In my second blog for the Mental Elf I am reporting on a Cochrane review (Dougall et al, 2015) to address this question: Is transcranial magnetic stimulation (TMS) a safe and effective treatment for reducing the psychotic symptoms associated with schizophrenia?
Many patients with schizophrenia experience persistent positive and negative symptoms between acute episodes, in spite of apparently adequate drug treatment. Researchers and clinicians alike have thought that TMS could provide an alternative treatment for patients unsuited to standard medication.
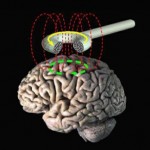
TMS involves the application of a strong magnetic field close to the surface of the scalp, it stimulates the brain, changing neuronal function (Chouinard P.A. et al, 2003), which is altered in patients with schizophrenia.
For example, activity in the Temporoparietal cortex (TPC) is increased in schizophrenia, which has been associated with auditory hallucinations (Shergill S.S. et al, 2000). Low frequency TMS (1Hz) is typically applied to the left TPC with the aim of reducing auditory hallucinations.
In contrast, activity is reduced in the dorsolateral prefrontal cortex (DLPFC), which has been linked to negative symptoms (Weinberger D.R. et al, 1996). High frequency TMS is applied to the left DLPFC to increase activity and reduce negative symptoms.
Both positive (Hoffman R.E. et al, 2005) and negative (McIntosh A.L. et al, 2004) controlled studies have been published using both treatment paradigms. This new Cochrane review aimed to evaluate the current evidence base of TMS treatments in schizophrenia.

This systematic review aimed to evaluate the evidence for the use of TMS in schizophrenia
Methods
Searches were done in the Cochrane Schizophrenia Group’s trial register. The authors also contacted the company who markets TMS machines in the UK for published and unpublished data. Studies were included that had been published up to April 2013.
All relevant RCTs with at least 5 participants were included. Participants were people with schizophrenia and related affective psychosis irrespective of age or gender.
Four types of intervention were included:
- The first, TMS at any stimulus voltage, frequency or charge, administered to the head at any location, this included theta burst stimulation (TBS TMS)
- Sham TMS
- Standard treatment (including antipsychotic medication)
- Other pharmacological or non-pharmacological treatments (such as electroconvulsive therapy or cognitive behavioural therapy)
Included papers assessed global, mental and cognitive state as well as adverse effects and quality of life.
Results
From 158 records identified through database searching, 41 studies were included in the meta-analysis. In total 1,473 participants were included in the review. The authors performed four main comparisons:
- Temporoparietal (TPC) TMS vs SHAM: There were some small improvements in the clinical global impression scale (CGI) and the Positive and Negative Syndrome Scale (PANSS). There was no evidence that cognitive state was affected.
- TPC TMS vs Standard care: There was no evidence that TPC TMS was superior to antipsychotic medication for improvements in global state.
- Prefrontal (PFC) TMS vs SHAM: No evidence of improvement in global, mental or cognitive state.
- PFC Theta-Burst Stimulation (TBS) TMS vs SHAM: Limited evidence for some improvements in mental state but not global or cognitive state.

Evidence was limited and did not show that any form of TMS produced clinically important improvements.
Conclusions
This Cochrane review has shown that although there is some evidence to support the benefit of TMS in schizophrenia, findings were inconsistent across measures and between studies.
The authors concluded that there was limited evidence for TPC TMS as superior to sham in improving auditory hallucinations and positive symptoms on the PANSS scale, supporting previously published meta-analyses (Freitas C. et al, 2009; Matheson S.L. et al, 2010).
While previous meta-analyses have reported that prefrontal TMS as superior to sham in improving negative symptoms (Freitas C. et al, 2009; Dlabac-de Lange J. et al 2010), the evidence for this was not replicated in this review.
Strengths and limitations
Overall the quality of evidence was poor. Although all studies were reported as randomised, there was unclear allocation concealment leading to a risk of selection bias. Most studies were reported to be double blind but only 7 used adequate blinding procedures, influencing both performance and attrition bias. Due to the high risk of bias and wide confidence intervals the quality of evidence was rated low to very low.
In addition to low quality data, the authors also highlighted a number of areas of weakness which I wanted to further comment on. Firstly there were substantial differences in the length of trials with a range of 4 days to 10 weeks. There was also a large variety in the stimulus voltage and frequency used. The lack of a standardized procedure for TMS makes comparison between studies very challenging and it is also difficult to know whether a potentially therapeutic dose was actually administered and thus assessment of efficacy difficult.
Another major issue is the variability in the control group used. In particular the use of Sham TMS is very variable. Some studies use the same stimulation but at a different angle to the scalp, while others use placebo stimulation which feels similar but produces no effects on the brain and others simply an identical sound. Ineffective sham methods bring into question if participants were adequately blinded and highlights how difficult it would be to conduct double-blind studies in this field.
In addition, the authors also highlighted how few studies compared TMS to active treatments, thus while the evidence is lacking for the therapeutic benefits of TMS, there is even less evidence that it is superior to current standard treatments.
In addition to the issues already discussed, there was also the issue of antipsychotic medication. In some studies both treatment groups were receiving first and second generation antipsychotic medication. Some studies excluded participants on clozapine, others did not, however some studies did not report whether antipsychotics were used at all or what type. It is difficult to know if any therapeutic effects of TMS are influenced by the concurrent use of antipsychotic medication, which again makes it difficult to assess its own clinical benefits.

