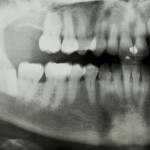
The surgical removal of third molars (wisdom teeth) is one of the commonest operations performed. It is usually carried out because of infection associated with a partially erupted and impacted tooth. The aim of this update to a Cochrane review was to compare the relative benefits and risks of different techniques for undertaking various aspects or stages of the surgical extraction of mandibular wisdom teeth.
Searches were conducted in Cochrane Oral Health Group’s Trials Register, CENTRAL, Medline, Embase, Clinical Trials.gov and the WHO International Clinical Trials Registry Platform without restriction of language or date of publication. Randomised controlled trials (RCTs) comparing surgical techniques for removal of mandibular wisdom teeth were considered. Standard Cochrane methodological approaches were used. The primary outcomes considered were; dry socket; wound infection; permanent alteration of sensation to tongue or lip; fractured mandible.
- 35 trials (2569 patients) were included
- 21 trials were assessed at high risk of bias, the other 14 as unclear.
- Compared with envelope flaps,
- Triangular flaps were associated with a 71% reduction in alveolar osteitis at one week (RR 0.29, 95% CI 0.11 to 0.78; three trials, moderate quality) and reduction in pain at 24 hours (MD -0.21, 95% CI -0.32 to -0.10; two trials, moderate quality)
- There was no evidence of a difference in overall infection rates, in maximum mouth opening or in permanent sensation.
- However, there was some evidence that residual swelling after one week was slightly increased in the triangular flap groups compared to envelope flap types (MD 0.66 mm, 95% CI 0.26 to 1.07; two trials, low quality).
- No data was found on temporary sensation, or adverse events. There was low quality evidence from two studies, looking at the use of a retractor during third molar surgery, to indicate more cases of temporary altered sensation (up to one month) when a retractor was used (Peto OR 5.19, 95% CI 1.38 to 19.49; two trials, low quality).
- There was evidence that secondary wound closure was associated with reduced pain at 24 hours (MD 0.79, 95% CI 0.35 to 1.24; four trials, moderate quality) and slightly reduced swelling after one week (MD 0.33, 95% CI 0.09 to 0.57; seven trials, moderate quality).
- There was some evidence that the use of a surgical drain was associated with less postoperative swelling (MD -0.90, 95% CI -1.62 to -0.19; five trials, moderate quality) and greater maximum mouth opening one week after surgery (MD 3.72 mm, 95% CI 2.84 to 4.59; two trials, moderate quality).
- Although two RCTs compared coronectomy with complete extraction, flaws in the design and the unit of analysis of these studies meant that there were no reliable data available for inclusion.
The authors concluded
The thirty-five included trials looked at a range of different surgical techniques. The comparisons related to seven broad aspects of the surgical procedures for impacted mandibular third molars: type of surgical flap raised, use of retractors, techniques for bone removal, wound irrigation, wound closure, wound drainage, and complete/incomplete tooth removal. The quality of the body of evidence for each of these comparisons was very low to moderate due to the small number of trials and patients, and the majority of the trials being at high risk of bias (65%) with the remainder at unclear risk of bias. The evidence for making changes to surgical practice is therefore limited. However, it is useful to describe the state of the research evidence supporting practice so that surgeons can make an informed choice in adopting new techniques, or continuing with established techniques.
Comment
As the authors note although they were able to include 35 trials there were only one of two studies that evaluated a given element of the surgery. The quality of the available evidence in general was only moderate to low and the authors highlight that although blind outcome assessment was possible this was only carried out in about a third of the trials. The authors also discuss two 2012 reviews , one by Carrasco-Labra et al (Dental Elf 25th June 2012), the other by Long et al (Dental Elf 12th June 2012), the findings of both these reviews are in disagreement with this review.
Links
Coulthard P, Bailey E, Esposito M, Furness S, Renton TF, Worthington HV. Surgical techniques for the removal of mandibular wisdom teeth. Cochrane Database of Systematic Reviews 2014, Issue 7. Art. No.: CD004345. DOI: 10.1002/14651858.CD004345.pub2.

Available evidence for various aspects of surgical removal of 3rd molars is very low to moderate http://t.co/ORF7RlucID via @TheDentalElf