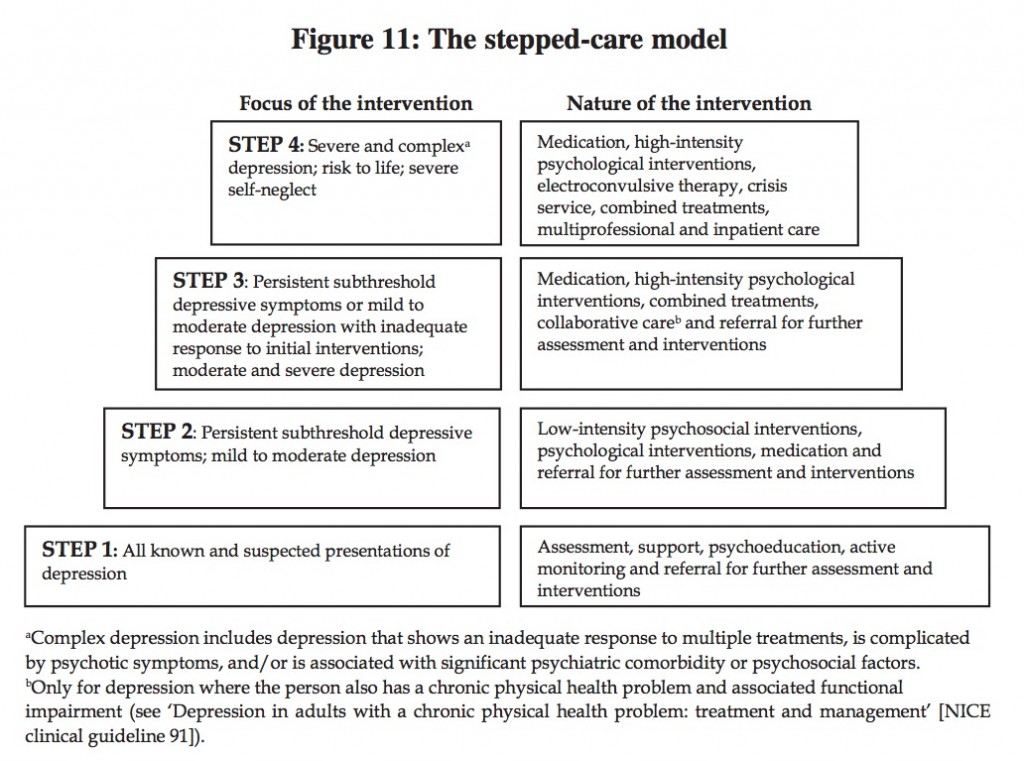
The NICE depression guidance recommends a stepped-care model for treating mild to moderate depression (see figure 11 below).
A considerable amount of funding has gone towards the Improving Access to Psychological Therapies initiative in England, but despite this the availability of individual therapy remains limited and relatively few people with depression receive the kind of individual cognitive behavioural therapy that is recommended by NICE.
The stepped-care model includes a number of possible interventions:
- individual cognitive behavioural therapy (CBT)
- computerised cognitive behavioural therapy (CCBT)
- group cognitive behavioural therapy (CBT)
- structured group physical activity programmes
- guided self-help programmes
- antidepressant drugs
However, the research evidence for these different therapies is of variable quality. For example, there is strong evidence for the effectiveness of antidepressants and individual psychotherapies, but the evidence for group-based talking treatments is less clear.
This new systematic review published in the British Journal of Psychiatry assesses the efficacy of group-based psychological therapies for depression in primary care and the community.
The research team from the University of Bristol conducted a comprehensive search and found 23 studies to include in their meta-analysis. They stated that the quality of studies was poor.
Here’s what they found:
- Group CBT performed better than usual care immediately post-treatment (standardised mean difference (SMD) -0.55 (95% CI -0.78 to -0.32))
- Group CBT performed better than usual care in the short-term (SMD = -0.47 (95% CI -1.06 to 0.12))
- Group CBT performed better than usual care in the medium- to long-term follow-up (SMD = -0.47 (95% CI – 0.87 to -0.08))
- Individual CBT performed better than group CBT immediately post-treatment (SMD = 0.38 (95% CI 0.09-0.66))
- They found no difference between individual CBT and group CBT at short- or medium- to long-term follow-up
The researchers concluded:
Group CBT confers benefit for individuals who are clinically depressed over that of usual care alone. Individually delivered CBT is more effective than group CBT immediately following treatment but after 3 months there is no evidence of difference. The quality of evidence is poor. Evidence about group psychological therapies not based on CBT is particularly limited.
Huntley AL, Araya R, Salisbury C. Group psychological therapies for depression in the community: systematic review and meta-analysis. Br J Psychiatry. 2012 Mar;200:184-90. [PubMed abstract].