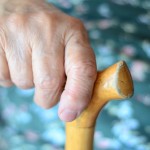
Falls are estimated to cost the NHS more than £2.3 billion per year (College of Optometrists, 2011) and are associated with significant morbidity and mortality. This fact alone should be giving us the drive to look for ways to prevent falls in healthcare settings.
A systematic review recently published in BMC Nursing (Bunn et al, 2014) is the first of its kind to evaluate the effectiveness of interventions aimed at preventing falls among older people with any form of mental illness, not just those with dementia or cognitive impairment.
The aim of this study from Bunn et al is honourable. Existing big reviews focus solely on preventing falls in older people in hospital settings, or just those with dementia or other forms of cognitive impairment (Oliver et al, 207), but this research group set out to find the interventions that could benefit those with any form of mental health problem in any setting.

This review looked for trials including older people with all kinds of mental health conditions
Methods
The researchers undertook a comprehensive literature search for both published and unpublished studies, English language, from any healthcare setting, which evaluated any intervention(s) aimed at reducing or preventing falls in people aged 60 or over, with any diagnosis of mental illness. There were no date restrictions. The two key outcomes examined were:
- Number of people sustaining at least one fall (‘fallers’)
- Total number of falls
21 studies met the inclusion criteria, 17 of which were randomised controlled trials and the remaining 4 uncontrolled trials.
Results
The authors stated their intention to address interventions preventing AND managing falls, although their results focused on prevention strategies only.
The interventions they identified varied widely, including physical activity, risk assessment, environmental modification, staff training, increased supervision, patient education and sensory interventions. Individual studies were not pooled in a meta-analysis because they were too varied, so a narrative analysis was provided instead.
Results were categorised according to location (nursing/residential care, hospital and community) as well as intervention type (single or multifactorial).
- 5 studies found a statistically significant reduction in the number of ‘fallers’ (2 of which were uncontrolled trials), interventions ranged from exercise and supervision to staff training
- 8 studies found a statistically significant reduction in the rate or total number of falls (2 of which were also uncontrolled), including interventions such as environmental adjustments, person-centred care, sensory stimulation, staff training and exercise
- Of note, 4 studies found a non-significant increase in falls with the intervention given, which were all different
However, due to the diversity of interventions studied and the variety in quality of the studies, no overwhelming evidence to be drawn in favour of any of the individual interventions.
Limitations
There were several problems with the quality of the individual studies:
- 7 of the studies did not specifically define a fall, leaving the results open to interpretation
- 1 study included syncopal falls (related to fainting or passing out)
- 1 study only included falls that needed medical attention
Less than half of the studies had a specific mental health focus. Although they all included patients with mental health problems, studies without a specific mental health focus were included as long as at least half of their participants had mental health problems.
For those identified as having mental health problems, the majority had dementia, other cognitive impairment or depression, so actually the aim to identify successful interventions relevant to other mental health problems was not met.
Looking at the review overall, the inclusion of both controlled and uncontrolled trials may have introduced a large element of bias.
Conclusions
The authors state:
Although the evidence from this review is not robust, it does challenge the American Geriatrics Society and British Geriatrics Society guideline (Martin, 2010) which states that there is insufficient evidence to support any recommendation to reduce fall risk for older people with cognitive impairment.
However, the strengths lie in the few individual studies of good quality that were included, not in the results drawn from the systematic review and there were no studies found that looked purely at mental health hospital settings, so results cannot be applied specifically to those with mental health problems.
The National Patient Safety Agency (NPSA) states:
Approaches to preventing falls must be individualised, as each patient is affected differently by the interplay between a range of risk factors.
Their report from 2007 indicates that using multifactorial interventions is an effective way to reduce the number of patient falls (Healy et al, 2007), including:
- Reviewing medication associated with a risk of falling
- Detecting and treating causes of delirium, cardiovascular illness, incontinence or urgency and eyesight problems (i.e. all those conditions that increase risk of falling)
- Providing safe footwear
- Physiotherapy, exercise and walking aids
- Consideration of the environmental layout
The NPSA acknowledges that it is uncertain if these interventions are as effective for those with cognitive impairment as for other people.
