
Do you remember 2007? That’s the year Northern Rock collapsed triggering the banking crisis, Amy Winehouse went global with Back to Black, and the final book in the Harry Potter series hit the shelves.
It was also the last time the National Institute for Health and Clinical Excellence (NICE, 2007) published guidance on psychosocial interventions for substance misuse.
A recent review by the NICE project team concluded that:
After considering all the new evidence and views of topic experts, we decided that no update is necessary for the guideline.
– NICE, 2016
So is guidance published a decade ago fit for purpose in 2016? First it’s important to consider what’s happened with drug use and which drugs people have developed problems with. Back in 2007, opiates such as heroin accounted for the majority of new treatment presentations, but since then cannabis has become the main drug that people present with, as shown in the graph below.
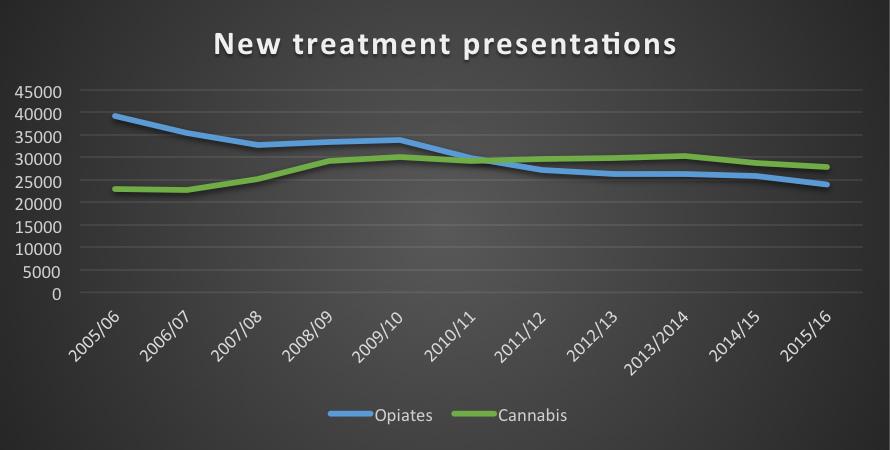
Cannabis has overtaken opiates as the main substance that users present with when starting drug treatment.
Opiate centric
Although the guidance has some generic information about assessment, self-help, brief interventions and involving families, it is telling that most of the examples given are in relation to injecting. This is important, but gives the impression that the guidance is aimed at ‘high risk’ injecting drug use. The majority of people who develop problems as a result of drug use in 2016 are not injecting their drugs. Cannabis remains the most widely used illicit drug and presentations to treatment services where cannabis is the primary problem have risen significantly in the last decade (Monaghan et al, 2016).
A recent Cochrane review for cannabis dependence found evidence to support a combination of motivational enhancement therapy (MET), cognitive behavioural therapy (CBT) and incentives (Gates et al 2016). But as fellow Elf Mark Monaghan pointed out in a recent blog, these reviews including the one by NICE limit their search to papers published in English (Monaghan, 2016). Given the range of treatment programmes across Europe, it is likely that we are missing valuable intelligence if evaluations of these treatments are published in a language other than English.
Most people who develop drug problems in 2016 are not injecting their drugs, which is the main focus of the NICE 2007 guidance.
Missing themes
Just like mass marketing, generic guidance misses some key groups and topics. Pregnant women who have drug problems are not catered for, but as two lives are involved deserve attention. Unfortunately all females have been ignored in research on substance use as acknowledged by a recent editorial in the Journal of Addiction (Del Boca, 2016).
Since 2007, legal highs or novel psychoactive substances (NPS) have emerged as a group of drugs that cause a range of problems, which workers in a range of settings will encounter. Project Neptune is one example of innovation in the field which offers evidence based guidance on NPS for drugs workers
Misuse of prescription drugs is not mentioned in the guidance, despite recent evidence that across Europe the United Kingdom has some of the highest levels of misuse of these drugs (Novak et al, 2016).
Although the last decade has seen a dramatic reduction in tobacco smoking in the general population this has not been mirrored for people who have problems with drugs, the majority of whom smoke. This is a complex issue for example many treatment staff who may not consider smoking a priority if you are injecting heroin. But research shows this group can be encouraged to quit (McClure et al, 2014).
There is scope for NICE to acknowledge these groups and substances in their updates, which might help draw attention to gaps in research and knowledge.

The decade old NICE guidance has a long list of gaps in the substances it covers.
Digital interventions
The last decade has seen significant innovations in technology. The Mental Elf being a good example of the way information about health and evidence is now communicated. In parallel, online or electronic methods of delivering health care have developed. Breaking Free Online is one example of a drug treatment innovation, which has accumulating evidence of reaching groups that don’t usually access traditional services (Elison et al, 2015).
Limitations
Alcohol is not included in the 2007 psychosocial interventions for substance misuse guidance, although NICE has issued a range of alcohol related guidance. Moreover, people don’t present with neat single drug use problems; they often use multiple substances including alcohol. It might be challenging in terms of drawing up guidance, but if guidance is to be meaningful and used in practice it needs to reflect the problems real people present with.
