
The diagnosis and treatment of depression in later life can be complex, and while treatments are available, these are effective less than half the time (Avari J. et al, 2014). Treatment-resistant late life depression occurs in 50-60% of patients (O’Brien J, 2015). Between 20-30% of older adults with treatment resistant depression do not achieve recovery. This can lead to increased risk of mortality, disability and reduction in quality of life (Dew M. et al, 2007).
Previous trials have shown that in patients that do not improve, adjunctive treatment with aripiprazole (an atypical antipsychotic) is more effective than stand-alone treatment with antidepressants (Steffens D, 2011). There is a gap in the information available regarding augmentation in late life depression in older adults (Dew M. et al, 2007).
Owing to this lack of evidence for clinicians, Lenze and colleagues (2015) developed a randomised, double blind, placebo-controlled trial (the first of its kind) that proposed the addition of aripiprazole would:
- Be associated with higher remission probability rate than placebo
- Greater improvement of depressive symptoms
- Resolution of suicidal ideation
- Better stability than placebo
- But may lead to increased risk of akathisia
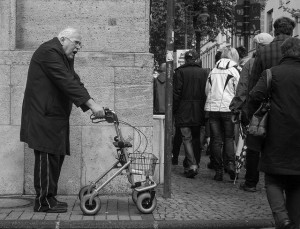
20-30% of older adults with treatment resistant depression do not achieve recovery
Methods
From July 2009 through to December 2013 participants over the age of 60 with major depressive disorder were recruited across three academic centres.
The study consisted of three phases:
- Open label treatment
- Randomization
- Follow up/ continuation
During the open label treatment, participants started on venlafaxine over 12 weeks with at least 4 weeks on the highest tolerated dose (up to 300mg/day). In some cases participants were treated up to 24 weeks to better establish treatment resistance. However, in most cases the treatment period was 12-14 weeks.
Once treatment resistance was established, participants entered the 12 week randomised phase. They were randomly assigned (1:1) to either the addition of aripiprazole or matched placebo starting at 2mg/ day and titrated as tolerated to a target dose of 10mg with the potential to increase to 15mg/day if required. The final dose of venlafaxine achieved in the initial open label treatment was maintained throughout the randomisation and follow-up phases.
Those who remitted in the randomisation phase entered a 12 week follow-up phase to assess the stability of remittance. The study drug was continued throughout this follow-up phase and double blind maintained.
The primary efficacy outcome was remission, with a MADRS score of 10 or less and at least a 2 point drop since baseline. The MADRS was carried out by independent raters.
Depressive symptoms, suicidal ideation and self-reported somatic symptoms were measured using the Hamilton Depression Rating Scale 17-item (Ham-D), Scale of Suicidal Ideation and the UKU scale. Cardiometabolic outcomes, weight, tardive dyskinesia, blood panel, and QT interval were also assessed at differing time points.
Results
Initially 1,098 people were screened with 486 entering open label treatment. From this 181 (39%) did not remit, of which 91 were randomized to aripiprazole and 90 to placebo.
Side-effect outcomes were as follows:
- Akathisia was common for those on aripiprazole; reported 26% of 91 vs 1% of 90 on placebo. In most cases this was mild and did not always persist into the follow-up phase
- Increased Parkinsonism; 17% of 86 on aripiprazole vs 2% of 81 on placebo
- Those on aripiprazole were more likely to experience increased dream activity, weight gain and tremor
- 5% of the aripiprazole group reported serious adverse events vs 2% on placebo
- 30 (33%) of the 91 participants on aripiprazole and 28% of 90 assigned to placebo presented with suicidal ideation at baseline. From this:
- Suicidal ideation resolved in 73% of 30 participants on aripiprazole vs 44% of 25 on placebo
- There was no associated increase in treatment emergent suicidal ideation
Positive outcomes included:
- Higher chance of remittance on aripiprazole vs placebo 44% vs 29%; odds ratio 2.0 (95% CI 1.1 to 3.7), p=0.03
- Enhanced improvement of (MOS) mental component score
- Did not detect QTc prolongation
- No differences noted for changes to percentage of body fat, total cholesterol, HDL, LDL, triglycerides, glucose, and insulin concentrations
- Greater decrease in their MADRS scores

