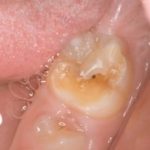
Molar incisor hypomineralisation is a developmental defect of enamel, affecting one to four first permanent molars and frequently permanent incisors (Dental Elf -18th November 2016). Its prevalence has been reported to range between 0.5-40% with a mean global incidence of 17.6 million people in 2016 (Dental Elf – 8th September 2017; Dave and Taylor, 2018; Schwendicke et al., 2018).
Microscopically, the enamel has a less dense prismatic structure with loosely arranged apatite crystals and a significantly reduced mineral density (Crombie et al., 2013). As a consequence, MIH-affected enamel has altered mechanical properties such as weaker hardness, modulus of elasticity and bond strength with resin composite (compared to sound enamel). Restorative intervention is 11-fold higher in children with MIH, and sealants and restorations need three times more re-treatment in comparison to those on children without MIH (Kotsanos et al., 2005).
Therefore, the aim of this study was to conduct a systematic review on bonding of adhesive materials to MIH affected enamel to identify and determine the best bonding protocols.
Methods
Searches were conducted in Medline/PubMed, The Cochrane Library, Web of Science and reference lists of selected papers. The keywords were related to MIH and combined with keywords for bonding. The searches were kept broad including no limitations on languages and the inclusion of laboratory and clinical studies. Case reports/series and animal studies were excluded.
Two reviewers independently screened the abstracts and titles for inclusion into the study and also extracted the data. Quality assessment included a risk of bias assessment and a narrative summary was provided. Meta-analysis was not conducted due to the heterogeneity between the included studies.
Results
- 10 studies were included comprising 6 laboratory studies and 4 clinical studies.
- All 4 clinical studies were prospective (of which 3 were randomised).
- 4 studies had a low risk, 4 had a medium risk and 2 had a high risk of bias.
- 9 studies reported a significantly reduced bond strength with MIH-affected enamel compared to sound enamel.
- 3 laboratory studies reported higher cohesive failures in hypomineralised enamel or MIH-affected enamel.
- One clinical study reported on two cavity designs for resin composite, an invasive treatment approach with removal of all affected enamel to obtain margins in sound enamel and a non-invasive treatment with removal of affected enamel until the bur met significant resistance from the hypomineralised enamel. The restoration success rate at 24 months of non-invasive treatment was significantly lower compared to the invasive treatment.
- Severity of hypomineralisation (assessed by the colour of enamel) had no significant effect on bond strength for composites or sealants.
- There was a significantly higher bond strength with an etch and rinse adhesive compared to a self-etch adhesive and a universal adhesive after etching. However, there were no significant differences in success rates at 18 months between etch and rinse and the self-etch adhesives.
- In 2 laboratory studies, the application of sodium hypochlorite after etching significantly increased bond strength to MIH-affected enamel (regardless of severity). In contrast, one study reported that sodium hypochlorite did not enhance enamel bonding. Clinically, one study found a significantly higher survival rate at 24 months of resin composites when using sodium hypochlorite on MIH-affected enamel.
- There was poor penetration with Icon® infiltration on MIH-affected enamel. One study reported no significance differences in bond strength (with additional use of sodium hypochlorite) however, another study did report significantly higher bond strengths when sodium hypochlorite was used.
Conclusions
The authors concluded: –
…bond strength of composite to MIH-affected enamel was not significantly different when using self-etch compared to etch-and-rinse adhesives; deproteinization after etching for etch-and-rinse adhesives seemed to enhance bond strength; resin infiltration showed an erratic penetration; however, a preliminary deproteinization after etching could improve bond strength; and regarding sealants, a study reported no significant differences in retention rate, whereas another recommended to previously apply an adhesive…
Comments
A broad search strategy was used to maximise study inclusion however only a few clinical and laboratory studies were included. The risk of bias varied between low, medium and high risk and the investigations within each study varied making direct comparisons challenging (hence, no meta-analysis was conducted). The findings of this systematic review are not sufficient to change clinical practice. The authors acknowledge that given the variability of MIH severity and small number of included studies, the findings from this review need to be interpreted with caution. Children with MIH have higher reported levels of restorative treatment need and failure of bonding to affected teeth. This review identifies a future direction for research design in improving our understanding of material bond strengths to MIH affected teeth and their longevity, helping inform clinical decision making.
Links
Primary paper
Other references
Dental Elf – 18th November 2016
Dental Elf – 8th September 2017
