
COVID-19 suddenly brought a lot of things to a halt back in March 2020. One of the places that has been affected the worst, not just in the UK but worldwide, have been care homes and nursing homes. Note, nursing homes are a specific type of care home providing special medical support to its residents, where required.
In fact, roughly half of all COVID-19 deaths so far in the UK have been reported in care homes (ONS, 2020). Considering that care home residents are some of the most vulnerable members of our society, one would have expected better preparations for care homes by the government, once we knew COVID-19 was going to have a significant impact on us.
As a result, care homes took their own individual approaches to providing care, whilst all closed down to the public in March. Family members were unable to visit their relatives for several months, and only recently some care homes have reopened, whilst others have closed down again. It is still unknown how these closures have affected residents specifically. Considering public health measures of social distancing and personal protective equipment (PPE), staff are likely to have significantly changed the ways in which care is provided, but it’s unclear how this has impacted on residents. Have social activities, such as coffee mornings or arts and crafts activities continued in groups, or have residents stayed in their rooms for months?
We know that social engagement is vital for good general well-being across the lifespan (Feng et al., 2020). Suddenly removing the ability to see family members and likely engaging with fellow residents, whilst also often suffering from cognitive deficits (Ulbricht et al., 2017), COVID-19 is likely having a detrimental impact on residents.
As one of the very first studies to have looked at the impact of social engagement on nursing home residents during the pandemic, for this blog I will be taking a look at a study from the Netherlands by Verbeek and colleagues (2020). The Netherlands generally has a very advanced care system, so it’s no surprise that one of the first studies on this topic comes from Holland!
What is interesting is that the Netherlands has published national guidance on allowing visitors back into nursing homes, something that is clearly lacking in the UK. In this guidance, residents are only allowed one designated visitor, with visitors having to agree the frequency of their visits with the nursing home in advance. In addition, visitors are required to wear face masks, be free from COVID-19 symptoms, and they can only meet at a 1.5 metre distance. Moreover, organisations need to have sufficient PPE and staffing to allow guidelines to be efficiently implemented.
So let’s see what Verbeek and colleagues found and how Dutch nursing homes are opening up to the public again.

Care homes have been affected the worst during the COVID-19 pandemic with half of all UK deaths being care home residents.
Methods
26 nursing homes participated in the study. Nursing homes were selected via the Local Area Health Authority, which ensured that they were representative for the general Dutch nursing home population.
In each nursing home, one representative who knew the most about the workings of the nursing home and the impact on residents was asked to completed a 30-item electronic questionnaire and participate in a telephone interview with the research team. Participants included nursing home managers, registered nurses, and local quality or policy officers.
In the questionnaire, participants were asked about the general nursing home characteristics. In the interview, they were asked about the impact of allowing family visitors back in to visit the residents, as well as any barriers and facilitators.
Results
All nursing homes participated in the interview, with 24 questionnaires being completed. In the first week, 57% of residents across the nursing home had received family visits. Whilst the majority of nursing homes allowed visitors for all residents, some nursing homes had special rules; such as only those residents who needed visits the most were allowed to receive them. It is unclear how this was judged, but it seems mostly due to logistics and organising safe ways of meeting visitors on nursing home premises.
Interestingly, not all staff wore face masks or other PPE. In some nursing homes, only visitors had to wear face masks. Visitors were tested for active COVID-19 symptoms in most nursing homes, with some nursing homes having asked about the symptoms on the phone a few days before the visit.
All nursing homes reported the positive impact that family visits had on the residents. Seeing each other face-to-face again was hugely beneficial to both residents and visitors. However, having to keep a physical distance and not being able to give someone a hug, for example, was considered difficult, but still an improvement on the remote solutions that some nursing homes had come up with during the first few months of the pandemic.
Sadly, some residents did not recognise their family members or any visitor, due to the prolonged period of not having been able to see them.
Whilst no new COVID-19 infections were reported in the participating nursing homes in the three weeks after visits were allowed, some family members had been too worried to visit because of the fear of bringing the virus into the nursing home.
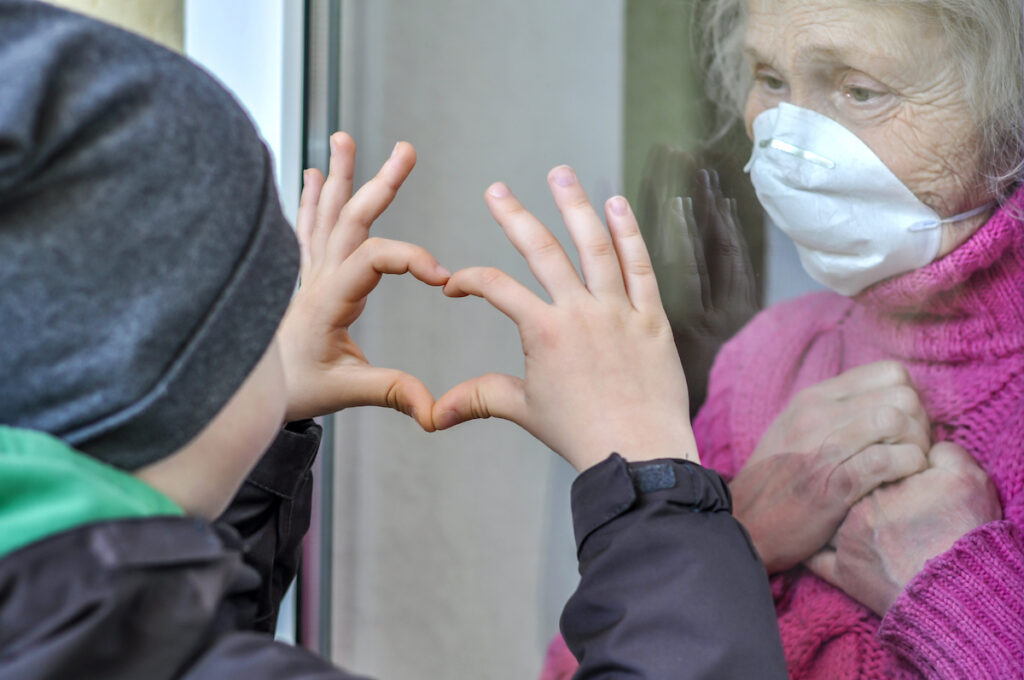
Seeing family members again had a huge impact on residents’ well-being, with nursing homes providing different access rights to residents – not all residents were allowed to see visitors.
Conclusions
These clear guidelines seemed to have helped nursing homes across the Netherlands to enable social interaction again for their residents. Although visits were under strict scrutiny and imposed guidance, including wearing face masks, keeping a distance, length of visit and where people could meet (usually only the resident’s own room), being able to see family members again had huge positive effects on residents. As visits were still restricted to the residents’ rooms in most nursing homes, Verbeek et al. (2020) recommend an adaptation to the guidelines, recommending that visits can also take place outdoors, enabling a vital change of scenery.

