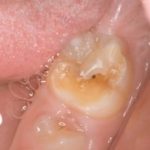
Molar incisor hypomineralization (MIH) is a developmental condition leading to enamel defects in first permanent molars and permanent incisors. In Europe its prevalence is reported to lie between 3-22%. Management of MIH can be difficult as a broad spectrum of clinical presentations are seen with enamel breakdown hypersensitivity and pain.
The main aim of this review was to assess which treatments for molar-incisor hypomineralization (MIH) have been evaluated in clinical studies and how well they performed.
Methods
Searches were conducted in the Medline, Embase, Cochrane Central Google Scholar and OpenGrey databases. Retrospective or prospective, controlled trials or cohort studies of treatment of MIH with a minimum of 10 cases were considered. The primary outcomes was treatment ‘success’, i.e. did not require further (restorative, endodontic, surgical) interventions.
Two reviewers independently selected studies, abstracted data and assessed study quality. The Newcastle-Ottawa scale (NOS) was used to assess study quality. A narrative summary was and pooled annual failure rates were presented.
Results
- 14 studies were included
- 10 studies (4 prospective cohorts,4 retrospective cohorts, 2 RCTs) related to MIH-affected molars involving 381 patients and 720 teeth.
- 4 studies (2 prospective cohorts,2 RCTs) related to MIH-affected incisors involving 139 patients and 274 teeth.
- For molars, remineralization, restorative or extraction therapies had been assessed.
- For restorative approaches, mean (SD) annual failure rates were highest for fissure sealants (12 [6]%) and glass-ionomer restorations (12 [2]%), and lowest for indirect (1[3]%) and composite restorations (4 [3]%) and preformed metal crowns (3%/one study).
- One study assessed extraction of molars in young patients (median age 8.2 years), the majority of them without malocclusions, but third molars in development. Spontaneous alignment of second molars was more frequent in the maxilla (55%) than the mandible (47%).
- For incisors, desensitizing agents successfully managed hypersensitivity. Micro-abrasion and composite veneers improved aesthetics.
Conclusions
The authors concluded
a limited number of mainly observational studies investigated treatment options for MIH. For molars, non-invasive and invasive/restorative options are available; the indication for which should be based on the severity of MIH and hypersensitivity. If restorations are needed, composites, preformed metal crowns or indirect restorations seem suitable. Prior to tooth extraction as last resort factors like the presence of a general malocclusion, patients’ age and the status of neighbouring teeth should be considered. No clear recommendations can be given for MIH incisors. Future studies should aim for high internal and external validity, follow- up patients for longer time periods and use outcomes relevant to patients, providers, and public services.
Comments
While a broad search strategy was conducted only a small number of small studies could be included in this review. These studies were few in number and small in size. The authors themselves noted that the included studies were mainly observational and prone to risk of bias with most studies not randomly allocating treatments. They also highlight that, as the studies were mainly from specialists centres and used techniques not common to general practice that the findings may not be generalisable. The limited quality of the available studies mean that the findings of this review need to be interpreted with caution and more high quality studies are needed in order to understand the best approaches for managing MIH.
Links
Primary paper
Elhennawy K, Schwendicke F. Managing molar-incisor hypomineralization: A systematic review. J Dent. 2016 Sep 28. pii: S0300-5712(16)30188-9. doi: 10.1016/j.jdent.2016.09.012. [Epub ahead of print] Review. PubMed PMID: 27693779.
Other references
Original review protocol on PROSPERO
Dental Elf -3rd May 2016
Dental Elf -2nd May 2016
Molar incisor hypomineralisation- review suggests link with childhood illnesses

Molar-incisor hypomineralisation https://t.co/Kr8kEepD0z
Molar-incisor hypomineralisation management https://t.co/nb9x0aY0zd
Limited evidence for molar-incisor hypomineralisation management https://t.co/nb9x0aY0zd
Treatment options for molar-incisor hypomineralisation-only limited observational studies? https://t.co/nb9x0aGpaD
Molar-incisor hypomineralisation little high quality evidence for treatment options https://t.co/nb9x0aY0zd
Don’t miss – Molar-incisor hypomineralisation management https://t.co/nb9x0aY0zd