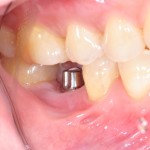
Peri-implant mucositis is a common inflammatory condition of the peri-implant mucosa without loss of the supporting bone. It results from biofilm accumulation and is characterised by bleeding on probing which may be resolved by good biofilm control. Treatments are focussed on biofilm disruption and control and a number of interventions have been reported, including oral hygiene instructions (OHI), curettes, ultrasonics, air-polishing and lasers.
The overall aim of this review was to assess the effectiveness of professional mechanical/physical treatment of peri-implant mucositis.
Methods
A protocol for the review was registered with PROSPERO. Searches were conducted in the Cochrane Database of Controlled Trials (CENTRAL), Medline, Embase and Scopus databases by a specialist librarian. Two reviewers independently screened and selected studies, extracted data and assessed risk of bias using the Cochrane risk-of-bias tool (RoB2) Randomised controlled trials (RCTs) published in English with minimum of 10 patient per arm at least 3 months follow-up were considered. Chemical therapies and non-professionally administered therapies were excluded. A range of implant and patient level outcomes were considered. For continuous outcomes results were expressed as difference in means (MD) with standard errors with odds ratios and 95% confidence intervals (CIs) for binary outcomes.
Results
- 5 RCTs (4 parallel, 1 split mouth) involving a total of 364 patients (383 implants) were included.
- All 5 trials were single-site University based studies.
- Sample sizes ranged from 12 to 220 patients with follow up periods range from 3 – 12 months.
- 2 studies were at high risk of bias and 3 had some concerns.
- Studies involving the use of air polishing, ultrasonics, curettes and laser therapy were reported in the included studies.
Conclusions
The authors concluded: –
Several mechanical/physical instrumentation procedures including curettes, ultrasonics, lasers, rotating brushes and air-polishing are documented, but a beneficial effect over OHI alone or superiority over other procedures could not be demonstrated. Moreover, it remains unclear whether combinations of different procedures or their repetition over time might provide additional benefits.
Comments
While the overall aim of this review was to assess the effectiveness of professional mechanical/physical treatment of peri-implant mucositis the authors were hoping to address 4 questions: –
- Is professionally administered non-surgical mechanical/physical therapy better than OHI alone?
- Is any single mode of professionally administered non-surgical mechanical/physical therapy superior to other single modes of therapy?
- Are combinations of treatment modes of professionally administered non-surgical mechanical/physical therapy superior to single modes?
- Does repetition of professionally administered non-surgical mechanical/physical therapy provide added benefits over single administration?
While a good number of databases were searched only a small number of RCTs met the overall inclusion criteria and none of the studies were at low risk of bias. Consequently, no studies were included that addressed questions 1 and 4. Two studies addressed question 2 and 3 studies question 3 but owing to variability in the interventions, comparisons, and outcomes no meta-analyses were undertaken. The limited number and low quality of the available studies means that high quality well reported studies of appropriate size, duration and using common outcomes are needed to provide good evidence to inform clinical practice.
Links
Primary Paper
Verket A, Koldsland OC, Bunaes D, Lie SA, Romandini M. Non-surgical therapy of peri-implant mucositis-Mechanical/physical approaches: A systematic review. J Clin Periodontol. 2023 Feb 19. doi: 10.1111/jcpe.13789. Epub ahead of print. PMID: 36802083.
Other references
Dental Elf – 8th May 2015
Peri-implant mucositis: adjuncts to improve professional plaque removal
Dental Elf – 15th Jan 2016