An additional factor is the relationship between mental health and substance use. Up to 70% of people in drug treatment settings have mental health problems (Turning Point, 2016). Although new guidance is due to be published by NICE imminently on dual diagnosis, topic or issue specific guidance risks looking artificial and distant from the reality of the complex problems that people present to services with. Depending on the individual presentation, a clinician could need to refer to three or more sets of NICE guidance, none of which take account of each other. There must be a better way to support workers and the people they meet.

Complex multimorbidities in patients pose complex challenges for health service staff (like this one pictured), which are rarely supported holistically by joined up guidance.
Summary
When reviewing their guidance, the teams at NICE invite individuals and organisations to submit comments and evidence. The consultation for this review attracted only two stakeholder contributions, but one notable stakeholder did disagree with the NICE decision not to update the guidance: Public Health England.
The overall lack of engagement with NICE on its consultation could be a reflection on the state of the treatment sector. Most drug treatment providers and the specialist staff working in them are subject to frequent retendering exercises. The sector has faced savage cuts in the last decade which have resulted in a rapid turnover of providers and staff. An environment that doesn’t lend itself to engaging with NICE on treatment guidance when survival is the priority.

In these hard times, guideline producers need to go that extra mile to engage with experts from the drug treatment sector.
Links
Primary paper
National Institute for Health and Clinical Excellence (2016) Surveillance report 2016 – Drug misuse: psychosocial interventions (2007) NICE guidelines CG51, 2016.
Other references
Del Boca, F.K., 2016. Addressing sex and gender inequities in scientific research and publishing (PDF). Addiction.
Elison, S., Davies, G. and Ward, J., 2015. Effectiveness of Computer-Assisted Therapy for Substance Dependence Using Breaking Free Online: Subgroup Analyses of a Heterogeneous Sample of Service Users. JMIR mental health, 2(2).
, , , , . Psychosocial interventions for cannabis use disorder. Cochrane Database of Systematic Reviews 2016, Issue 5. Art. No.: CD005336. DOI: 10.1002/14651858.CD005336.pub4.
McClure, E.A., Acquavita, S.P., Dunn, K.E., Stoller, K.B. and Stitzer, M.L., 2014. Characterizing smoking, cessation services, and quit interest across outpatient substance abuse treatment modalities. Journal of substance abuse treatment, 46(2), pp.194-201. [Abstract]
Monaghan,M. (2016) CBT and motivational interviewing: best bet for cannabis cessation. The Mental Elf, 7 Jun 2016.
Monaghan, M., Hamilton, I., Lloyd, C. and Paton, K., 2016. Cannabis matters? Treatment responses to increasing cannabis presentations in addiction services in England. Drugs: Education, Prevention and Policy, 23(1), pp.54-61. [Abstract]
National Institute for Health and Clinical Excellence (2007) Drug misuse in over 16s: psychosocial interventions. https://www.nice.org.uk/guidance/cg51
Novak, S.P., Håkansson, A., Martinez-Raga, J., Reimer, J., Krotki, K. and Varughese, S., (2016). Nonmedical use of prescription drugs in the European Union. BMC psychiatry, 16(1), p.274.
Turning Point (2016) Dual Dilemma (PDF).

NICE one? Is NHS guidance on substance misuse fit for purpose? https://t.co/aAkBZU1ZyJ
What was going on in 2007 ? should we still rely on @NICEcomms guidance for #addiction from 2007 ?… https://t.co/1JhXWegC1b
Today @ian_hamilton_ explains why NICE have missed a trick by not updating their 2007 substance misuse guidance https://t.co/5y7Mq8gbNy
@Mental_Elf An actual headclutcher – nice ;-)
@Mental_Elf @ian_hamilton_ Puzzled by use of “two lives” re pregnant women; a pregnancy isn’t a life. Don’t women deserve care qua women?
of course ! @Sectioned_ @Mental_Elf
@ian_hamilton_ @Mental_Elf And how does your article convey that?
difficult to do on guidance that has an impact on so many aspects of people’s lives but take your point @Sectioned_ @Mental_Elf
@ian_hamilton_ @Mental_Elf What point of mine is it you’re taking?
@Sectioned_ @Mental_Elf it could have been clearer and better
@ian_hamilton_ @Mental_Elf What’s the “it” in that sentence referring to?
@Sectioned_ @Mental_Elf my prose
@ian_hamilton_ @Mental_Elf Nope.
NICE one? Is NHS guidance on substance misuse fit for purpose? https://t.co/6HhU4fhF2y via @sharethis
UK drug use has changed quite significantly over the last decade, so why hasn’t @NICEcomms guidance changed too? https://t.co/5y7Mq8gbNy
@Mental_Elf @NICEcomms Because new evidence was consistent with existing guidance.
