
A friend of the Elf has ankylosing spondylitis, a chronic inflammatory rheumatic disease that affects mainly the skeleton, causing inflammation of the spine, but can also affect the peripheral joints, eyes, bowel and skin. They have also been suffering with their mouth health.
The Elf’s friend wondered if there is any connection between the two. On looking at the evidence we found this recent review by a group in Aberdeen, their aim was to examine the link between ankylosing spondylitis and periodontitis.
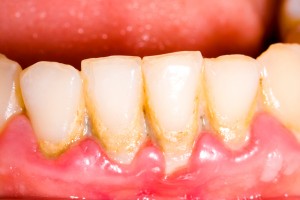
Periodontitis is a loss of the periodontal ligament which leads to loss of connective tissue and alveolar bone. Peridontitis can follow an immune response to the long term presence of plaque bacteria. Periodontitis may not have any symptoms but if left untreated it can lead to tooth loss.
Here’s what they did
The authors searched Medline, Embase, AMED, CINAHL, Web of Science and Google Scholar to March 2014 for reviews or reviews or observational studies of cross-sectional, case–control or cohort design. Randomized controlled trials, case reports and case series were excluded. There were no restrictions on publication date or publication status. Randomized controlled trials, case reports and case series were excluded. There were no restrictions on publication date or publication status. Two authors independently reviewed each study.
Participants of the studies had to be diagnosed with AS based either on recognized international criteria or on clinical diagnosis by a rheumatologist.
Prevalence of periodontal disease had to be reported in AS patients and also available for a non-AS population.
Here’s what they found
- Six case–control studies were included in the review.
- Study size ranged from 90 to 40 926 participants.
- The prevalence of periodontitis ranged from 38% to 88% in AS patients and from 26% to 71% in controls.
- As there was low-level heterogeneity (I2 = 13%), using fixed effects analysis the overall pooled estimate of the odds ratios for periodontitis was 1.85 (95% CI 1.72, 1.98).
- The only significant difference was found for Bleeding On Probing [using a random effects model, the combined mean difference between cases and controls was 14.05 (95% CI 4.16, 23.94), P = 0.005].
- There was no evidence of publication bias.
There is an important (almost double) and statistically significant risk of AS associated with periodontitis.
The author’s conclusions
Meta-analysis showed an important (almost double) and statistically significant risk of AS associated with periodontitis.
The authors also comment that it appears that DMARDs used for the treatment of chronic inflammatory rheumatic diseases may affect the risk of periodontitis.
The Musculoskeletal Elf’s view
The authors of this review suggest that the small number of studies with important methodological weaknesses. They recommend that there is a need for a study with sufficient statistical power to detect the desired effect size, taking into account potential confounding factors and using validated measures of AS and periodontitis.
So what is statistical power? It is ability of a study to demonstrate an association or causal relationship between two variables. By convention, 80% is an acceptable level of power. This means that there is 80% chance of ending up with a p value of less than 5% in a statistical test (i.e. a statistically significant treatment effect). If the statistical power of a study IS low, the study results will be questionable (the study might have been too small to detect any differences).
What is effect size? The effect size can be just the difference between the mean values of the two groups but there are other ways of calculating this. In general terms the larger the effect size, the greater is the impact of an intervention.
What do you think?
- Do you consider any association between ankylosing spondylytis and mouth health?
- Were you aware of periodontitis?
Send us your views on this blog and become part of the ever expanding Musculoskeletal Elf community. Post your comment below, or get in touch via social media (Facebook, Twitter, LinkedIn, Google+).
Links
- A possible link between ankylosing spondylitis and periodontitis: a systematic review and meta-analysis. Ratz T et al. Rheumatology (Oxford). 2015 Mar;54(3):500-10. doi: 10.1093/rheumatology/keu356. Epub 2014 Sep 10.
- Statistical power. Bandolier.
- Effect size. Bandolier


Is there a link between ankylosing spondylitis and periodontitis? http://t.co/mSLfwttxJm
#Glasgow #ChitChat | http://t.co/Hhk9FsqfUl | Is there a link between ankylosing spondylitis and periodontitis?
