
Aretha Franklin’s feminist soul banger ‘Respect’ was originally released by Otis Redding. In the original Redding sings that he doesn’t mind if his woman does him wrong while he’s gone, she’s sweeter than honey and he’s going to give her all his money. All he’s asking is a little respect when he gets home. Franklin’s reworked version could be interpreted: I’ve got my own money thanks, I’m not going to cheat on you and why don’t you show me some respect?
Similarly, when 90’s R&B girl group TLC sung they didn’t want ‘No Scrubs’, it was triggering for the hip hop trio Sporty Thievz who responded with a parody rebuttal ‘No Pigeons’. And who remembers Eamon’s 2003 ‘Fuck it’? (for those who don’t, it was a slow, heartbreak/medium-aggressive number about being cheated on by his girlfriend); replied to, in song form of course, by Frank’ee in the unrestrained ‘F.U.R.B’ (Fuck You Right Back). As Frank’ee rightly says at the start (before she goes on to absolutely slate his technique in the bedroom – “Fuck it, I faked it, aren’t you proud?” – and cite this as the reason for her infidelity) there are two sides to every story.
In relationships communication is key. As demonstrated above, a hit single is a good way get the message across, but for most of us a conversation is probably easier. A fairly recent sex positive movement champions open and honest conversations about relationships and sex to help promote healthy and enjoyable experiences. For example, sex and relationship blogger and influencer @Oloni would probably advise Frank’ee to stop faking her orgasms to protect her man’s ego and instead tell him what she likes and how to satisfy her… but 2003 was a different time.
Yet despite a recent overhaul to update the sex education curriculum in schools and prominent TV campaigns aiming to educate people about consent vs rape, sexual health is a topic often overlooked in mental health services. However, the sexual health of people who use mental health services is an important area to consider given evidence that suggests people with mental health diagnoses are at increased risk of sexually transmitted infections (STIs) (Hughes et al., 2016) and vulnerability to abusive relationships (Trevillion et al., 2012).
The RESPECT study aims to address this important but often overlooked area. It is a feasibility randomised controlled trial (RCT) of a sexual health promotion intervention of people with serious mental illness in community mental health services in the UK (Hughes et al, 2019; Hughes et al 2020).
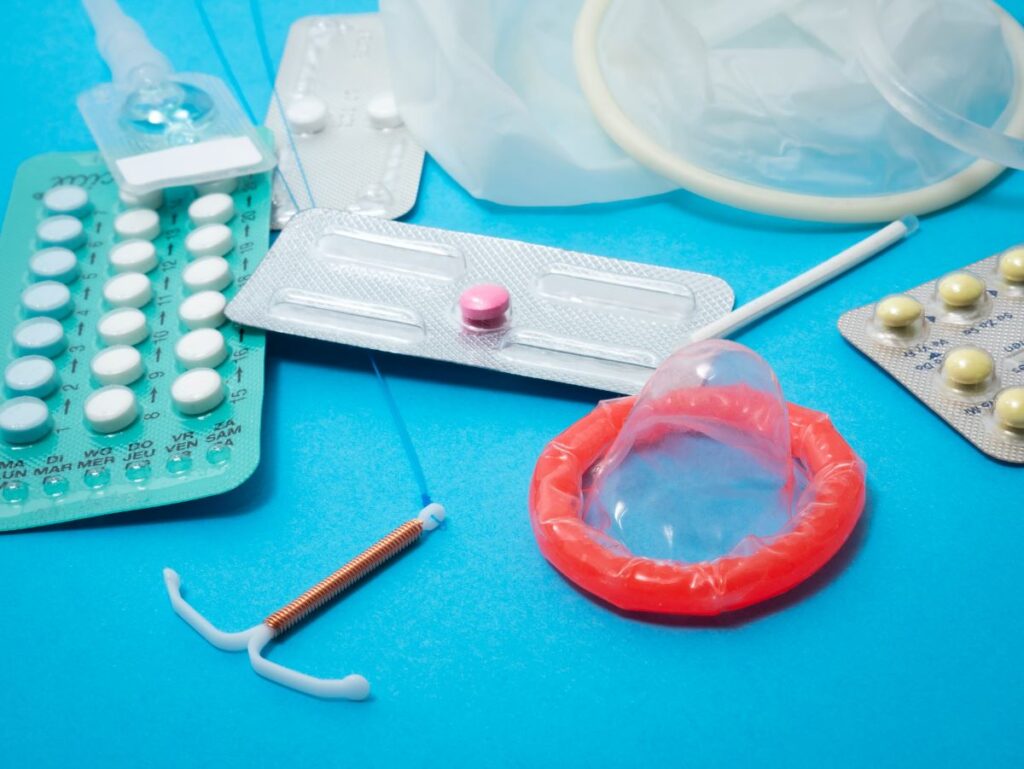
The RESPECT study aims to establish whether a sexual health promotion intervention is acceptable and feasible in UK community mental health services
Methods
This was a multi-centred, open feasibility RCT that took place in community mental health services. Participants were eligible to take part if they:
- Were receiving support from participating services
- Had a diagnosis of schizophrenia, psychosis, bipolar affective disorder, schizoaffective disorder, major depressive disorder
- Were aged 18 or over
- Were able to provide written consent.
