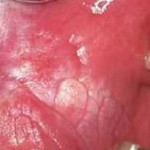
Oral squamous cell carcinoma (OSCC) is the most common type of oral cancer and is a major health burden with a 50% overall 5-year survival rate (Dental Elf – 29th Jun 2020). Oral potentially malignant disorders (OPMD) are a group of conditions that may progress to oral cancer (Dental Elf – 24th Aug 2020). Early detection and management of these lesions are crucial to improve survival rates and prevent oral cancer progression.
Current practice for the detection of OMPD involves a conventional oral examination under white light and biopsy of suspicious lesions. The decision to biopsy is based on the findings of the examination, however conventional oral examinations have been shown to be a poor predictor of oral squamous cell carcinoma and oral epithelial dysplasia (OED).
Optical fluorescence imaging (OFI) has been shown to have poor diagnostic yield for OSCC and OED and based on the published evidence, the American Dental Association have recommended against the use of auto fluorescence imaging for clinically detected lesions. However, adjunctive OFI has been demonstrated to provide more clinical information to the practitioner such as lesion detection, assessment and management than by clinical examination alone. Therefore, the aim of this systematic review was to provide evidence on the efficacy of direct OFI as an adjunctive to clinical oral examination in the evaluation and management of OPMD and OSCC.
Methods
This review was performed in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA). Database searches were conducted in Medline, Web of Science, Embase and Scopus using a combination of MESH terms. Studies needed to evaluate and report the efficacy of both clinical oral examination and OFI for OPMD, OSCC or OED (or provide enough data for the efficacy to be calculated).
The primary outcome measures focused on evaluating the efficacy of OFI in clinical evaluation, risk assessment or management of OPMD and/or OSCC. Secondary outcomes were the efficacy of OFI as an adjunct to clinical oral examination in general dental practice and its value in long term surveillance of OPMDs. Risk of bias was assessed using the QUADAS-2 tool.
Results
- 78 full text articles were assessed for eligibility and 27 studies met the inclusion criteria.
Auto fluorescence in the clinical evaluation of OMPD and OSCC
- 15 studies reported efficacy on the detection of OMPD and/or OSCC with significant heterogeneity and risk of bias reported in the methodologies used. 3 studies demonstrated a low risk of bias.
- Two studies assessed the efficacy of VELscope as an adjunct to clinical oral examination with both studies demonstrating higher sensitivity but lower specificity values.
- On study assessed the efficacy of Identafi’s multispectral light which demonstrated equivalent accuracy to clinical oral examination with the extra-oral LED white light. The violet auto florescence light alone demonstrated low sensitivity and specificity for the detection of OPMD and/or OSCC.
Auto fluorescence for visualisation of oral mucosal lesions
- Auto fluorescence for the visualisation of oral mucosal lesions was reported by 8 studies of which 3 had a low risk of bias.
- 6 studies reported additional lesion detection with auto fluorescence compared to clinical oral examination alone.
Auto fluorescence as an adjunctive tool to clinical oral examination
- A large range in efficacy values were reported for adjunctive OFI in detected OPMD/OSCC across 7 studies (sensitivity: clinical oral examination vs auto florescence as an adjunct: 17-99.2% vs 73.9-100%; specificity: 33.3-99% vs 38-97.9%).
Discrimination of benign oral lesions from dysplastic or cancerous lesions
- 21 studies reported efficacy on OFI in discriminating between benign, dysplastic and neoplastic oral lesions. Significant heterogeneity and variation in reported efficacy were noted (clinical oral examination alone: sensitivity 5.9-96.6%, specificity 42.9-97.8%, OFI alone: sensitivity 30-100%, specificity 12.5-93%, combined examination: sensitivity 46-100%, specificity 6-74%).
- An overall reduction in specificity was noted when OFI was utilised (alone or as an adjunct) compared to clinical oral examination.
Secondary outcomes
- One study with a low risk of bias assessed auto fluorescence examination as an adjunctive tool to clinical oral examination in general dental practice. This study informed higher sensitivity values with a reduction in specificity compared to clinical oral examination alone for the detection of oral mucosal lesions
Conclusions
The authors concluded: –
There is promising evidence for the use of adjunctive OFI to clinical oral examination in varying aspects of clinical practice, contributing to the overall improvement in patient management.
Comments
This systematic review provides insight into the role optical fluorescence imaging as an adjunct to clinical oral examination for the detection of oral mucosal lesions including oral potentially malignant disorders and oral squamous cell carcinoma. The included studies demonstrated substantial heterogeneity which likely precluded quantitative analysis. The authors reported the overall sensitivity increased and specificity decreased for the detection of lesions using optical fluorescence imaging. It is of note that different optical fluorescence imaging systems were used and the majority of included studies were at high risk of bias. The included studies had a range of sample sizes and the majority were in specialist centres. Therefore, there may be a spectrum of bias towards disease. This has implications for how optical fluorescence may be used in the future as if used in primary care, there is likely to be a lower prevalence of suspicious lesions; hence sensitivity and specificity may be further reduced. One of the authors was lead author on several papers included in this systematic review however no measures of bias mitigation were reported in the methodology. Overall, this review provides support for a larger study to conclude the efficacy of the use of optical fluorescence imaging as an adjunct to clinical oral examination for the detection of oral mucosal lesions however no change in clinical practice can be recommended from this review.
Links
Primary paper
Tiwari L, Kujan O, Farah CS. Optical fluorescence imaging in oral cancer and potentially malignant disorders: A systematic review. Oral Dis. 2020 Apr;26(3):491-510.
Dental Elf – 24th August 2020
Human Papilloma Virus in oral potentially malignant disorders
Dental Elf – 29th June 2020
Elective neck dissection versus observation for T1-2 oral squamous cell carcinoma