This research suggests that Dutch guidance on allowing visitors back into nursing homes has been effective, but should also include use of outdoor space as staying within the same room 24/7 for the residents did not feel natural.
Strengths and limitations
This is a strong study, having taken place super quickly after national guidelines were imposed. The study benefits for example from having recruited nursing homes that are representative of the Dutch population, with each region being represented. In addition, a member of staff was purposefully selected based on their knowledge of the organisation and residents, as opposed to just approaching any member of staff in each nursing home.
Considering the tight time frame, it is impressive to see this research out so quickly. Possibly because of the tight COVID-19 time frame, a few things could have been addressed also. For example, gains in well-being of the residents are based on staff interviews and their perceptions of how residents feel. Whilst it is of course difficult to measure well-being quantitatively with residents, many of whom have cognitive deficits such as dementia, the benefits reported by staff need to be considered with some caution. However, considering that staff sees the residents every day, they are likely best placed to provide an insight into their quality of life.
It would also have been important to speak to family members who were visiting residents, to explore their experiences of the new guidelines, and generally their experiences of having been unable to see their relatives for a substantial period of time. For example, in our study in the UK we interviewed 50 unpaid carers and people living with dementia residing in the community, some of which cared for a person with dementia living in a care home. Amongst others, we found that unpaid carers faced difficult decisions about receiving paid carers into the home (Giebel et al., 2020). Some decided to discontinue receiving paid care, due to the risk of the virus transmission. Therefore, many ended up being more burdened. This shows that it is important to gain different perspectives, and future research should explore how family members of care home residents have experienced the pandemic so far and changes in visiting rights.

The study benefits from having recruited nursing homes across the Netherlands, but there is limited understanding on how family members have experienced visiting their relatives.
Implications for practice
Although this was only a first foray into re-enabling social visits for residents again, the positive impact and ability to adhere to guidelines suggests that the UK and other countries should learn from the Dutch care system and implement similar national guidelines. Currently, each care home and nursing home in the UK for example has their own ways of dealing with the pandemic, with only some enabling social visits. However, what is needed is a clear national guidance on how care homes should operate during the pandemic, to ensure that vital social interactions and the quality of care are not compromised.
In terms of research implications, we still need to fully understand how the lockdown and various public health measures have impacted on residents and their family members. Considering the sudden drastic changes to how care could be provided and how people could interact with one another, both residents and family members, but also staff, have likely been impacted severely, and possibly long-lasting.

Other countries could adapt these Dutch guidelines to support nursing homes who wish to allow family members back to visit their loved ones.
Statement of interests
None.
Links
Primary paper
Verbeek, H., Gerritsen, D., Backhaus, R., de Boer, B., Koopmans, R. and Hamers, J., 2020. Allowing Visitors Back in the Nursing Home During the COVID-19 Crisis: A Dutch National Study Into First Experiences and Impact on Well-Being. Journal of the American Medical Directors Association, 21(7), pp.900-904.
Other references
Feng Z, Murray Cramm J, Nieboer AP. Social participation is an important health behaviour for health and quality of life among chronically ill older Chinese people. BMC Geriatrics 2020
Giebel, C., Hanna, K., Cannon, J., Eley, R., Gaughan, A., Komuravelli, A., Shenton, J., Callaghan, S., Tetlow, H., Butchard, S., Limbert, S., Whittington, R., Rogers, C., Rajagopal, M., Ward, K., Shaw, L., Hughes, M., Gabbay, M. (2020). Decision-making for receiving paid home care for dementia in the time of COVID-19: A qualitative study. BMC Geriatrics.
Office for National Statistics (ONS). Deaths involving COVID-19 in the care sector, England and Wales: deaths occurring up to 12 June 2020 and registered up to 20 June 2020 (provisional). London, England: ONS, 2020.
Ulbricht CM, Rothschild AJ, Hunnicutt JN, Lapane KL. Depression and cognitive impairment among newly admitted nursing home residents in the USA. International Journal of Geriatric Psychiatry 2017;32(11): 1172-1181.
Photo credits
- Photo by Erik Mclean on Unsplash
- Photo by Martin Kníže on Unsplash
- Photo by Ekaterina Shakharova on Unsplash