Participants were allocated randomly to the intervention or control arm of the study. The control arm of the study was treatment as usual. So, normal mental health care plus access to sexual health services in their local area.
Participants in the intervention group received three 1-hour sessions with a specifically trained mental health worker that aimed to promote safe sexual behaviours and positive sexual relationships:
- Session 1: knowledge regarding safer sex including HIV, STI quiz, condoms and contraception and where to seek help and advice
- Session 2: Risky and less risky behaviours for HIV, pros and cons of condom use, how to use a condom, contingency planning for risky sexual situations
- Session 3: Signs of good and less good aspects of relationships, assertive communication, negotiating own needs and wishes in sexual relationships, developing an action plan for the future.
The intervention was developed in consultation with service users and members of a patient and public involvement (PPI) group.
Questionnaires measuring sexual risk behaviour, contraception use, STI knowledge, motivation to engage in safer sex, intensions regarding safer sex, stigma, quality of life, alcohol, smoking and substance use were completed by participants at baseline as well as three and six month follow up (post randomisation). All participants were offered condoms and lube at each session.
Twenty-two participants also took part in a qualitative study that aimed to understand the experience of taking part in the trial.
Results
The main outcome of the trial was to establish feasibility and acceptability for an intervention to promote sexual health. As such, no formal analysis was conducted, and all results presented as descriptive.
Recruitment was reported to be slower than anticipated. Overall, the study recruited and randomised 72 participants, meaning it fell a little short of the 100-participant target. 138 people were formally screened for eligibility, 117 met the criteria and 72 were randomised. Finally, 36 received treatment as usual and 27 received the sexual health promotion intervention. 22 of these 27 received the full three-hour intervention.
Retention was reported to be good. At three and six month follow up 81.9% and 76.3% of participants (split equally across the two arms) completed the questionnaires respectively.
Participants were asked about the number of unprotected sex acts they had participated in during the last three months. For those in the intervention group this figure had reduced from 97% of men and 73% of women at baseline to 50% of men and 53% of women at six month follow. In the TAU arm figures were 87% and 68% for men and women respectively at baseline and 79% and 97% at six month follow up. However, it is important to note that 50% of participants reported no sexual acts during the study period. It is not reported whether these participants are distributed across the intervention and TAU groups, however, the authors attribute this as the reason why no significant effects were found.
No adverse events were reported in the paper and results from the qualitative component indicated that those who received the intervention found it interesting and informative. Participants also expressed a preference for being able to have a conversation with someone, such as their care coordinator, about participating in the trial. Despite completion of surveys taking up to two hours and involving questions about sexual activity, participants reported they had been comfortable with data collection.

Recruitment was slower than expected but retention was good and participants gave positive feedback about being involved in the trial.
Conclusions
The main outcome of the trial was to establish the feasibility and any limitations to inform a larger-scale, future study. The authors concluded that the intervention was “feasible safe and acceptable to participants”. There were no significant effects found, however there was a trend whereby those who received the intervention reported reduced unprotected sex at six month follow up compared to those in the TAU group.

Sexual health research within mental health services can be feasible, safe and acceptable.