Variety may be the spice of life, but in the case of treatment protocols it’s a big problem.
Summary
- Previous research has found that TMS can significantly reduce symptoms of schizophrenia. However this has not been replicated in all subsequent studies.
- This Cochrane review confirms this and has shown that although there is some evidence to support the benefit of TMS in schizophrenia, findings were inconsistent.
- At present, there is not enough evidence to support the use of TMS in any form to treat or manage symptoms of schizophrenia, either on its own or in conjunction with standard treatments.
- Further, high quality research is needed in this area. Future research must establish consistent therapeutic and sham protocols before larger scale trials can be performed.

Is TMS useful in the treatment of schizophrenia? At the moment no, but in the future definitely maybe…
Links
Primary paper
Dougall N, Maayan N, Soares-Weiser K, McDermott LM, McIntosh A. Transcranial magnetic stimulation (TMS) for schizophrenia. Cochrane Database of Systematic Reviews 2015, Issue 8. Art. No.: CD006081. DOI: 10.1002/14651858.CD006081.pub2.
Other references
Chouinard PA, Van der Werf YD, Leonard G, et al (2003) Modulating neural networks with transcranial magnetic stimulation applied over the dorsal premotor and primary motor cortices. J Neurophysiol 2003;90(2):1071–83.
Dlabac-de Lange J, Aleman A. (2009) Effect of high frequency rTMS on negative symptoms and cognitive functioning in schizophrenia. Netherlands Trial register.
Freitas C, Fregni F, Pascual-Leone A. Meta-analysis of the effects of repetitive transcranial magnetic stimulation (rTMS) on negative and positive symptoms in schizophrenia. Schizophr Res 2009;108(1-3):11–24.
Hoffman RE, Gueorguieva R, Hawkins KA, et al. (2005) Temporoparietal transcranial magnetic stimulation for auditory hallucinations: safety, efficacy and moderators in a fifty patient sample. Biol Psychiatry 2005;58(2):97–104. (PubMed Abstract)
Matheson SL, Green MJ, Loo C, et al (2010). Quality assessment and comparison of evidence for electroconvulsive therapy and repetitive transcranial magnetic stimulation for schizophrenia: a systematic meta-review. Schizophr Res 2010;118(1-3):201–10. (PubMed Abstract)
McIntosh AM, Semple D, Tasker K, et al (2004) Transcranial magnetic stimulation for auditory hallucinations in schizophrenia. Psychiatry Res 2004;127(1-2):9–17. (PubMed Abstract)
Saba G, Verdon CM, Kalalou K, et al (2006) Transcranial magnetic stimulation in the treatment of schizophrenic symptoms: A double blind sham controlled study. J Psychiatr Res 2006;40(2):147–52. (PubMed Abstract)
Shergill SS, Brammer MJ, Williams SC et al (2000) Mapping auditory hallucinations in schizophrenia using functional magnetic resonance imaging. Arch Gen Psychiatry 2000;57:1033–8.
Weinberger DR, Berman KF. (1996) Prefrontal function in schizophrenia: confounds and controversies (PDF). Philos Trans R Soc Lond B Biol Sci 1996; 351(1346):1495–503
Photo credits
- By Eric Wassermann, M.D. [Public domain], via Wikimedia Commons
- UK in Israel CC BY 2.0
- Sutha Kamal CC BY 2.0
- Kahlil CC BY 2.0
- Adrienne Bassett CC BY 2.0
- Kristian Bjornard CC BY 2.0


Transcranial magnetic stimulation for schizophrenia https://t.co/e0QWh4k8Pm #MentalHealth https://t.co/re7JhhS20E
Today @StarryJojo on recent @CochraneSzGroup SR of Transcranial Magnetic Stimulation for schizophrenia https://t.co/fqwc596OMt
Transcranial magnetic stimulation for schizophrenia https://t.co/fqwc59opE1 #TMS #schizophrenia #CochraneEvidence
Hi @nadinedougall @KarlaWeiser @mcintosh2001 We’ve blogged about your TMS for schizophrenia review https://t.co/fqwc596OMt Any thoughts?
Does TMS work in schizophrenia? Check out my latest blog @Mental_Elf https://t.co/Q3izkvxi6B
Transcranial magnetic stimulation for #schizophrenia https://t.co/8PgcOhwmgR @Mental_Elf finds some #evidence in use of #TMS in #psychosis
Is transcranial magnetic stimulation safe & effective for reducing psychotic symptoms assoc w schizophrenia? https://t.co/fqwc596OMt
Catch @StarryJojo’s blog for @Mental_Elf about @nadinedougall’s TMS for schizophrenia Cochrane Review https://t.co/gDFebmdOtR #MentalHealth
Recent SR finds Transcranial Magnetic Stimulation for schizophrenia produced no clinically important improvements https://t.co/fqwc596OMt
Don’t miss: Transcranial magnetic stimulation for schizophrenia https://t.co/fqwc596OMt #EBP #InTheMind