Has there really be no advance in knowledge on #addiction since 2007 ? @Mental_Elf https://t.co/EMdchozERA https://t.co/kTUrZRZP9r
@ian_hamilton_ @Mental_Elf re: opioids, just REGRESSION since Rolleston Report of 1926, accelerating rapidly in last 2 decades
NICE one? Is NHS guidance on substance misuse fit for purpose? via The Mental Elf -… https://t.co/R6Onv7wP0t
.@Breaking_Free_ your great work included in todays @Mental_Elf blog on @NICEcomms substance use guidance https://t.co/0rzxqz50tR
NICE one? Is NHS guidance on substance misuse fit for purpose? https://t.co/334fCL2WTs via @sharethis
would be interested in your thoughts @DrG_NHS is there too many guidelines ? should they be integrated ? https://t.co/ePLbA4HgCX
@NICEcomms one? Is NHS guidance on substance misuse fit for purpose? https://t.co/LDElQXiuq8 via @Mental_Elf
Is NHS guidance on #substance misuse fit for purpose? @ian_hamilton_ writes about this for @Mental_Elf see https://t.co/IdtEw3Btwt
Our guidance is being updated, it will come under the new guideline for drug misuse prevention. More details here:… https://t.co/HEGmz4oQV3
many thanks for this @NICEcomms @Mental_Elf & the link to the consultation, hoping as many people as possible will contribute this time
NICE one? Is NHS guidance on substance misuse fit for purpose? https://t.co/IGcEHvn75R via @sharethis
Great piece. Reflects sludgy NHS. NICE one? Is NHS guidance on substance misuse fit for purpose? https://t.co/TYyeTM0NSa via @Mental_Elf
@Mental_Elf Check out our resources for carers and friends of people with ARBD, and professionals working with them: https://t.co/yIGgEQDRFK
Back in 2007, NICE had nothing to say about women in its substance abuse guidance – & NICE has just decided it’s st… https://t.co/0kj646zcwe
these appear to be two different guidelines albeit both themed on substance use @Mental_Elf @NICEcomms but happy to be corrected
[…] Read the full blog post here […]
@Mental_Elf Hi, if you send this info through to nice@nice.org.uk we can check with the guideline developers.
@Mental_Elf @ian_hamilton_ sure, we’ll let the team know you’ll be sending.
Is #NHS guidance on #substancemisuse fit for purpose? https://t.co/6yYW4vMMXf Lack of #stakeholder contributions a problem finds @Mental_Elf
#LunchtimeRead
Another very accessible #SubstanceMisuse blog from @ian_hamilton_
Is NICE guidance fit for purpose?… https://t.co/D3hMTGb4Ho
@Mental_Elf @ian_hamilton_ Hi both, apologies we did flag the wrong update. Ian’s blog is correct. We’ll take down the correction tweet.
NICEly confused
Its great that the people at NICE have engaged with this blog as that’s the idea. There was a little confusion created by some of the tweets from NICE in response to the blog today, suggesting that the NICE guidelines the blog was based on would be updated next year. Unfortunately the people at NICE were mixing up guidelines as they were referring to guidance on substance misuse prevention and not the guidelines for substance misuse interventions, which the Mental Elf blog is about today. NICE have kindly acknowledged this mistake and have said they will remove their tweets that caused the confusion.
Perhaps this presents an opportunity to think about how guidance can be simplified or at least be made easier to access and understand, as it seems there is so much guidance at differing stages of development and review its confusing NICE.
p.s. would be interested in your thoughts on todays @Mental_Elf blog @TheNewImpostor on @NICEcomms & drugs – https://t.co/EMdchozERA
Darlin’ reach out!
Are @NICEcomms doing enough to consult with stakeholders on their drug misuse guidance?… https://t.co/RyAo9UuqOm
Perfect for my (very soon to be submitted) dissertation, cheers @mental_elf ? https://t.co/6GJwXvFeQG
NICE one? Is NHS guidance on substance misuse fit for purpose? https://t.co/Z135YDxqN5
NICE one? Is NHS guidance on substance misuse fit for purpose? https://t.co/LKFa5r76UF
Don’t miss:
NICE one?
Is NHS guidance on substance misuse fit for purpose?
https://t.co/5y7Mq8gbNy https://t.co/8yY0dztj8L
Are @NICEcomms guidelines focussed on #opiate at the expense of #cannabis ? @Mental_Elf https://t.co/EMdchozERA https://t.co/tIOGnVyepa
NICE one? Is NHS guidance on substance misuse fit for purpose? https://t.co/sREdfXTSn7 via @sharethis
RT @Mental_Elf: Most popular blog this week?
@ian_hamilton_ asks:
Is @NICEcomms guidance on #SubstanceMisuse fit for purpose?
https://t.co/…
NICE one? Is NHS guidance on substance misuse fit for purpose? https://t.co/QHZZBVokic via @sharethis
[…] Most drug treatment providers and the specialist staff working in them are subject to frequent retendering exercises. The sector has faced savage cuts in the last decade which have resulted in a rapid turnover of providers and staff. An environment that doesn’t lend itself to engaging with NICE on treatment guidance when survival is the priority. (The Mental Elf) […]