The latest NICE guidance (NICE, 2013), in addition to the above considerations, recommend also routinely asking older people about their falls history and then tailoring any interventions specifically to the patient, depending on their risk factors.
With regard to this systematic review, the researchers looked at a clearly focused question and comprehensively assessed the quality of each study, but their inclusion criteria could have been stricter and they were limited by the number of good quality, comparable studies.
This work has not identified any robust evidence to recommend specific interventions. Multifactorial interventions may be effective, but this must be refined. There is a need for better quality studies examining single interventions to determine what is actually effective at reducing falls in older people with mental health problems.
In the meantime, don’t let the poor quality evidence trip you up: find the shoe that fits your patient and tailor your approach.
Links
The importance of vision in preventing falls. The College of Optometrists & British Geriatrics Society, Jun 2011.
Bunn F et al. Preventing falls among older people with mental health problems: a systematic review. BMC Nursing, 2014;13:4.
Oliver D et al. Strategies to prevent falls and fractures in hospitals and care homes and effect of cognitive impairment: systematic review and meta-analyses. BMJ, 2007; 334 (7584):82.
Martin F. Prevention of falls in older persons. American Geriatric Society & British Geriatric Society, Jul 2010.
Healy F, Scobie S. Slips, trips and falls in hospital: The third report from the Patient Safety Observatory. National Patient Safety Agency, 2007.
Falls: assessment and prevention of falls in older people. NICE clinical guideline 161, 2013.



Are there any effective interventions for preventing falls in older people with mental health problems?: Falls… http://t.co/10lXcmLWp2
tai chi classes regularly
@Mental_Elf A walker.
@Mental_Elf Declutter the home environment #clutter #hoarding #mentalhealth
My first blog in the woodland for @Mental_Elf – looking at falls in older people with mental health problems http://t.co/0JaCAnz3F7
@Mental_Elf @anniecoops Nothing but restraint will prevent, but you can assess and manage the risk.
Falls cost the NHS £2.3 billion per year. How can we reduce the cost? http://t.co/wtvxBfgpsF
Mental Elf: Are there any effective interventions for preventing falls in older people with mental health problems? http://t.co/1tWERjzpTo
New systematic review looks at interventions aimed at reducing falls in older people with mental health problems http://t.co/wtvxBfgpsF
Last medical tweet: Review into preventing falls in Elderly patients with mental health illnesses http://t.co/rA6maBCBXC @Trisha_the_doc
RT @Mental_Elf: Are there effective interventions for preventing falls in older people with mental health problems? http://t.co/ndxmWRE3sD
Are @NICEcomms guidelines helping to prevent falls in older people? http://t.co/wtvxBfgpsF
Are there any effective interventions for preventing falls in older people with mental hlth problems? http://t.co/FhAvta2kMC via @sharethis
Do mental health problems affect the strategies we should use to prevent older people from falling? http://t.co/0PFVgFBp6V
Are there effective interventions for preventing falls in older people with #mentalhealth problems? http://t.co/WdB2odrNWM via @mental_elf
@NEPNHS What i miss in this article is evaluation of medication @Mental_Elf
If you missed the earlier flurry of tweets, my debut blog for @Mental_Elf is online today! http://t.co/7lTvTXaAT3
Recent systematic review challenges guidelines from @AmerGeriatrics and @GeriSoc http://t.co/0PFVgFBp6V
@Mental_Elf think @AmerGeriatrics @GeriSoc more likely to consider this meta-analysis on reduces falls in cog imp http://t.co/ZXvQ7goxH3
Don’t miss: Are there any effective interventions for preventing falls in older people with mental health problems? http://t.co/0PFVgFBp6V
@Mental_Elf To increase participation in specific #Balance and Stability classes that uses FaME (Falls Management Exercise) @LaterLifeTrain
@Mental_Elf @TYC_Action @NHSCTrust @publichealthni