Suicidal ideation resolved in 73% of 30 participants on aripiprazole versus 44% of 25 on placebo.
Conclusions
Over a 6 month period it was found that the addition of aripiprazole induced remission and was maintained during the follow-up phase.
Aripiprazole was associated with some akathisia and treatment emergent parkinsonism. There was no association between aripiprazole and an increase in cardiometabolic risk.
These findings help to inform on the risks and benefits of aripiprazole augmentation for treatment-resistant depression in older adults. The NNT (number needed to treat) for aripiprazole is 6.6, but this has a wide confidence interval around it (95% CI 3.5 to 81.8).
Clinicians need to be aware of the adverse effects of aripiprazole and adjust dose accordingly or potentially switch treatment.
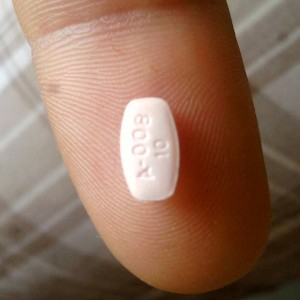
The addition of aripiprazole was found to be moderately effective in older adults with treatment resistant depression.
Strengths and limitations
The authors suggest several limitations to their study:
- Small sample size
- The short duration of the study
- Under representation of participants aged over 75
- Exclusion of those with cognitive impairment and dementia
Due to these limitations the study has been unable to fully address safety and tolerability of aripiprazole for older adults.
This was a well thought-out trial that had clear aims which were addressed and shortfalls highlighted. Placing an emphasis for clinician awareness on the risks of akathisia and parkinsonism and the need for further trials to better address tolerability and different combinations of treatments.

This RCT does not fully address the safety and tolerability of aripiprazole for older adults.
Summary
This and similar trials consistently highlight the need for more studies on treatment options available to older adults with treatment resistant depression. The trial is suggestive that aripiprazole is an affective adjunctive treatment and the authors have gone some way to addressing the concerns commonly raised around safety and tolerability.
Key points to take away from this trial are the reduction in suicidal ideation and depressive symptoms. It provides an important step towards better understanding of pharmacological treatments for treatment resistant depression in older adults and a way forward for future research.

Patients and their caregivers must ask themselves: do the benefits outweigh the risks?
Links
Primary paper
Lenze E, Mulsant B, Blumberger D. et al (2015) Efficacy, safety, and tolerability of augmentation pharmacotherapy with aripiprazole for treatment-resistant depression in late life: a randomized, double-blind, placebo-controlled trial. The Lancet, 386: 2404-2412. (PubMed abstract)
Other references
Avari J, Yuen G, AbdelMalak B. et al (2014) Assessment and Management of Late-Life Depression. Psychiatric annals 44:3.
Cooper C, Katona C, Lyketsos K. et al (2011) A systematic review of treatments for refractory depression in older people. Am J Psych 2011: 168:161-88. (PubMed abstract)
Dew M, Whyte E, Lenze E. et al (2007) Recovery From Major Depression in Older Adults Receiving Augmentation of Antidepressant Pharmacotherapy. Am J Psychiatry 164:6.
Karp J, Reynolds C. (2004) Pharmacotherapy of Depression in the Elderly: Achieving and Maintaining Optimal Outcomes. Primary Psychiatry. 2004;11(5):34-46.
O’Brien J. (2015) Management of late-life depression: a major leap forward (Editorial). Lancet, 386: 2374-2375.
Steffens D, Nelson C, Eudicone J. et al (2011) Efficacy and safety of adjunctive aripiprazole in major depressive disorder in older patients: a pooled subpopulation analysis. International journal of geriatric psychiatry, 26(6) 564-572.
Photo credits
- Jake Stimpson CC BY 2.0
- Georgie Pauwels CC BY 2.0
- Ant Jackson CC BY 2.0
- Daniel Oines CC BY 2.0
- Jake Stimpson CC BY 2.0
- By Boboque (Own work) [Public domain], via Wikimedia Commons

@Mental_Elf great blog,shame the authors excluded those using alcohol & other substances given the high prevalence for this group,pragmatic?
Aripiprazole for treatment-resistant depression in later life: do the benefits outweigh the risks? https://t.co/JxpO5Sd9JW
@Mental_Elf be interesting to know if talking therapy tried before labelled “treatment resistant”
20-30% of older adults with treatment-resistant depression do not recover https://t.co/JxpO5Sd9JW
Aripiprazole for treatment-resistant depression in older adults @Mental_Elf looks at the evidence https://t.co/by8FpiffOD
RCT @TheLancet finds aripiprazole to be moderately effective in older ppl w treatment-resistant depression https://t.co/JxpO5Sd9JW
New RCT from @CFReynolds3MD et al does not fully address safety & tolerability of #aripiprazole for older adults https://t.co/JxpO5Sd9JW
Don’t miss: Aripiprazole for treatment-resistant depression in older adults https://t.co/JxpO5Sd9JW
@Mental_Elf “Older adults” but not over 75? Risk of Akathisia increases with vascular damage as people age. Akathisa can be very distressing
Khalid Azmi
[…] 1Aripiprazole for treatment-resistant depression in later life- Mental Elf Blog post. […]