
Before we start I have to disclose I am a great believer in cognitive behavioural therapy (CBT) delivered using digital technology. I have sat through many clinics seeing patients over and over again who were in what felt like a perpetual holding pattern waiting for psychotherapy and never quite getting it, in spite of my many referral letters. In fact, this got to be so frustrating that I started a company that develops applications to deliver these and other types of non-pharmacological treatments. The need for therapy is such that there is no other way to reach the millions that need it.
Fairburn and Patel (2014) discuss the methods to disseminate psychological treatments globally and come to the conclusion that computerised self-delivered or facilitated treatments are one of the key ways to reach all of those who need it and the only method that really scales.
Internet cognitive behavioural therapy (iCBT) has been shown to be effective (Andersson and Cuijpers, 2009), and it can scale up with minimal resources, but the key question has remained whether iCBT can get participants to complete the treatment.
To answer this question van Ballegooijen and colleagues undertook a meta-analysis of studies investigating face to face and internet based CBT for depression looking in particular at treatment completion and length of treatment for those that discontinue it (Ballegooijen et al. 2014).

One of the benefits of iCBT is that it can be delivered almost anywhere.
Methods
The authors primarily examined www.evidencebasedpsychotherapies.org an existing database that aims to list all trials for psychological treatments for depression. According to the authors the database was current as of January 2013. They identified 14,164 abstracts from 4 major databases. They also looked into PhD theses, but it is not clear how they did this. They stated that they did not seek out other unpublished studies due to time constrains.
For the meta-analysis they included studies on CBT among depressed adults (18+ years). These adults either had gone through a diagnostic interview or scored above cut-off on a validated symptom scale. They included studies where one arm was either CBT or iCBT but the iCBT had to have a coaching component by telephone, email or some means of communication, completely self-administered therapy was not included. The authors also excluded studies where depression was co-morbid with other conditions and studies published before 2000 as that is when research on iCBT started. They also excluded studies which combined therapy with medication and studies on group CBT. They only looked at community studies where participants had been recruited through advertising rather than through clinical services.
Coding
The main outcome was average number of sessions/modules completed by participants divided by the total number of sessions. Where authors defined ‘completion’ as going through a number of sessions lower than the specified maximum number that was the number used in the above calculation. The authors state that this could overestimate completers in the CBT condition. Two raters independently carried out data extraction.
Quality assessment
As efficacy outcomes were not analysed, the authors only carried out quality assessment on how completion of sessions was recorded and how missing data were dealt with. Two independent raters did the quality assessment and they resolved disagreements through discussion.
Meta-analysis
The authors assessed heterogeneity using the I2 statistic and a random effects model. Each outcome measure was pooled within the face to face and iCBT subgroups and the final analysis was done using a mixed effects model with fixed effects for the analysis within the subgroups and random effects for the between subgroups analysis.

