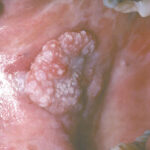
Proliferative verrucous leukoplakia (PVL) is an oral potentially malignant disorder. Patients with this form of oral leukoplakia often have multiple lesions. PVL starts as a white patch that over time progresses to having an exophytic, verrucous appearance. PVL lesions are difficult to treat surgically and have a high rate of malignant transformation. The aetiology of PVL is not fully understood.
The aim of this systematic review was to answer the question: “What are the main clinical features of PVL patients?”
Methods
Searches were performed in PubMed and Scopus databases over a 10-year period ending in September 2018. Studies reporting at least 10 PVL patients that were published in English or Spanish were included. Each paper was read and assessed by three reviewers independently. Each paper was appraised using the Strength of Recommendation Taxonomy (SORT) (Ebell et al., 2004).
Results
- 6 articles, involving 219 patients, satisfied the inclusion criteria.
- 3 of these studies were retrospective cohort studies, 2 were case control studies and 1 was a clinical trial.
- Most of the patients were females, the mean age was 67.4 years.
- Malignant transformation rate varied from 33.3 to 71.4% but methods for evaluating this varied between studies.
Conclusions
This systematic review confirmed that PVL was more prevalent in older women, consistent with other information.
When analyzing the location, we can agree that the most common location is the gingiva and the buccal mucosa, as agreed in other papers.
The findings of this study have to be seen within limitations; the evaluated studies are based on subjective clinical characteristic, and the sample size was limited. There is a lack of randomized controlled trials (RCT), since most of the papers are from series of retrospective cases; therefore, the evidence is not enough, and more studies are needed.
Comments
The authors of this review limited their search by only searching in two databases and limiting to English/Spanish; this means that relevant studies may have been excluded. This review seems to support previous reviews (e.g. Abadie et al., 2015 and Pentenero et al., 2014) concluding that PVL typically occurs in females over the age of 60 and affects the gingivae, buccal mucosa and tongue most commonly. However, due to its limitations it is difficult to draw any further conclusions. One limitation being that the majority of the included studies were retrospective; meaning potentially valuable information was not recorded in some of the studies (e.g. smoking/alcohol status) and due to difficulties with retrospective studies some patients with PVL may not have been captured.
Furthermore, the diagnostic criteria used for PVL varied between some of the included studies. Therefore, this needs to be taken into consideration when interpreting the findings. Villa et al., 2018 described in detail the lack of a standardised approach to the clinical and histological diagnosis for PVL and proposed a new criteria which highlights the importance of clinicopathological correlation aided by sharing clinical photographs with pathologists. However, this important issue of differing diagnostic criteria was not discussed in detail in the current review.
The high malignant transformation rate (MT) of PVL has been previously demonstrated as being up to 63.9% (Pentenaro et al., 2014 and Abadie et al., 2015). However, the authors of this review felt they could not provide good evidence on MT due to limitations in drawing together studies that have followed patients up over different time frames and calculated the MT in different ways.
One included study found Epstein-Barr Virus (EBV) in PVL biopsies (Bagan et al., 2008) and another found higher serum and salivary levels of interleukin-6 (IL-6) in PVL and oral squamous cell carcinoma in comparison to controls (Bagan et al., 2015). However, further research is required to ascertain the nature/aetiological role (if any) of these associations.
PVL is an oral potentially malignant disorder with a high MT rate and patients need close review and repeat biopsies, with many advocating life-long review. However, evidence regarding the aetiology of PVL is weak. The future development and use of an evidence-based standardised diagnostic criteria for both the clinical and pathological diagnosis of PVL would support the correct diagnosis of lesions and the need for more high-quality studies. Further prospective studies are needed to study the aetiology of PVL and future randomised controlled trials to compare treatment approaches.
Links
Primary paper
Torrejon-Moya A, Jané-Salas E, López-López J (2020) Clinical manifestations of oral proliferative verrucous leukoplakia: A systematic review. J Oral Pathol Med 2020 00 1–5. https ://doi.org/10.1111/jop.12999
Other references
Ebell MH, Siwek J, Weiss BD et al (2004). Strength of recommendation taxonomy (SORT): a patient-centred approach to grading evidence in the medical literature. Am Fam Physician 2004 1;6(39) 548-556.
Abadie W, Partington EJ, Fowler CB et al (2015). Optimal Management of Proliferative Verrucous Leukoplakia: A Systematic Review of the Literature. Otolaryngol Head Neck Surg 2015 153(4) 504-511. doi:10.1177/0194599815586779
Pentenero M, Meleti M, Vescovi P et al (2014). Oral proliferative verrucous leucoplakia: are there particular features for such an ambiguous entity? A systematic review. British Journal of Dermatology 2014 170(5) 1039-1047. doi:10.1111/bjd.12853
Bagan JV, Jiménez Y, Murillo J, et al. Epstein-Barr virus in oral proliferative verrucous leukoplakia and squamous cell carcinoma: a preliminary study. Med Oral Patol Oral Cir Bucal. 2008;13:110-113.
Bagan L, Sáez G, Tormos M, Labaig-Rueda C, Murillo-Cortes J, Bagan JV. Salivary and serum interleukin-6 levels in proliferative verrucous leukoplakia. Clin Oral Invest. 2015;20:737-743
Dental Elf 6th Apr – 2020.
Picture Credits
By Aitor III – Own work, Public Domain, Link