Q. Have #AnkylosingSpondylitis have gum probelms read our blog http://t.co/eJSuiJ7Ky7 @NASSdirector @arthritis_care
Q. Have #AnkylosingSpondylitis aware of #peridontitis read our blog http://t.co/5Y2pCK3EoM @NASSexercise @thecsp @TheDentalElf
Have #AnkylosingSpondylitis beware gum probelms read our blog http://t.co/5Y2pCKlfgk @Spinehealth @TheDentalElf @NASSchiefexec
Periodontitis &AnkylosingSpondylitis read @MSK_Elf blog http://t.co/pfDRl72p6J
Q. Is there a link #peridontitis & #AnkylosingSpondylitis new blog http://t.co/eJSuiJ7Ky7 @TheDentalElf @RheumJC @WeAHPs
Don’t miss the @MSK_Elf blog on Periodontitis and Ankylosing Spondylitis http://t.co/pfDRl72p6J
RT @MSK_Elf: Have #AnkylosingSpondylitis beware gum probelms read our blog http://t.co/eJSuiJ7Ky7 @Spinehealth @TheDentalElf @NASSchiefex…
Q. #AnkylosingSpondylitis and gum problems new blog http://t.co/5Y2pCK3EoM @TheDentalElf @spondylitis
Blog-post from @MSK_Elf discussing our meta-analysis of link between ankylosing #spondylitis and #periodontitis http://t.co/mJSv3fgXTx
Hi Tracey – I have read loads about RA and often research the links between AS and RA. I had been aware of the link between gingivitus bacteria (expressing an enzyme called PAD1) and citrullination of proteins. I also read a paper the other day about detection of citrullinated proteins in AS.
I successfully control my AS with diet changes (23 years now) – but I am aware there are other factors – and believe that gut bacterial balance is key also.
Then I also read a paper last week where researchers had run a comparison with amino acids in bacterial and dietary proteins – to look for homology to self proteins – they discovered that there were “countless candidates” for citrullination.
I’m not a scientist (I am in IT so a bit of a geek) – but it looks to me that 4 things cause autoimmune disease –
– Protein modification (either by citrullination / deamination / failed clearance apoptosis)
– Gut barrier (I had stopped taking all NSAIDs) – and we know from Fasano that zonulin causes gut permeability in all people irrespective of celiac
– Commensul bacteria that prime the immune response
– Genetic susceptibility
Hi Tracey – also wanted to add that I am in contact with many on forums that have successfully treated their RA (there are a few with AS too) with Minocyline / Minocin.
What I find interesting is that this antibiotic does not tend to impact Proteus Mirabilis or Klebsiella – but would be normally be effective against gingivitis – therefore may be impacting the post translational modification.
Dear Sean thanks for these comments I’m going to ask the Dental Elf for his opinion on this.
Sean,
I’m curious to know what helped people suffering from AS that includes oral degradation.I’ve had ulcerative colitis for over 15 years & developed AS the past 5. Any advice would be greatly appreciated.
I have A.S and dental loss I know many people also with A.S who have dental loss so I feel your study is correct there’s a connection
Is there a link between ankylosing spondylitis (AS) and tooth external resorption?
My dentist said today that a broken molar of mine has external resorption. As I was diagnosed with AS about 40 years ago and am now much better though retain a few mild symptoms, I wondered if the ankylosis in the system might provide some sprt of strange link. I’d be interested in your thoughts. Many thanks
External root resorption (ERR) is thought to occur following damage to the root surface and is see in patients who have had orthodontic treatment or previous trauma the teeth. while a number of studies have suggested that there may be a link between AS and periodontal disease I am not aware of any research linking AS and ERR.
I have had AS for many years but diagnosed 7 years ago. I have recently suffered from severe tooth problems and abscesses. Had operation to remove wisdom tooth three weeks ago and the abscess went all the way up to the eye socket and ear canal.
@MSK_Elf @NASSchiefexec @SpineHealth @TheDentalElf also check out oral health section @NRAS_UK