
Complementary and alternative medicine (CAM) therapies are often perceived to be as effective as conventional treatments, more “natural”, less expensive, have fewer side-effects and are easily available without a prescription. But do these perceptions match up with the reality? Can CAM therapies be helpful additions to conventional treatments?
This alludes to an interesting sociological question – why do we use CAM therapies? Sometimes even with the knowledge that there is a poor evidence base? Qualitative research has found that CAM-users tend not to be dissatisfied with conventional medicine; rather they believe CAM therapies expand their health care options (Bishop et al, 2010). Furthermore, information from the US National Center for Complementary and Alternative Medicines notes that CAM-users tend to be female, have above average levels of income and education. The Health Survey for England suggests use of CAM therapies remains substantial, even amongst those taking prescription drugs (Hunt et al, 2010). This suggests that people with more disposable income and education are more likely to be attracted to use CAM as a way to enhance their health… but is it worth the money? Does it actually work?

Globally, the CAM industry is estimated to be worth some $60 billion a year (Source: The Economist, 2011)
This is an important research area; as long as CAM therapies are available – it is important to understand the benefits and harms of using such therapies, so that patients can make informed decisions about their treatment.
1 in 4 people will experience some sort of mental health problem over the course of a year, and in Britain anxiety and depression are the most common mental health illnesses diagnosed and treated. A range of treatment options are typically offered to patients with diagnosed depression and/or anxiety, and these can include pharmacotherapy (e.g. antidepressants) and talking therapies (e.g. CBT or counselling). However, sometimes people opt for CAM therapies (e.g. physical therapies, herbal remedies, dietary supplements etc) to support their recovery.
Ravindran and Da Silva recently published a systematic review which sought to find evidence for the efficacy and safety of CAM therapies as an adjunct to pharmacotherapy (using CAM alongside drugs) in the treatment of depression and/or anxiety.
Methods
The authors limited their review to CAM therapies with a “reasonable body of published research” (no further details regarding what was considered ‘reasonable’ were provided in the paper).
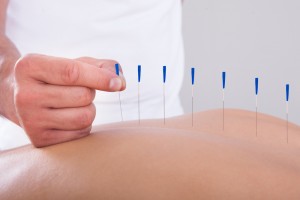
There are numerous systematic reviews about acupuncture for mental health issues, but they simply highlight the lack of good quality randomised trials in this field
Included CAM therapies were physical therapies (specifically exercise, yoga, acupuncture, sleep deprivation and light therapy), herbal remedies (specifically free and easy wandered plus (FEWP)), and dietary supplements (specifically omerga-3 fatty acids, S-adenosylmethionine, dehydroepiandrosterone, tryptophan, folate, inositol and N-actetylcysteine).
Results
The authors reported that there have been many more published studies looking at CAM therapies for depressive conditions, and far fewer studies for anxiety conditions. Most identified papers studied the impact of therapies in the short-term, so we do not know how long any reported benefits would last.
Evidence identified by this review (which included a comparison group) suggested:
- Some benefit for depression in using sleep deprivation therapy or FETW (at least one double-blind RCT).
- Some benefit for bipolar disorder in using omega-3 fatty acid supplements (meta-analyses), and sleep deprivation therapy (at least one double-blind RCT).
Overall, the evidence identified was “insufficient to inform recommendations for clinical practice” due to sparse data and methodological weaknesses of the research.
Conclusion
The authors suggested there was some evidence of benefit for people with depressive disorders who use CAM, but very little evidence of benefit for anxiety disorders. The authors stressed caution in clinical use due to the lack of adequate safety and tolerability data, and they make it very clear that CAM therapies should not be considered replacements for first-line evidence based treatments for depression or anxiety.
Overall, this paper is methodologically weak and therefore it is difficult to draw any firm conclusions from the reported findings.
