
For people who are suffering from a severe depression, antidepressants are a very effective treatment, but how they work is still not fully understood. The basic biochemistry of how one dose of the drug affects one part of the nervous system is known, e.g. increasing serotonin levels at the synapse by preventing it from being recycled into the neurons (SSRIs), but this is a far too simplistic account of what will be happening in the brain in order for these drugs to be effective. Neuroimaging offers another way to try and understand the effects of these drugs on how the brain functions at a wider level.
People who are depressed have difficulties with a number of different neuropsychological tests looking at negative and positive emotions. During a depressive episode, on average, people:
- Process negative stimuli differently:
- Pay more attention to negative emotions
- Remember negative stimuli better
- Classify neutral/ambiguous faces as negative
- Remember more negative events from the past
- Process positive stimuli differently:
- Classify positive faces as neutral
- Experience reduced pleasure from previously rewarding activities
- Struggle to regulate emotions as well, especially getting control of negative emotions
When people recover from depression these biases in their emotional processing improve a lot. Previous studies have suggested that changes in the emotion processing areas in the brain underlie this improvement (no matter what treatment is offered).

The world can look very different when we are depressed, as we process negative and positive stimuli quite differently compared to when we are well
To work out how antidepressants might be affecting the neural circuits that underlie emotional processing a researcher from Baltimore performed a meta-analysis of studies where people did an emotional processing task during an MRI scan. We have discussed meta-analyses of functional MRI studies before and there are real technical challenges combining lots of different studies using different scanners and analysis methods. Over the last couple of years most people have converged on using one technique (www.brainmap.org/ale) and this new study uses it.
Methods
A literature search found studies looking at two types of antidepressants: SSRIs (e.g. fluoxetine) and SNRIs (e.g. venlafaxine). Only studies that directly looked at the difference between taking antidepressants and not were included, i.e. studies where:
- The same person took an antidepressant and then a placebo (or vice versa) sequentially,
- A group taking an antidepressant were compared to a group taking placebo
- Comparing people before and after taking an antidepressant
Both healthy people and people experiencing depression were included to see if there are differences in how antidepressants affect their brains.
Sixty studies were included with 1,569 participants. The tasks that people performed in the scanner were broadly similar: emotional stimuli were presented to them in various different ways.
Brain imaging studies do a lot of statistical comparisons. The problem with this is that if you stick to p=0.05 for accepting/rejecting each test then you would expect 1 in 20 tiny areas of the brain to be ‘significant’ even if none of them are actually true (false positives). This study took account of this by setting acceptable error rate by using a method called the false discovery rate. This reduces the significance level of each individual test so that overall the chance of a positive finding for the whole brain not being really true (false positive rate) remains at the standard 1 in 20, or p<0.05.
Results
In people who are suffering from depression, taking antidepressants regularly:
- Decreased the response of the brain to negative emotional stimuli
- Increased the response of the brain to positive emotional stimuli
- Increased the activation of an area of the prefrontal cortex linked to emotional regulation
Figure one shows the details of where these changes took place, but in summary, areas of the brain long know to respond to emotional stimuli were affected.
Figure 1: Red indicates increased activity, blue decreased
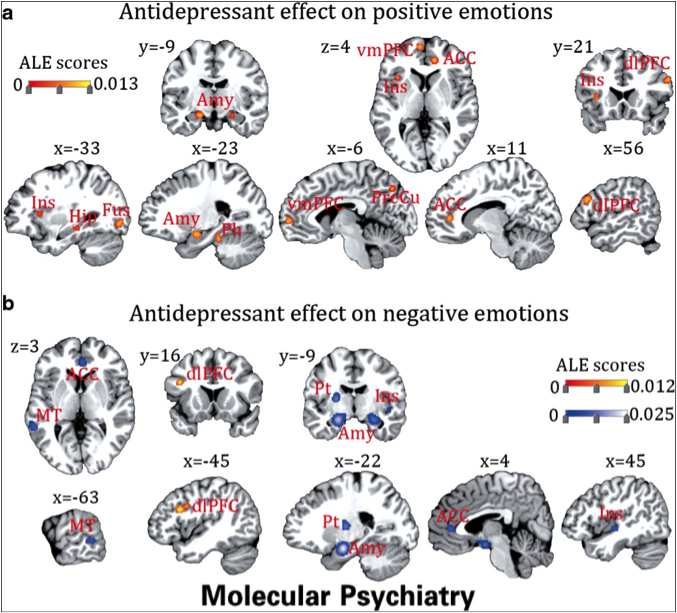
ACC, anterior cingulate; Amy, amygdala; CB, caudate body; dlPFC, dorsolateral prefrontal cortex; dmPFC, dorsal medial prefrontal cortex; Ins, insula; NAcc, nucleus accumbens; Ph, parahippocampus; Pt, putamen; rACC, rostral anterior cingulate; St, superior temporal; Th: thalamus; vlPFC: ventrolateral prefrontal cortex.
In healthy volunteers, taking antidepressants regularly:
- Decreased responses to negative emotional stimuli
- BUT a decreased response to positive emotional stimuli was found
- AND there was no effect in the prefrontal cortex
- The study showed that similar areas of the brain were affected by the drugs
One dose (usually very high) of antidepressant had a different effect:
- There were both increases and decreases to both positive and negative emotional stimuli, even within the same network within the brain
Conclusions
The author concluded:
Antidepressants act to normalize the abnormal neural responses in depressed patients through reduction of mood-congruent biases by increasing activity to positive emotions and decreasing activity to negative emotions in the amygdala, insula and anteriour cingulated, and increasing regulatory responses in dlPFC [part of the prefrontal lobe].
He also argued that the study suggests that antidepressants work primarily by altering the emotional processing biases, rather than boosting emotional regulation, and that this suggests that antidepressants and CBT could be complementary, as CBT focuses much more on emotional regulation.
Summary
- People who are depressed have well described biases in how they process emotional stimuli in the environment
- Antidepressants help to correct these biases, and this study suggests that this is the main mechanism of action
- Giving people who are depressed the space to not be focusing on negative emotions or events all the time is a powerful first step to help people make changes in their lives to sustain their recovery
- To have a sustained positive effect, antidepressants need to be taken regularly, as one-off doses have a much more mixed effect on emotional processing. This may underlie the increased agitation and anxiety that some people, but not all, experience when starting an antidepressant
- Healthy people taking antidepressants regularly may experience a reduction in the emotional reactivity of the brain