Strengths and limitations
There are lots of great things about this study. It contributes to a growing body of work that aims to acknowledge and address the sexual health needs of people who experience mental health difficulties. Whilst there have been initiatives to promote sexual health in inpatient settings and resources developed to encourage conversations and support in this area (Luby, 2020), this is the first RCT that I am aware of that has trialled a sexual health promotion programme in a community setting. The robust design, justification of sample size and involvement of people with lived experience are all to be credited. Additionally, given the notoriously tricky nature of behaviour change, it’s a real strength of this study that the design of the intervention followed existing guidance and was based in theory and problem-driven. The inclusion of exercises to increase self-efficacy, self-worth and assertiveness are likely to be particularly valuable, not only because people with mental health diagnoses can experience low self-esteem linked to internalised stigma (Livingston et al., 2010), but also because low self-esteem has been linked to intimate partner violence, unprotected sex (Taquette et al., 2019) and difficulty forming intimate relationships (de Jager et al., 2017).
The authors’ conclusion that sexual health interventions are feasible and acceptable is a novel and encouraging finding. For me, the fact that there were no adverse events reported is particularly important. My own qualitative research indicates that minimising risk is a key priority for mental health professionals (White et al., 2019). People who use mental health services are often seen as ‘vulnerable’ and relationships may be seen as inherently risky. Mental health professionals may worry that being exposed to rejection or exploitation within relationships may actually be detrimental to service users’ mental health. So, providing support in this area is seen as incongruous with the main aim of services (to reduce risk). The fact this study reported no adverse events challenges the view that discussing sex and relationships will ‘rock the boat’ in terms of service users’ mental health and these findings should be used to challenge this view when it is presented.
Regarding limitations, we need to be mindful that this is a topic many may regard as personal, private or indeed, prefer to discuss with someone outside of mental health services. We must consider why it is that almost half (45%) of participants were excluded before randomisation for reasons unknown and why 25% of those allocated to the intervention arm of this study did not receive the sessions. One possible explanation is that those who entered and remained in the study were more comfortable discussing sex within the context of mental health services. Therefore, we shouldn’t assume that this type of intervention is desirable to all. Some may prefer to receive support and information about sexual health from sources external to mental health services. As noted by the authors, more detailed information about the numbers of potential participants screened would give a clearer picture of how desirable the intervention was generally.
Finally, this study took a ‘one-size fits all’ approach to sexual health, with people of all sexualities and all diagnoses receiving the same intervention. Information about participants’ diagnoses are not provided and whilst some aspects may be relevant to all, experiences may differ between diagnostic groups. Similarly, adjustments could be made to make content more relevant to members of the LGBTQI+ community. For example, although lesbians may use condoms, is two sessions on condoms and contraception overkill? I mentioned in my previous blog that members of the LGBTQI+ community are likely to have different needs than those who identify as heterosexual due to intersectional discrimination – would some of the time be better spent addressing these experiences and issues? Obviously, this is still an emerging area of research and we can’t do everything at once! However, future work should be mindful to avoid being heteronormative, especially as research suggests sexual and gender minority people are at increased risk of mental distress, suicide and substance dependence due to hostility and prejudice experienced because of their identity (King et al., 2008; Valentine et al., 2018). The sessions described in this study could be tailored to individuals’ needs, especially as it seems the intervention was delivered 1:1, which affords flexibility, making this easier to do than in group interventions.

Key strengths of this novel RCT are the robust design and involvement of people with lived experience.
Implications for practice
The fact the authors reported better recruitment when they approached eligible potential participants directly as opposed to via mental health staff was attributed to demands of the job, leaving little time to discuss the study with potential participants. This is almost certainly a contributing factor. However, it is also worth considering that professionals may be sceptical (due to already large workloads) about any interventions that could be perceived as non-essential or may potentially increase risk. In a way, the intervention in this study is an ideal gateway to more holistic work around sex and romantic relationships with people who experience mental health difficulties as it aims to minimise risk, which as mentioned previously, is something services are extremely concerned with.
