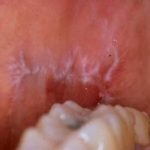
Oral lichen planus (OLP) is a chronic, inflammatory, mucocutaneous disorder associated with cell-mediated immune system dysfunction. It affects between 0.5-2.0% of the population more frequent in women. Diabetes Mellitus (DM) is a metabolic and chronic disorder characterized by an increase of the blood concentration of glucose resulting from a defect in insulin secretion, insulin action, or both with a global prevalence of about 8.8%. A relationship between OLP and DM was described in the 1960s and a number of subsequent studies have suggested an association.
The aim of this review was to assess the relationship between oral lichen planus and diabetes mellitus.
Methods
Searches were conducted in the PubMed/Medline and Scopus databases. Case control or prevalence studies published in English and evaluating the prevalence of DM in patients with OLP or the prevalence of OLP in patients with DM were considered.
Three reviewers independently selected studies. Data was abstracted, and study quality assessed using the Oxford Centre for Evidence‐Based Medicine (OCEBM) Levels of Evidence. Pooled estimates were analysed using a random effects model.
Results
- 22 studies were included.
- 12 studies (8 prevalence; 4 case-controls) considered the prevalence of DM in OLP patients.
- 4 (of 12) found a statistically significant association between DM and OLP.
- The prevalence of DM ranged from 1.6% to 37.7%.
- Meta-analysis of 4 case-controlled studies found relative risk (RR) = 2.432 (95%CI; 0.953 to 6.205).
- 10 case-controlled studies considered the prevalence of OLP in DM patients.
- 2 (of 10) reported a statistically significant association.
- The prevalence of DM ranged from 0.5% to 6.1%.
- Meta-analysis of 4 case-controlled studies found relative risk (RR) = 1.453 (95%CI; 0.876 to 2.408).
Conclusions
The authors concluded: –
This review found contradictory results when analysing the relationship between OLP and DM and the possible clinical–pathological differences in OLP among patients with DM. This discrepancy may be due to the heterogeneous criteria in the diagnosis of OLP and DM, different selections of age, sex, and type of DM. These factors should be considered when studying this association for a correct interpretation of the results. Considering the high prevalence and morbidity associated with DM, new case–control studies are of great interest.
Comments
The authors of this review have searched a limited number of databases and restricted their search to English language only studies so there is the potential to have excluded some relevant studies. They have also chosen to use the OCEBM Levels of Evidence to assess study quality when the Newcastle-Ottawa Scale would have been a more appropriate choice. The authors also highlight potential issues with the variation in diagnostic criteria for both diseases with some of the included studies not reporting the diagnostic methods for DM. While both meta-analysis suggest a relationship the confidence intervals cross the line of no effect so are not statistically significant. Higher quality and better conducted and reported studies are needed to assess the relationship between diabetes and OLP.
Links
Primary Paper
Otero Rey EM, Yáñez-Busto A, Rosa Henriques IF, López-López J, Blanco-Carrión A. Lichen planus and diabetes mellitus: Systematic review and meta-analysis. OralDis. 2018 Sep 11. doi: 10.1111/odi.12977. [Epub ahead of print] Review. PubMed PMID: 30203902
Other references
Dental Elf – Oral Lichen Planus blogs
Photo credits
By James, Candice, Mai – http://bohone09.wikispaces.com/Group+1, CC BY-SA 3.0,
