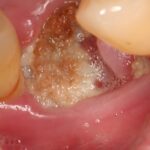
Medication‐related osteonecrosis of the jaw was first described in 2003 in patients receiving bisphosphonates. Subsequently it has been reported in patients taking anti-resorptive and anti-angiogenic medication. Medication- related osteonecrosis of the jaw (MRONJ) is estimated to have a prevalence of 1–15% in oncology patients and 0.001–0.01% in osteoporotic patients. Recently, non-antiresorptive medications such as antiangiogenic inhibitors, immunosuppressants, radiopharmaceuticals, mammalian target of rapamycin (mTOR) inhibitors, and chemotherapeutic drugs have been linked with MRONJ.
The main aim of this review was to assess the association between non-antiresorptive medications and medication‐related osteonecrosis of the jaw (MRONJ).
Methods
Searches were conducted in the Medline/PubMed, Embase and Web of Science databases. English language studies of any design reporting evidence of MRONJ following non-resorptive drug treatment were considered. Two reviewers independently selected studies extracted data and assessed quality using the Newcastle–Ottawa Scale (NOS). Disagreements were resolved by a third reviewer. Odds ratios (OR) and 95% confidence interval (CI) were used to assess the relationship between non-antiresorptive drugs and MRONJ.
Results
- 70 studies (3 cohort studies, 2 clinical trials, 1 case–control study, 2 case series, and 54 case reports) were included.
- 867 cases of MRONJ were included (33% female, 55% male, 12% no gender reported).
- The mean age at diagnosis was 60.6 years (range 19-100).
- mean time of diagnosis was 9.75 months following non-antiresorptive drug therapy.
- Site was reported in 52% of cases, with 35% of cases in the mandible, 14% in the maxilla and 3% in both.
- Breast cancer was the predominant primary disease (15%).
- 14 studies contributed to the meta-analyses (see table below)
| Medication | No. of studies | Odds Ratio (95% CI) |
| Corticosteroids | 11 | 0.61 (0.39 to 0.82) |
| Chemotherapy | 11 | 0.59 (0.51 to 0.67) |
| Monoclonal antibody | 7 | 0.32 (0.10 to 0.58) |
| Anti-tyrosine kinase inhibitor | 4 | 0.17 (0.03 to 0.36) |
| Aromatase inhibitor | 3 | 0.62 (0.41 to 0.82) |
| Immunomodulators | 3 | 0.54 (0.32 to 0.75) |
Conclusions
The authors concluded: –
A significant association existed between MRONJ and non-antiresorptive drugs. However, due to the availability of limited evidence, the findings should be interpreted with caution. The risk of developing MRONJ should be assessed for each drug individually to allow an improved prediction of MRONJ occurrence. Dentists should be aware of these drugs and proper management guidelines should be established. Unlike bisphosphonates, majority of the non-antiresorptive drugs mentioned in the review have a shorter half-life which might allow the dentist to apply the principle of “drug holiday” following concurrence from the drug prescribing clinician.
Comments
The authors have searched 3 major databases however as they have only included English language studies, they may have excluded some relevant papers, a fact that they acknowledge in the discussion. A large number of studies were included in the review with a majority (77%) being case studies. The quality of the case report studies was not assessed although guidelines for case reports are available ( CARE guidelines ) which could improve their usefulness. The 14 studies included in the meta-analyses were quality assessed using the NOS tool with 10 being rated as fair and 4 as good. The link between MRONJ and chemotherapeutic agents and corticosteroids was higher than the other medications however, the authors note than many on the patients were receiving multiple drug therapies. Overall while the review provides a reasonable summary the amount of the evidence is limited as is the quality consequently additional evidence from well designed and conducted studies are needed to improve our understanding of the relationship between MRONJ and non-antiresorptive drug therapy.
Links
Primary Paper
Suryani IR, Ahmadzai I, Shujaat S, Ma H, Jacobs R. Non-antiresorptive drugs associated with the development of medication-related osteonecrosis of the jaw: a systematic review and meta-analysis. Clin Oral Investig. 2022 Jan 11. doi: 10.1007/s00784-021-04331-7. Epub ahead of print. PMID: 35013781.
Other references
Dental Elf – 18th Oct 2017
Medication-related osteonecrosis of the jaw (MRONJ): treatment and prevention
Dental Elf – 22nd Jul 2020
Photo Credits
By Coronation Dental Specialty Group – Own work, CC BY-SA 4.0, Link
