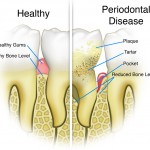
The management of periodontal disease involves stopping its progress, maintaining healthy periodontal tissues and ideally regenerating lost tissues. Where intra-bony defects exist and regenerative treatment is not indicated osseous resective surgery can eliminate defects and improve contour to facilitate oral hygiene.
The aim of this review was to assess the evidence for osseous resective surgery (ORS) in the treatment of residual periodontal defects in terms of pocket elimination and biological costs in patients with chronic periodontitis.
Methods
Searches were conducted in the Medline/PubMed, Embase and Cochrane Central Register of Controlled trials (CENTRAL) databases. This was supplemented with searches of the journals. journal of Clinical Periodontology, Journal of Dental Research, Journal of Periodontal Research, Journal of Periodontology and The International Journal of Periodontics and Restorative Dentistry.
Retrospective studies, case–control studies, case series, randomized controlled (RCT) and non-randomized controlled (non-RCT) published in English investigating the clinical efficacy of ORS without or with fibre retention technique for the treatment of intrabony defects were considered. Two reviewers independently selected studies extracted data and conducted a risk of bias assessment. RCTs were assessed using the Cochrane Tool. A random effects meta-analysis was carried out.
Results
- 4 RCTs (2 split-mouth RCTs) involving a total of 96 patients were included.
- 3 studies were considered to be at low risk of bias and 1 at high risk of bias.
- 3 studies contributed to the meta-analysis;
- Percentage of pocket elimination (PD ≤ 4 mm) 12 months after osseous resective surgery = 98.3% (95%CI; 96.8 – 99.7)
- Weighted mean amount of resected bone was 0.87mm (95%CI; 0.49 -1.25).
- Weighted mean increase in gingival recession was 2.13mm (95%CI; 1.49 – 2.78) at 12 months.
- 4 studies reported on patient pain experienced during surgery and early postoperative weeks.
Conclusions
The authors concluded: –
ORS represents an effective surgical approach for the elimination of residual periodontal pockets in the short to medium term. Additional randomized controlled clinical trials with data on pocket elimination are warranted.
Comments
3 major databases and a number of relevant journals were searched for the review although restricting the inclusions to English language publications may have excluded relevant studies. Only a small number of small RCTs were included although they all provided data for 12 months follow up. Two of the included studies were from the same group. The primary outcome reported was the percentage of pockets with PD ≥ 5 mm converted to PD ≤ 4 mm. This was considered to ‘suggestive of clinical stability and long-term tooth maintenance’ by the authors. While this review suggests some benefit from ORS the small number of small studies included in the review and meta-analysis (45 patients and 80 sextants) means that the findings should be interpreted cautiously. Additional high-quality well-reported RCTs are needed.
Links
Primary Paper
Ferrarotti F, Giraudi M, Citterio F, et al. Pocket elimination after osseous resective surgery: A systematic review and meta-analysis. J Clin Periodontol. 2020;47(6):756-767. doi:10.1111/jcpe.13281
Other references
Dental Elf – 11th Dec 2019
Periodontal surgery: Is a minimally invasive approach effective for infrabony defects?
