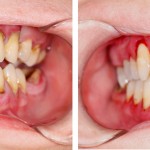
Periodontal disease is common and the standard treatment approach remains improving oral hygiene measures along with scaling and root planing (SRP). A wide range of systemic and local antimicrobial agents have been used as an adjunct to SRP over the years and previous revises have suggested a benefit. The aim of this review was to update an earlier review (Herrera et al 2002) that looked at the effectiveness of antibiotic therapy as an adjunct to SRP compared with a treatment of only SRP.
Methods
Searches were conducted in PubMed, Embase and the Cochrane Central Register of Controlled Trials (CENTRAL). This was supplemented by hand searches of the Journal of Clinical Periodontology, Journal of Periodontal Research, and Journal of Periodontology. Randomised controlled clinical trials (RCTs), controlled clinical trials (CCTs), or prospective clinical studies with a minimum of 6 months follow up were included. Studies comparing SRP to SRP with adjunctive systemic antibiotics published in English or Spanish between April 2001 and October 2013 were considered. Two reviewers independently selected studies and assessed study quality. Primary outcome measures were clinical attachment level (CAL) and probing pocket depth (PPD). Bleeding on probing (BOP) and adverse effects were secondary outcomes.
Results
- 23 RCTs were included.
- 11 of the studies were considered to be at low risk of bias 4 at moderate risk and 7 at elevated risk.
- Follow up period ranged for 6-24 months
- Intervals between visits of SRP were variable (from 24 hours to 7 weeks), as were the durations of the procedures (30 minutes to 2 hours).
- A range of antibiotics were used, amoxicillin [AM]; metronidazole [M]; azithromycin [AZ]; clarithromycin [CLAR]; doxycycline [DOX]; moxifloxacin [MOX] and ornidazole [ORN].
- A narrative summary of the results was presented.
- In most studies, the effects of antibiotic therapy adjunctive to mechanical periodontal therapy may have had a beneficial effect on the outcomes of SRP in terms of the clinical parameters CAL, PPD, and BOP.
Conclusions
The authors concluded: –
Owing to the high level of heterogeneity of the studies included in this review, the authors could not establish definitive conclusions and guidelines regarding the use of adjunctive systemic antibiotics. However, within the limitations of this review, the use of systemic antibiotics with SRP may be beneficial for specific populations. Standardized clinical disease diagnostic criteria and additional randomized controlled clinical trials are necessary to verify the effectiveness of the use of adjunctive systemic antimicrobials with SRP.
Comments
This review is an update of 2002 review by Herrera et al that included 25 studies, which also suggested that systemic antibiotics offered some additional benefit but considered that it was difficult to establish definitive conclusions. Despite a further decade of research it would appear that the findings of this new review are similar. Although this new review only considered studies published since 2001 it would have been interesting to have also included the relevant studies from the earlier review. Amoxicillin and metronidazole were the commonest antibiotics used in the studies identified (11 out of 23) and a number of previous systematic reviews have been published focused on these two antibiotics ( see Dental Elf 25th May 2012) . However, with the increasing concern regarding antimicrobial resistance whether the clinical benefit is such as to recommend their use is still in question.
Links
Garcia Canas P, Khouly I, Sanz J, Loomer PM. Effectiveness of systemic antimicrobial therapy in combination with scaling and root planing in the treatment of periodontitis: A systematic review. J Am Dent Assoc. 2015 Mar;146(3):150-163. doi: 10.1016/j.adaj.2014.12.015. Review. PubMed PMID: 25726342. [Abstract]
Herrera D, Sanz M, Jepsen S, Needleman I, Roldán S. A systematic review on the effect of systemic antimicrobials as an adjunct to scaling and root planing in periodontitis patients. J Clin Periodontol. 2002;29 Suppl 3:136-59; discussion 160-2. Review. PubMed PMID: 12787214. [Abstract]
Dental Elf 25th May 2012 – Systemic antibiotics as an adjunct to non-surgical periodontal treatment

My opinion, in most cases local therapy including lasers is better long term over systemic antibiotics. http://t.co/ObLx4NZzYk
@benyoungdds Evidence for adjunctive use of lasers with non-surgical perio treatment is poor see. http://bit.ly/1BMmTdW
@TheDentalElf studies dealing with lasers and nonsurgical periodontal therapy are currently limited. LANAP vs perio surgery studied more.
@TheDentalElf @carlopoggio If optimum mechanical debridement is not done, antibiotics are not effective. If done, you don’t need antibiotics
@perioindia @TheDentalElf: as a clinician that’s a common sense statement I do agree. Evidence however should be beyond “common sense”.
@carlopoggio The three philosophies of antibiotics: Pre-emptive philosophy, prophylactic philosophy & Therapeutic philosophy @TheDentalElf
@carlopoggio Therapeutic philosophy helps to enhance the clinical outcomes obtained from mechanical therapy, if used well. @TheDentalElf
@carlopoggio Mean Probing depth reduction & Attachment gain both improve if antibiotics targeting Gm -ve bacteria are added. @TheDentalElf
Don’t miss – Non-surgical periodontal treatment – is there a role for systemic antibiotics? http://t.co/JoAZczHYir #EBP
[…] Dental Elf – 16th March 2015 – Non-surgical periodontal treatment – is there a role fo… […]
[…] Dental Elf – 16th Mar 2015 – Non-surgical periodontal treatment – is there a role for syst… […]
[…] Dental Elf – 16th Mar 2015 – Non-surgical periodontal treatment – is there a role for syst… […]
[…] Dental Elf – 16th Mar 2015 – Non-surgical periodontal treatment – is there a role for syst… […]
[…] Non-surgical periodontal treatment – is there a role for systemic antibiotics? […]