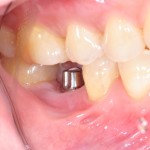
With the increase in use of dental implants maintaining the health of their supporting tissues is important. Failure to do this lead sto peri-implantitis and this requires treatment. As with periodontics both non-surgical and surgical approaches have been suggested.
The aim of this review was to assess the efficacy of different surgical approaches for the management of peri-implantitis.
Methods
The Medline, PubMed, Embase, and Dentistry and Oral Sciences Source databases were searched. This was supplemented by a hand search of 13 relevant dental journals. Case series (CS), cohort studies, quasi-experiments (QEs), and randomized controlled trials (RCTs) published in English looking at surgical approaches to treat peri-implantitis with a minimum 3 month follow up period were considered. Two reviewers independently selected studies, abstracted data and undertook risk of bias assessment of the studies.
Results
- 21 studies were included (5 RCTs, 2 QEs, 12 CS, and one cohort)
- 1 RCT was considered to have a low risk of bias, 3 a moderate risk and I RCT a high risk of bias.
- 4 treatment groups were identified, access flap and debridement only (4 studies); resective approach (2 studies); bone grafting 6 studies); guided bone regeneration (12 studies).
| Total number of patients | Weighted mean pocket depth reduction (mm) | 95% confidence interval | |
| access flap and debridement | 105 | 2.38 | 1.86 – 2.91 |
| resective approach | 47 | 2.04 | 1.87 – 2.19 |
| bone grafting | 99 | 2.32 | 1.04 – 3.61 |
| guided bone regeneration | 269 | 3.16 | 2.54 – 3.78 |
Conclusions
The authors concluded
Within the limitation of this systematic review, the application of grafting materials and barrier membranes resulted in greater PD reduction and RBF, but there is a lack of high-quality comparative studies to support this statement. The results might be used to project treatment outcomes after surgical management of peri-implantitis.
Commentary
Earlier this month (Dental Elf-20th Oct 2014) we looked at a review of non-surgical approaches for the management of peri-implantitis and found limited evidence to suggest which non-surgical approach was best. This review focused on just surgical approaches. The meta-analysis conducted suggests that studies using regenerative treatment provide the largest improvement in pocket depth although the authors themselves highlight significant variability in these studies. This is perhaps not surprising given the decision to include a wide range of study designs in the meta-analysis. RCTs are least prone to bias and only 1 of the 5 included was considered to be at low risk of bias. The results of this meta-analysis should therefore be interpreted with caution.
Links
Chan HL, Lin GH, Suarez F, MacEachern M, Wang HL. Surgical management of peri-implantitis: a systematic review and meta-analysis of treatment outcomes. J Periodontol. 2014 Aug;85(8):1027-41. doi: 10.1902/jop.2013.130563. Epub 2013 Nov 21. PubMed PMID: 24261909.
Dental Elf -20th Oct 2014 – Peri-implantitis:little evidence that particular non-surgical treatments are better than debridement alone
Esposito M, Grusovin MG, Worthington HV. Interventions for replacing missing teeth: treatment of peri-implantitis. Cochrane Database of Systematic Reviews 2012, Issue 1. Art. No.: CD004970. DOI: 10.1002/14651858.CD004970.pub5.

Don’t miss – Peri-implantitis: lack of high quality evidence for surgical approaches http://t.co/s4IeHzd1ob
[…] Dental Elf – 27th Oct 2014 – Peri-implantitis: lack of high quality evidence for surgical ap… […]