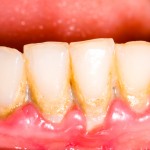
Periodontal disease is one of the worlds commonest diseases. Inadequate oral hygiene, smoking and diabetes are considered to be important risk factors. Accumulation of plaque and calculus leads to gingival inflammation and persistent gingivitis is an important predictor of periodontal breakdown. While poor oral hygiene (OH) is considered important the strength of the association between OH and periodontitis has not been quantified.
The main aim of this review was to estimate the effects of OH on periodontitis.
Methods
Searches were conducted in the Medline and Scopus databases. Observational studies (cohort, case–control or cross-sectional) assessing associations between oral hygiene and periodontitis in general or specific adult populations were considered. Two reviewers independently assess studies for inclusion. Key data items were extracted and study quality was assessed using the Newcastle–Ottawa Scale.
The main outcome was periodontitis. A multivariate random-effects meta-analysis was used to pool the effects of fair/poor OH versus good OH on periodontitis across studies. The associations between oral care habits and periodontitis were also assessed.
Results
- 50 studies were included, 45 involved oral examination, 11 oral health care habits.
- 3 studies were cohorts, 19 case-controlled, 28 cross-sectional
- 23 studies were considered to have a low risk of bias, 19 a moderate risk and 8 a high risk.
- 15 studies categorical data were pooled and the effect on periodontitis of
- fair OH v’s good OH; odds ratio(OR) = 2.04 (95%CI; 1.65-2.53)
- poor OH v’s good OH; OR = 5.01(95%CI; 3.40-7.39),
- 31 studies measured OH on a continuous scale finding that periodontitis patients had a significantly higher OH score, standardised mean difference (SMD)=2.04(95% CI; 1.59–2.50).
- Patients who brushed their teeth regularly had significantly lower odds of having periodontitis pooled OR = 0.66 (95%CI; 0.47–0.94) [10 studies].
- Regular dental visiting also demonstrated similar lower odds with pooled OR = 0.68 (95%CI; 0.47–0.98) [6 studies].
- The effect of dental floss on periodontitis was borderline significant OR = 0.87 (95%CI; 0.75–1.00) [4 studies].
- All the pooled estimates were scored as low quality using the GRADE approach.
Conclusions
The authors concluded: –
poor OH increases the risk of periodontitis by approximately two- to five-fold compared with good OH. Oral care habits, including regular brushing and dental visits, can decrease the risk of periodontitis and should thus be promoted as a public health intervention.
Comments
Only English language studies were included in this review so relevant studies could have been excluded. As the authors note all the included studies were observational with a majority being cross-sectional. They also note that many of the studies provided inadequate details regarding the samples used so there are important questions regarding representation. Failure to report or adjust for potential confounders in the original studies was also highlighted as an issue. These points taken together with a variation in the definition of periodontitis used amongst the included studies points to a need to be cautious in interpreting the findings. Some of the meta-analysis only used data from a small number of studies and the authors note that this could affect their validity. Concerns are also raised regarding the potential for publication bias. So, while the conclusions point to an association between poor oral hygiene and periodontitis the quality of the supporting evidence is low.
Links
Primary paper
Lertpimonchai A, Rattanasiri S, Arj-Ong Vallibhakara S, Attia J, Thakkinstian A. The association between oral hygiene and periodontitis: a systematic review and meta-analysis. Int Dent J. 2017 Jun 23. doi: 10.1111/idj.12317. [Epub ahead of print] Review. PubMed PMID: 28646499.
Other references
Dental Elf- 1st Jul 2016