The reviewers found 24 studies to include in their meta-analysis.
Results
After running through the exclusion criteria the authors identified 24 papers describing 26 treatment conditions and extracted 14 treatment conditions for face to face CBT and 12 for iCBT. There were no papers comparing iCBT with CBT directly.
- CBT ranged from 12 to 28 sessions and iCBT interventions consisted of 5 to 9 sessions
- CBT participants completed on average 83.9% of their treatment, which did not differ significantly from participants in guided iCBT who completed 80.8%
- The percentage of completers was significantly higher in CBT (84.7%) compared with iCBT (65.1%, P = .001)
- The percentage of completers of 80% or more of the intervention was significantly higher in CBT (85.2%) compared with iCBT (67.5%, P = .003)
- Non-completers of face-to-face CBT completed on average 24.5% of their treatment, while non-completers of guided iCBT completed on average 42.1% of their treatment.
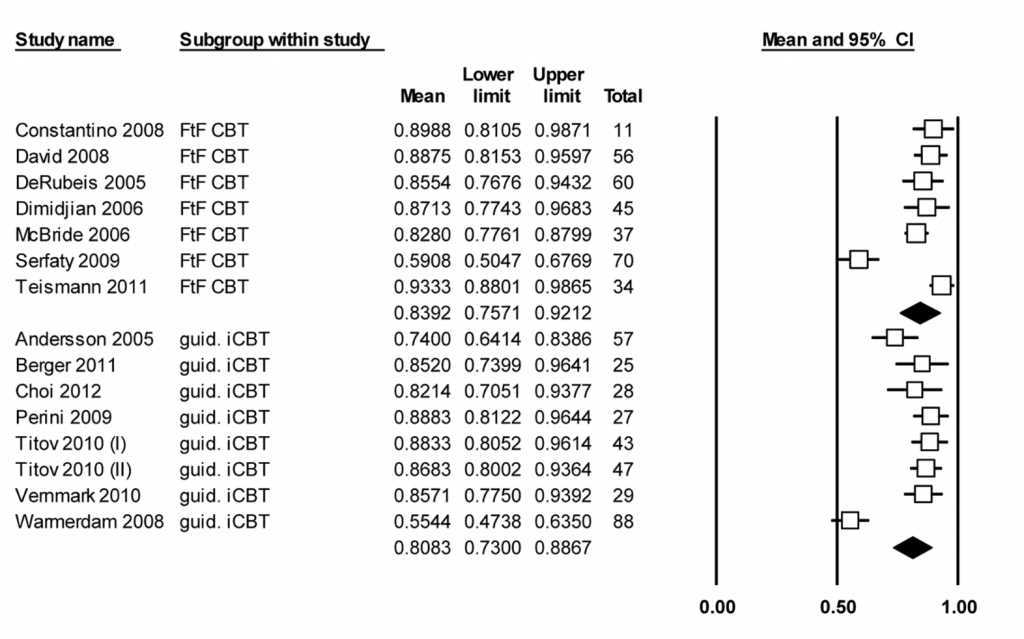
Fig 1: the distribution of average percentage (and 95% confidence interval) of completed sessions per study group.
Discussion
The study focused on adherence to guided iCBT as compared to face to face CBT. The authors chose guided iCBT as opposed to unguided on the presumption that guided CBT yields better results and better treatment adherence (Andersson and Cuijpers 2010; Richards and Richardson 2012).
However, when directly comparing guided and unguided iCBT in the same trial, the intervention rates of adherence did not differ greatly (Berger et al. 2011). The study was not designed to look at adherence so it may have been underpowered, but it may be that adherence is more related to study population or intervention design.
In most trials of iCBT (guided and non-guided) reasons for discontinuation are usually not reported and there is no analysis on what factors may contribute to greater adherence within the intervention itself or intrinsic to the participants. There is also one study that suggested participants in an unguided programme dropped out because they had recovered.
Limitations
- The studies included were very heterogeneous (various designs, lengths of treatment and definitions for ‘completion’) and there were no studies directly comparing guided iCBT with face to face CBT.
- The final number of studies was small and while there was a difference in the main outcome measured it did not reach significance. This might have been because the meta-analysis was underpowered.
- Having said this, the authors’ choices when coding completion in face to face CBT, may have resulted in artificially higher completion rates in that group.

The results of included studies were combined, despite their heterogeneity.
Conclusions
After reading this study I believe guided iCBT offers lower adherence than face to face CBT judging by the percentage of 100% and 80% completers. Interestingly, the average number of completed sessions was similar in both groups, which seems to be explained by the percentage completed by those who did not finish the treatment, which was higher in the guided iCBT group.
Investigation into what can be done to re-engage after discontinuation in guided iCBT (and non-guided) might be a fruitful line of research.
There was no economic analysis accompanying the meta-analysis but it is safe to assume that the cost of delivering guided iCBT is lower than that of CBT.
We need to focus on what specific adherence mechanisms result in better outcomes and we need to produce more studies comparing guided and unguided iCBT and also direct comparisons between CBT and iCBT.
I believe this method still holds much promise. The efficacy of iCBT is fairly well established by now with the caveat that people going through it need to complete it to benefit. We need to focus on what specific strategies can maximise adherence, particularly to non-guided iCBT as it is likely to be the most scalable method of reaching the maximum number of people at the lowest cost.

How close are we to delivering iCBT at scale for whole populations?
Links
van Ballegooijen W, Cuijpers P, van Straten A, Karyotaki E, Andersson G, et al. (2014) Adherence to Internet-Based and Face-to-Face Cognitive Behavioural Therapy for Depression: A Meta-Analysis. PLoS ONE 9(7): e100674. doi:10.1371/journal.pone.0100674
Andersson G, Cuijpers P (2009) Internet-based and other computerized psychological treatments for adult depression: a meta-analysis. Cognitive Behavioural Therapy 38: 196–205 [PubMed abstract]
Berger T, Hammerli K, Gubser N, Andersson G, Caspar F (2011) Internet based treatment of depression: a randomized controlled trial comparing guided with unguided self-help. Cognitive Behaviour Therapy 40: 251–266 [PubMed abstract]
Clarke G, Kelleher C, Hornbrook M, Debar L, Dickerson J, et al. (2010). Randomized effectiveness trial of an Internet, pure self-help, cognitive behavioral intervention for depressive symptoms in young adults. Cognitive Behavioural Therapy 38: 222–234 [PubMed abstract]
Fairburn C G, Patel V (2014). The Global Dissemination of Psychological Treatments: A Road Map for Research and Practice. American Journal of Psychiatry, 171(5), pp. 495–498 [PubMed record]
Richards D, Richardson T (2012) Computer-based psychological treatments for depression: a systematic review and meta-analysis. Clin Psychol Rev 32: 329–342. [PubMed abstract]