The road to recovery can be long. People need time and space to make sustained changes in their lives
Link
Ma Y. Neuropsychological mechanism underlying antidepressant effect: a systematic meta-analysis. Mol Psychiatry. 2014 Mar 25. doi: 10.1038/mp.2014.24. [PubMed abstract]


RT @Mental_Elf: Antidepressants work by changing emotional processing http://t.co/iaSb0bfKU8
Really interesting post RT @Mental_Elf: Antidepressants work by changing emotional processing http://t.co/xk82wG32Xq
The Mental Elf liked this on Facebook.
Lisa Eden liked this on Facebook.
Antidepressants work by changing emotional processing http://t.co/pqDDArIp1T via @sharethis
@andrewwatson28 on a meta-analysis looking at the neuropsychological mechanisms underlying the antidepressant effect http://t.co/3X3zjuIJuW
This article makes antidepressants sound like a cure-all. They *don’t* work for everyone, and many have significant side effects. I know from experience.
“@Mental_Elf antidepressants and CBT may have similar mode of action http://t.co/xkiCXx2d7E“
Caroline Tomes liked this on Facebook.
Antidepressants work by changing emotional processing – The Mental Elf http://t.co/v3FxoCi7Xf
Mental Elf article on new meta analysis of effects of antidepressants on emotional processing http://t.co/yrvwsjUAih via @Mental_Elf
New study looks at how antidepressants might be affecting the neural circuits that underlie emotional processing http://t.co/3X3zjuIJuW
How are antidepressant working? http://t.co/cp1m0yaxzt
João Leal liked this on Facebook.
RT @Mental_Elf: Ever wondered how antidepressants actually work? http://t.co/3X3zjuIJuW
All of which basically says that when they work (mostly they don’t by the way) anti-depressants work by lessening depression. It never ceases to amaze me how those involved in research, perhaps most especially neuroimaging, seem to confuse newly measurable *correlates” of a given condition with some kind of novel insight into its essence. Talk about not seeing the word for the trees … It still looks like we’re years off neuroimaging work actually contributing in any meaningful way to modified clinical protocols. To date, we’ve just got new ways to look at dubious medicines doing their thing
Don’t miss: Antidepressants work by changing emotional processing http://t.co/3X3zjuIJuW
@Mental_Elf @profelainefox Very interesting work; thanks for sharing. My wonderful ex-supervisor Cath Harmer does v good work in this field!
Interesting summary of fMRI showing antidepressants normalise emotional processing in depression http://t.co/Wx2wNg5pg0 via @sharethis
Candace Alexandra Price liked this on Facebook.
Kirsten Corden liked this on Facebook.
We all know now that there is no scientific proof that antidepressants have positive effects…only major side effects.
In my experience, any change of the emotional process is the result of psychotherapy.
Antidepressants work by correcting emotional biases http://t.co/MS5c6Xmq77
[…] Antidepressants work by changing emotional processing The Mental Elf (Andrew Watson) […]