Discussion
Personally, I do not think pooling “Complementary and Alternative Medicine” therapies under the same umbrella is helpful, as CAM therapies are so vastly different. I feel as if the authors have tried to cram too much into this paper, and have therefore neglected to report important details. I would recommend that future researchers limit their review to a single intervention or treatment group, in order to reduce heterogeneity and produce findings which can be described, interpreted and appraised in a meaningful way.
It is always important to remember that lack of evidence does not mean the treatment doesn’t work. It may be that CAM therapies are useful and can aid people with mental health issues, however the current evidence-base is weak and does not support this. This Elf is frustrated by the poor quality of CAM research to-date, and hopes the quality of future studies of CAM for mental health improves!
Top 5 tips for improving the quality of CAM research:
- Ask a focused question targeting a single intervention or treatment group
- Ensure a representative sample size
- Report treatment effects compared to either placebo or current treatments
- Design the research so it accounts for chance bias and confounders
- Provide information about both benefits and harms over time
Only then can we judge whether CAM therapies will remain ‘complementary’ or ‘alternative’, or whether some therapies ought to be reconsidered as ‘conventional’ treatments.
In the meantime, if you are interested in trying a CAM therapy – please do so with caution. It is always a good idea to discuss your plans with a health professional before starting.
Links
Ravindran AV and da Silva TL (2013) Complementary and alternative therapies as add-on to pharmacotherapy for mood and anxiety disorders: A systematic review. Journal of Affective Disorders, Sep 25;150(3):707-19. [PubMed abstract]
Bishod, FL, Yardley L, Lewith GT (2010) Why consumers maintain complementary and alternative medicine use: a qualitative study. J Altern Complement Med. 2010 Feb;16(2):175-82. [PubMed abstract]
The Use of Complementary and Alternative Medicine in the United States. National Center for Complementary and Alternative Medicine, 2008.
Hunt KJ et al (2010) Complementary and alternative medicine use in England: results from a national survey. Int J Clin Pract. 2010 Oct;64(11):1496-502. [PubMed abstract]
Medicine: There is no alternative. The Economist, 19 May 2011.
Dr Edzard Ernst frequently blogs about alternative medicine – if you are interested in this topic, I would recommend having a look at the Alternative Medicine section of his website.




CAM: Many of us are using it, despite poor evidence. Whats going on?: Complementary and alternative medicine (… http://t.co/s95aXUaFmx
My latest blog:“@Mental_Elf: CAM: Many of us are using it, despite poor evidence. Whats going on? http://t.co/PfzWJJU3HW” #WMHD #WMHD2013
@carotomes @Mental_Elf because you call it medicine/therapy! It should be interventions with unknown effectiveness http://t.co/Ny9OqGjVKH
@Theresevilvite @Mental_Elf Excellent point. And I agree that the conventional terminology is unhelpful, but unfortunately well-established.
Interesting @M1ke5myth? “@Mental_Elf: CAM: Many of us are using it, despite poor evidence. Whats going on? http://t.co/fGO5QULSmJ“
Current evidence of complementary & alternative therapies for mental health is limited, so why are they so popular? http://t.co/N6Vrh3G7tl
@Mental_Elf Another great post- is is frustrating & self-defeating sometimes when they group everything under the giant CAM umbrella.
@EdzardErnst Interested in your thoughts on our CAM in mental health blog today http://t.co/N6Vrh3G7tl @carotomes
New SR on CAM for depression & anxiety is “methodologically weak”. We call for better quality CAM research http://t.co/N6Vrh3G7tl #WMHD
Read our top 5 tips for improving the quality of complementary and alternative research in mental health http://t.co/P0r0IFyccu @carotomes
In case you missed it earlier – CAM: Many of us are using it, despite poor evidence. Whats going on? http://t.co/N6Vrh3G7tl
Mental Elf: CAM: Many of us are using it, despite poor evidence. Whats going on? http://t.co/tCOG4wYYmw
#alternativemedicine: Many of us are using it, despite poor #evidence. Whats going on? http://t.co/qLm01Xoxma
CAM: Many of us are using it, despite poor evidence. Whats going on? – The Mental Elf http://t.co/TW1jHxqZwW