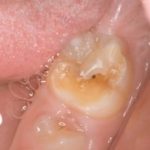
Molar incisor hypomineralisation (MIH) can be defined as damage that occurs due to alteration in the transition or maturation stage of amelogenesis or the secretion stage. It is a developmental defect of enamel, affecting one to four first permanent molars and frequently permanent incisors (Dental Elf – 18th November 2016). MIH-affected enamel has altered mechanical properties such as weaker hardness, modulus of elasticity and bond strength (Dental Elf – 26th June 2020). Its prevalence has been reported to range between 0.5-40% with a mean global incidence of 17.6 million people in 2016 (Dental Elf – 8th September 2017; Dave and Taylor, 2018).
Recently, the terms Deciduous Molar Hypomineralisation (DMH) and Hypomineralised Secondary Primary Molar (HSPM) have been used which refer to the same type of enamel defect – idiopathic hypomineralisation affecting 1- to 4- deciduous molars. The prevalence of HSPM has been reported at 11.17%.
There is overlapping of the mineralisation of the second deciduous molars and the first permanent molars, hence aetiological factors of MIH may be the same as those of HSPM. Therefore, the aim of this systematic review was to review the aetiological factors of the relationship between drugs and HSPM and evidence on the association between HSPM and drug use during pregnancy and first year of life.
Methods
This systematic review was conducted in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) statement. Searches were conducted in PubMed, Pharmaceutical News Index, MedLine, Embase and Medes using keywords related to enamel defects, hypomineralisation and deciduous molars combined with the terms ‘drugs’, ‘pregnancy’ and ‘primary dentition’. Study inclusion was undertaken in three stages; (1) title review, (2) abstract review and (3) full article review. Two authors independently conducted the three selection stages with involvement of a third author to help reach consensus if there were disagreements. Moreover, a hand search of the reference lists was conducted to identify studies not found in the initial search. There were no restrictions on languages. Animal studies, case reports, pilot studies, editorials, letters and literature reviews were excluded. Only studies that described the relationship between HSPM and drug administration during pregnancy or the first year of life were included.Data were extracted for pre-determined factors and quality assessment undertaken with the Newcastle-Ottawa Quality Assessment Scale.
Results
- 7 articles were included for review comprising 2 case-control, one cross-sectional and 4 cohort studies.
- Quality assessment using the Newcastle-Ottawa Quality Assessment Scale demonstrated that all studies included were high quality.
- One study was conducted in the USA and the rest in Europe. Not all studies used the terms DMH or HSPM.
- Heterogeneity was demonstrated in the assessment of enamel defects through indexes from the Modified Developmental Defects of Enamel Index, Modified Tooth Surface Index of Fluorosis whilst two studies did not use an index.
- 4 studies reported data on drug consumption during pregnancy and possible enamel defects in the primary dentition. Two studies specified the weeks of pregnancy in which drug use began (specifically from early pregnancy (<18 weeks)).
- Antibiotics – One study reported the ingestion of amoxicillin from 6 weeks to 3 months and from 3 to 6 months significantly increased the risk of fluorosis in the second primary molars. Another study reported no significant differences in prevalence of children with and without DMH with antibiotic consumption in the first year of life.
- Antiepileptic drugs – One study reported that the number of children with more than 2 teeth with white opacities, more than one tooth with diffuse opacities or with more than one tooth with hypoplasia was significantly higher amongst children exposed to antiepileptic drugs during the gestational period. There were no significant differences in the appearance of yellow opacities.
- Antihistamines and anti-asthma drugs – There were no associations with an increase in DMH.
- Folic Acid – The prevalence of children with DMH was significantly higher (than children without DMH) in pregnant women who began to consume folic acid periconceptionally and in those who started in the first 10 weeks of gestation.
- Chemotherapy – A report of 3 patients treated with myeloablative preparative therapy and autologous stem cell transplantation for neuroblastoma showed all patients having defects in the enamel in their primary dentition.
- Renal medication – 2 studies reported an association between renal failure (and its associated medications) with hypoplasia of primary teeth, especially the primary canines. Enamel opacities were also reported.
Conclusions
The authors concluded: –
…Although all the studies selected in this systematic review were of high quality, there were few of them, and the kind of drug used varied widely. We found no clear evidence that the use of drugs during pregnancy and during the first year of life is associated with second primary molar hypomineralisation. More studies, especially prospective and controlled studies, are required to analyse this relationship…
Comments
There is considerable heterogeneity in the included studies that has preluded quantitative analysis and the ability to draw conclusions on prevalence of DMH or HSPM and specific drugs with respective to relative risk. The findings of this systematic review are not sufficient to change clinical practice. Nonetheless, significantly increased rates of DMH and HSPM were reported in several of the included studies in association with certain drugs hence this review identifies a future area for research.
Links
Primary paper
Serna Muñoz, C., Ortiz Ruiz, A. J., Pérez Silva, A., Bravo-González, L. A. & Vicente, A. (2020) Second primary molar hypomineralisation and drugs used during pregnancy and infancy. A systematic review. Clin Oral Investig, 24(3), 1287-1297.
Other references
Dave, M. & Taylor, G. (2018) Global prevalence of molar incisor hypomineralisation. Evidence Based Dentistry, 19, 78.
Dental Elf – 18th Nov 2016
Dental Elf – 26th June 2020
Molar-Incisor Hypomineralisation: Bonding to Adhesive Materials
Dental Elf – 8th September 2017
