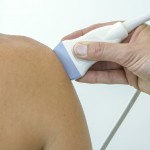
Calcium deposits within tendons (calcific tendonitis) of the shoulder’s rotator cuff muscles is a common cause of shoulder pain in middle age, and is more common in women. Normally, this is a self-limiting condition that resolves without the need for any intervention, but patients with prolonged symptoms may be offered barbotage.
Barbotage comes from the French word meaning ‘to bubble or splash’, and in some contexts can be used to describe champagne cocktails. Unfortunately, for these elves with shoulder pain, barbotage describes a technique of ultrasound guided needle dissection of the calcium deposits under local anaesthetic, normally undertaken in a clinic room, allowing the deposits to be removed straight away.
But does it work? This study published last year from a group in Blackpool, UK examines the available evidence behind the practice
Here’s what they did
They searched online medical journal databases (MEDLINE, EMBASE, Cochrane library) for all research into the use of ultrasound guided barbotage in the shoulder for calcific tendonitis until June 2013. They included studies in all languages, and all studies that included more than one patient. They focussed their analysis upon the results following barbotage, in addition to which patient groups were included and the investigations the patients had undergone before the treatment. They also investigated the technical details of how the procedure was undertaken and any complications seen.
Here’s what they found
- 13 relevant studies were found by the search that included a total of 908 patients.
- 9 prospective trials, but no randomised control trials were found. The difference in trial types found prevented meta-analysis from being undertaken.
- Average age of patients included was between 40.3-63 years; all had shoulder pain and calcific tendonitis identified on imaging.
- 6 studies commented on management occurring before barbotage, all patients in these studies only having undergone conservative measures (pain relief, physiotherapy).
- Follow up range was 1 month- 10 years (most studies follow up between 1- 2 years)
- Technical details: 12 studies saw radiologists undertaking barbotage, 1 study was lead by an orthopaedic surgeon. 8 studies used a ‘double needle technique’.
Outcomes
- A combined result of 92% (198/214 patients) of patients had good or excellent outcomes post barbotage (5 studies).
- Constant score: mean improvement of 40.9 (3 studies)
- Shoulder pain and disability index score (SPADI) mean improvement of 23 (2 studies)
- Numeric rating scale (NRS) mean improvement of 8.1 (2 studies).
- Complications: A combined 7% complication rate (5 studies that quoted complications (67/908); all were considered minor. A combined 13% retreatment rate (114/908) with a 2nd treatment given for persistent pain was seen in 4 studies.
The authors concluded
There are small studies that show good or excellent results with the use of barbotage for calcific tendonitis, with minimal rates of minor complications quoted in evidence.
Small studies show good or excellent results with the use of barbotage for calcific tendonitis with minimal rates of minor complications.
The authors also appreciated the shortcomings of the studies, and suggested the need for more work in comparing barbotage to other available therapies.
The Musculoskeletal Elf’s view

A mixed bunch of studies to attempt to interpret! The group looked into study design and appreciated the shortcomings of the trials, and attempted to combine evidence from the trials to give us meaningful headline results. On the other hand, only 5 of 13 trials discussed complications, and only half discussed how long patients included had symptoms or what their previous management had been. These small studies show the likely benefits of barbotage, and with approximately 90% of people not needing a second treatment and having a good or excellent result you can understand the positive approach to the treatment. But what this systematic review really shows me is the need to wait for the results of upcoming randomised control trials to truly answer the question!!
What do you think?
- Have you undergone barbotage?
- Do you offer barbotage or other treatments in your centre?
- Do you find it effective in your patients?
Send us your views on this blog and become part of the ever expanding Musculoskeletal Elf community. Post your comment below, or get in touch via social media (Facebook, Twitter, LinkedIn, Google+).
Links
- Gatt DL, Charalambous CP. Ultrasound-guided barbotage for calcific tendonitis of the shoulder: a systematic review including 908 patients. Arthroscopy. 2014 Sep;30(9):1166-72 PMID 24813322 [abstract]
- NHS inform supraspinatus tendonitis
- PRISMA statement
- EQUATOR Network

Ultrasound guided barbotage for calcific tendonitis in the shoulder – does it work? http://t.co/tb3cqulmcj
#Ultrasound guided barbotage for calcific tendonitis #shoulder- does it work? http://t.co/IsXt5PqR7j @EFORTnet @IDEALCollab
calcific tendonitis #shoulder #Ultrasound guided barbotage – does it work? http://t.co/IsXt5PqR7j @BoneJointportal
today’s blog #Ultrasound guided barbotage for calcific tendonitis #shoulder- does it work? http://t.co/iFkiIZFS88
#Ultrasound guided barbotage for calcific tendonitis #shoulder- does it work? http://t.co/iFkiIZFS88 @ndorms @BritOrthopaedic
calcific tendonitis #shoulder #Ultrasound guided barbotage – does it work? http://t.co/iFkiIZFS88 @KirOxford
calcific tendonitis #shoulder #Ultrasound guided barbotage – does it work? http://t.co/iFkiIZFS88 @BoneJointDecade @bonejoint360
calcific tendonitis #shoulder #Ultrasound guided barbotage – does it work? http://t.co/iFkiIZFS88 @ndorms @OrthoEvidence
#Ultrasound guided barbotage for calcific tendonitis #shoulder- does it work? http://t.co/IsXt5PqR7j @AAOS1 @ortho_facts
I have had barbotage on the rotator cuff left shoulder and it relieved the pain for about 2-3 months then pain reoccurred and am still in pain. ant suggestions please ?
I had barbotage for calcific tendonitis of the right supraspinatus tendon over 30 months ago with Summit Medical Group in New Jersey. The radiologist was not able to aspirate the deposit due to its consistency, but instead performed fenestration. Rehab was uneventful and progressed over a period of about 5 weeks. The procedure was a complete success and I have no pain and now enjoy complete functionality of that shoulder. Now I need to do the left shoulder! It wasn’t as bad as the right side, but is now getting annoying.
Would have liked to have known the time to experience symptom relief.
@MSK_Elf @AAOS1 @ortho_facts