RT @Mental_Elf: The Internet Therapist: adherence to Internet CBT compared to face to face CBT http://t.co/FzIM6G1iDX
Kirsten Corden liked this on Facebook.
Amanda Collins-Eade liked this on Facebook.
The Mental Elf liked this on Facebook.
Lisa Eden liked this on Facebook.
Today @AndrFon on recent meta-analysis comparing adherence to Internet CBT vs face-to-face CBT for depression http://t.co/XHM4tQ2Azk
Andy Conway liked this on Facebook.
Morning @heleenriper We’ve blogged about your @PLOSONE CBT meta-analysis http://t.co/XHM4tQ2Azk Any thoughts?
@Mental_Elf @heleenriper @PLOSONE : what About this? #PersuasiveTechnology http://t.co/5dlbLHV9wW
Hi @BigWhiteWall1 @jennyhyatt Check out our blog today on iCBT vs CBT for depression http://t.co/XHM4tQ2Azk by @AndrFon
Interesting read from the Internet Therapist re adherence to Internet CBT compared to face to face CBT http://t.co/k7ME2M6Fkd
One for @adiemusfree and others…. Adherence to Internet CBT compared to face to face CBT http://t.co/m6Pk20yUBU
Do people complete internet CBT as readily as those receiving face2face CBT?
http://t.co/pnfJ8IcP3L
Face-to-face CBT has higher adherence rates than guided iCBT for people with depression, according to new review http://t.co/XHM4tQ2Azk
Adherence to Internet CBT (Cognitive Behavioral Therapy) compared to face-to-face CBT- http://t.co/C0unNURUcI
How close are we to delivering iCBT at scale for whole populations? http://t.co/XHM4tQ2Azk
“@Mental_Elf: How close are we to delivering iCBT at scale for whole populations? http://t.co/73VdSnQPUy” good to start review with belief?
@suzypuss @Mental_Elf OMG its awful with a therapist, the th’ht of it2 masses via Internet,doesn’t bear thinkin about pity can’t add towater
Mental Elf: The Internet Therapist: adherence to Internet CBT compared to face to face CBT http://t.co/Mhhq7JBpyK
@suzypuss Interesting. Did you think @AndrFon’s blog was critical enough of the meta-analysis he highlighted? http://t.co/XHM4tQ2Azk
@Mental_Elf @AndrFon was pleased he highlighted his own belief upfront. And he acknowledged evidence contrary to his own view.
A significant challenge for digital mental health is keeping people engaged – @AndrFon on completion of online CBT http://t.co/jSSrRYUfxN
RT @Mental_Elf: Face-to-face CBT has higher adherence rates than guided iCBT for people with depression http://t.co/VJGvISZRzC
RT @Mental_Elf: Helping people with depression stick with Internet CBT http://t.co/XHM4tQ2Azk
Interesting. RT @Mental_Elf How close are we to delivering iCBT at scale for whole populations? http://t.co/egZ8FW1LZ1
Don’t miss – The Internet Therapist: adherence to Internet CBT compared to face to face CBT http://t.co/XHM4tQ2Azk
Nicola Davies liked this on Facebook.
João Leal liked this on Facebook.
The Internet Therapist: adherence to Internet CBT compared to face to face CBT http://t.co/krlpHdGjEF via @sharethis
“Adherence to Internet CBT vs face to face CBT” http://t.co/biqQBm2RZk
The Internet Therapist: Metaanalysis looks at adherence to #Internet #CBT compared to face to face CBT http://t.co/bQQcdKXi64 via @sharethis
[…] The Internet Therapist: adherence to Internet CBT compared to face to face CBT […]
[…] The Internet Therapist: adherence to Internet CBT compared to face to face CBT The Mental Elf (Andrés Fonseca) […]
[…] The Internet Therapist: adherence to Internet CBT compared to face to face CBT The Mental Elf (Andrés Fonseca) […]
[…] computerised cognitive behavioural therapy (cCBT) in a previous blog post, looking specifically at adherence to cCBT treatment. As I did then, I have to disclose now that I am an advocate for its use and I run a company that […]