However, I can’t help feeling that the attitudes more generally need shifting – why is it that when a friend or colleague announces that they’re pregnant it’s ‘congratulations!’ and excitement, but if a service user might be pregnant there’s a distinct feeling of, in my experience: ‘SHIT!’. Yes, the experience of mental distress can make parenting more challenging (Strand et al., 2020) and the possible involvement of other services would bring complexity, but pervasive and damaging stigmatising views about people with mental health difficulties being bad parents are not helpful (Lacey et al., 2015). Let’s not forget that people with mental health diagnoses have the same aspirations as everyone else, and that can include relationships and everything that comes with them. I think it’s important that work is done with staff to address any paternalistic attitudes and to reframe and challenge concerns about risk to make any sexual health/relationship intervention a success in practice.
The RESPECT study begins this work by viewing “sexual health as broader than simply the prevention of infections” and giving “a clear message that sexual expression is an important part of being human and having a mental illness should not exclude people from what is actually a fundamental human right”. The fact no adverse events were recorded from this study will be encouraging and hopefully pave the way for more holistic consideration of sex and relationships within mental health services.

Mental health staff may be concerned that discussing sex and relationships could increase risk, but this study reported no adverse events.
Statement of interests
My PhD is about romantic relationships in the context of psychosis. I have previously had correspondence with the first author of the paper regarding the submission of abstracts for a conference symposium.
Links
Primary paper
Hughes E, Mitchell N, Gascoyne S, Moe-Byrne T, Edmondson A, Coleman E, Millett L, Ali S, Dare C, Hewitt C, Johnson S, Llewellyn C, Mercer C, Nolan F, Walker C, Watson J. Sexual health promotion in people with severe mental illness: the RESPECT feasibility RCT. Health Technol Assess. 2019 Dec;23(65):1-136. doi: 10.3310/hta23650. PMID: 31854292; PMCID: PMC6936169.
Hughes, E., Mitchell, N., Gascoyne, S. et al. (2020) The RESPECT study: a feasibility randomised controlled trial of a sexual health promotion intervention for people with serious mental illness in community mental health services in the UK. BMC Public Health 20, 1736 (2020). https://doi.org/10.1186/s12889-020-09661-x
Other references
de Jager, J., Cirakoglu, B., Nugter, A., & van Os, J. (2017). Intimacy and its barriers: A qualitative exploration of intimacy and related struggles among people diagnosed with psychosis. Psychosis-Psychological Social and Integrative Approaches, 9(4), 301-309.
Hughes E, Bassi S, Gilbody S, Bland M, Martin F (2016). Prevalence of HIV, hepatitis B, and hepatitis C in people with severe mental illness: a systematic review and meta-analysis. Lancet Psychiatry, 3(1):40-48
Livingston, J. D., & Boyd, J. E. (2010). Correlates and consequences of internalized stigma for people living with mental illness: A systematic review and meta-analysis. Social science & medicine, 71(12), 2150-2161.
Luby, R. (2020). Using the STARTER model to talk about sex in mental health nursing practice. Mental Health Practice, 23(3).
Strand, J., Boström, P., & Grip, K. (2020). Parents’ descriptions of how their psychosis affects parenting. Journal of Child and Family Studies, 29(3), 620-631.
Taquette, S. R., & Monteiro, D. L. M. (2019). Causes and consequences of adolescent dating violence: a systematic review. Journal of injury and violence research, 11(2), 137.
Trevillion, K., Oram, S., Feder, G., & Howard, L. M. (2012). Experiences of domestic violence and mental disorders: a systematic review and meta-analysis. PLoS One, 7(12), e51740.
Valentine, S. E., & Shipherd, J. C. (2018). A systematic review of social stress and mental health among transgender and gender non-conforming people in the United States. Clinical Psychology Review, 66, 24-38.
White, R., Haddock, G., & Varese, F. (2019). Supporting the intimate relationship needs of service users with psychosis: what are the barriers and facilitators?. Journal of Mental Health, 1-7.
White, R. (2020). Sex and schizophrenia: what determines sexual interest and confidence? The Mental Elf.
Photo credits
- Photo by Reproductive Health Supplies Coalition on Unsplash
- Photo by Jude Beck on Unsplash
- Photo by Dainis Graveris on Unsplash
- Photo by Brooke Cagle on Unsplash
- Photo by Artem Maltsev on Unsplash
