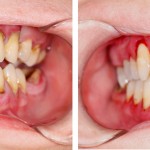
Diagnosis of periodontal disease usually consists of measuring clinical parameters such as pocket probing depth (PPD), clinical attachment levels (CALs), bleeding on probing, and radiography to assess alveolar bone level. Mediators of tissue destruction can be found in the saliva of patients with periodontal disease and the potential to use these biomarkers as a non-invasive of identifying patients with disease and monitoring the progress of treatment has been proposed.
The aim of this review was to evaluate the diagnostic value of salivary biomarkers in periodontal disease, in order to determine which of the numerous biomarkers reported in literature have an excellent or acceptable diagnostic test accuracy (DTA), and to provide insights for future studies in this emerging field.
Methods
Searches were conducted in the Medline, LILACS, Science Direct, Scopus, Web of Science and Goggle Scholar databases. Diagnostic studies assessing host-derived salivary biomarkers for periodontal disease diagnosis in humans, compared with accuracy a gold standard diagnostic technique [pocket probing depth (PPD) and clinical attachment levels (CAL)] measurements were considered.
Two reviewers independently selected studies with a single review abstracting data, which was crosschecked by a second reviewer. Study quality was assessed against the revised Quality Assessment of Diagnostic Accuracy Studies (QUADAS-2) tool. Sensitivity and specificity were the main outcome measures. Positive predictive value (PPV), negative predictive value (NPV), positive likelihood ratio (LR+), negative likelihood ratio (LR ), diagnostic odds ratio (DOR), and the Youden’s Index were also calculated
Results
- 4 studies involving a total of 313 patients were included.
- Sample sizes range from 74-99 patients.
- 17 different biomarkers were evaluated but only 12 had sensitivity and specificity assessed.
- The 12 markers were proteins and assessed by immunosorbent assays
- The risk of bias was high in all 4 studies.
- The sensitivity (41–95%) and specificity (40–100%) showed a wide range of values.
- Good sensitivity and specificity were reported for macrophage inflammatory protein-1a (MIP-1a), interleukin (IL)-6 and IL-1b.
- Only MIP-1a was considered to show satisfactory results for all test indicators.
| MIP-1a | IL -6 | IL-1b | |
| Sensitivity | 95 | 88 | 88 |
| Specificity | 93 | 97 | 93 |
| Positive predictive value | 92.86 | 98.00 | 95.44 |
| Negative predictive value | 94.79 | 82.91 | 82.30 |
| Positive likelihood ratio | 13.00 | 29.33 | 12.57 |
| Negative likelihood ratio | 0.06 | 0.12 | 0.13 |
| Diagnostic odds ratio | 236.29 | 237.11 | 97.43 |
| Youden’s Index | 0.88 | 0.85 | 0.81 |
Conclusions
The authors concluded:-
There is currently limited evidence to confirm the diagnostic capability of salivary biomarkers in the clinical assessment of periodontal disease. Notwithstanding, the summary findings showed the growing importance of salivary biomarker, and can guide larger, well-controlled, diagnostic accuracy studies. Likewise, although not conclusive, MIP1α, IL-1β and IL-6 may be promising biomarkers for future studies.
Comments
While the authors originally identified 140 potential relevant papers for this review a large majority did not report sensitivity and specificity data or sufficient information to calculate this. Sensitivity and specificity data is a key requirement for diagnostic test accuracy studies so this is an issue that needs to be address in future studies in this area. Another important issue is the use of an appropriate diagnostic reference standard (gold standard). The authors specified the use of both PPD and CAL as it is considered that CAL on its own may result in false positive diagnosis. Inconsistencies in the diagnostic definitions of periodontitis also add to the problem of defining a consistent reference standard.
While the results of the review do point to the potential of 3 biomarkers the small number of included studies limited number of patients and the fact that they were all assessed as being at high risk of bias means that these findings should be interpreted with caution.
Links
Primary paper
de Lima CL, Acevedo AC, Grisi DC, Taba M Jr, Guerra E, Canto GL. Host-derived salivary biomarkers in diagnosing periodontal disease: Systematic review and meta-analysis. J Clin Periodontol. 2016 Mar 1. doi: 10.1111/jcpe.12538. [Epub ahead of print] Review. PubMed PMID: 26926312.

Salivary biomarkers for diagnosing periodontal disease https://t.co/nbqAb111zi
Limited evidence of diagnostic capability of salivary biomarkers in periodontal disease https://t.co/nbqAb111zi
Diagnosing periodontal disease using salivary biomarkers – limited evidence https://t.co/nbqAb111zi
Limited evidence for use of salivary biomarkers in diagnosing periodontal disease https://t.co/nbqAb111zi
@TheDentalElf The deep pocket is contaminated w/absolute anaerobic bacteria such as spirochete at gingival exudate.Maybe detected in saliva.
Don’t miss- Salivary biomarkers for diagnosing periodontal disease https://t.co/nbqAb111zi