 partial responses and 15 non-responses in the methylphenidate-only group
- 8 partial responses and 11 non-responses in the combination group
- Regardless of group, remission rate was significantly associated with citalopram dose.
Secondary outcomes
- All treatment groups improved on some of the cognitive tests
- All groups improved significantly on language
- Both the methylphenidate-only and the combination group improved globally
- The methylphenidate-only group also improved in executive functioning
- The citalopram-only group improved in attention
- These changes appeared to have no clear connection to the HAM-D score changes.

Improvement in depression severity and the Clinical Global Impressions improvement score was more prominent in the combination group.
Conclusions
This was a well-conducted randomised trial, which went to significant effort to minimise bias and ensure blinding of study personnel and participants.
On the whole, this study appears to give some legitimacy to a common “off-label” practice, although this research is certainly not sufficient on its own to change clinical practice. Adding methylphenidate to citalopram may be a way to improve the efficacy of treatment and rate of response for geriatric depression in individuals who respond to the treatment and are able to tolerate it.
Limitations
The study has several limitations:
- Firstly, the authors used a convenience sample of outpatients with moderate major depression and excluded individuals with histories of substance abuse and anxiety, so the results may not apply in more severe cases or in cases with comorbidities.
- Secondly, dropout rates were very high, and a considerable number of people dropped out because of side effects.
- Finally, citalopram was given above the FDA-recommended dose of 20 mg/day in elderly patients, which raises a flag about potential cardiac side-effects. Safety and tolerability was monitored throughout the study, but this limits clinical applicability, especially when taking into account that remission rates were highest among those taking citalopram dosages above these levels.

Further work is needed to ensure that citalopram is safe at these dosages in older people with depression.
Links
Primary paper
Lavretsky H et al. Citalopram, methylphenidate, or their combination in geriatric depression: A randomized, double-blind, placebo-controlled trial. Am J Psychiatry 2015 Feb 13.
Other references
Tomlin A. (2012) Antidepressants may be less effective in older patients with depression, according to new meta-analysis. The Mental Elf, 20 Jan 2012.

@Mental_Elf the fastest way to recover from depression is feeling it all without numbing the symptoms, it does hurt however
Combined methylphenidate and citalopram may help older people with depression… http://t.co/cwFfc7QVw4 #MentalHealth http://t.co/Vr9aXDjmtZ
Today @lisaburscheidt on an RCT of combined methylphenidate and citalopram for depression in older people http://t.co/Hvfpt55tED
http://t.co/8oTcI3fdVL
Mejor respuesta a #depresión en #mayores con #metilfenidato + antidepr. vs. Placebos
RT @Mental_Elf: Today @lisaburscheidt on a RCT of combined methylphenidate and citalopram for depression in older ppl http://t.co/hvSqIKwrl3
Combined methylphenidate and citalopram (high dose) may help older people with depression recover faster https://t.co/IMrBB1JdNz
A combination of medication may be better for treating older people w/ #depression Interesting study @Mental_Elf http://t.co/p3ubBs9Y4x
Don’t miss: Combined methylphenidate and citalopram may help older people with depression recover faster http://t.co/Hvfpt55tED #EBP
@Mental_Elf What’s the age limit for “older people” & “geriatric depression”? The website doesn’t mention any ages.
Thank you for asking, and sorry for the omission. Mean ages in this study were 70, 70.1 and 68.9 respectively for the three groups.
@Sectioned_ Thank you for asking, and sorry for the omission. Mean ages in this study were 70, 70.1 and 68.9 respectively for the three groups.
@Mental_Elf Older people may find it harder to metabolize an SSRI. Also makes them more prone to falls, fractures & death !
@Mental_Elf Can there be any more misinformation about these drugs out there ? They are poisons based on mythology.
This was a great summary but this one in particular and this site in general do not seem to comment on the conflicts of interest and pharma links of study authors, these are also not accessible via the paper abstracts which the summaries link to.
I think this is highly problematic and the Mental Elf might want to look at making this transparent in all research summaries.
Hi Andrew,
Thanks for the comment. I can’t speak for all the Elves but I think we try and highlight potential conflicts when we are aware of them. In this instance, I didn’t think the authors’ declarations represented a potential conflict of interest – none of them reported having received money from pharma companies or similar. You can see the authors’ declarations here, on the “References” tab of the link to the paper: http://ajp.psychiatryonline.org/doi/ref/10.1176/appi.ajp.2014.14070889
Combined methylphenidate and citalopram may help older people with depression recover faster https://t.co/WZWXoUEEfb via @Mental_Elf
Combined methylphenidate and citalopram may help older people with depression recover faster http://t.co/pYrRBeSC1L #EBP via @Mental_Elf
Combined methylphenidate and citalopram may help older people with depression recover faster https://t.co/HwqJRUScs1 via @sharethis