
Individuals with mental health problems smoke more heavily than the general population, thus contributing to as much as 43% of tobacco consumption in the UK (McManus et al, 2009).
While the high prevalence of smoking, heavier addiction rates, and smoking-related illnesses contributing to increased morbidity and mortality in this group have been studied extensively, very little research has been conducted into the economic disadvantages as a result of ill-health in smokers with mental illness (RCP, 2013; Wu et al, 2014).
Methods
The authors of a new study published in Tobacco Control (Wu et al, 2014), use economic modeling to investigate different components of the financial burden of smoking in individuals with mental disorders. These costs were assessed in UK adults in 2009-2010 from both the National Health Service (NHS) and Personal Social Services. The different components investigated were:
- Direct healthcare costs: costs of resources consumed as a result of treating smoking related diseases, including hospital admissions, outpatient visits, GP and practice nurse consultations, and prescriptions for smoking related diseases
- Indirect morbidity costs: economic value of lost productivity from increased rates of work absences associated with smoking
- Indirect mortality costs: additionally, the authors estimated the economic cost due to years of potential life lost due to smoking

People with mental health disorders are much more likely to smoke than those without mental illness. View Table 1: Prevalence of mental disorders and associated smoking status
Results
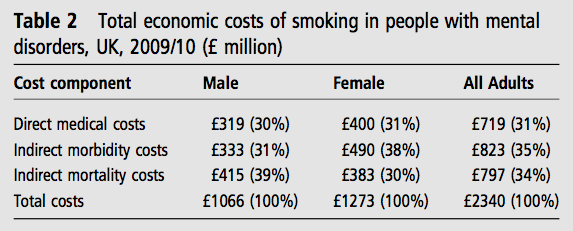
The authors estimated 3 million UK adults with mental disorders (>16 years old) were also smokers in 2009-2010, with the total smoking-attributable costs for this group estimated at £2.34 billion (see table 2 below taken from the paper).
Direct healthcare costs
- A total of £719 million was spent treating smoking-related disease among people with mental health disorders
- £352m of which were due to hospital admissions, while other cases were treatments of cancer, cardiovascular disease and respiratory diseases
- GP and nurse consultations cost £116m, with a total of 18.8 million prescriptions issued for smoking-related diseases among individuals with mental disorders generating a cost of £179m
Indirect morbidity costs
- A total of £823 million due to productivity loss and work absence
- 44% of the costs incurred were from those with mixed depression and anxiety disorder, 23% incurred from individuals with generalised anxiety disorder, and 14% from those with depression
- A relatively small (0.06%) proportion of indirect costs were incurred from those with serious mental illnesses, as only 28% were in regular work
Indirect mortality costs
- A total £797 million was associated with premature mortality
- A total of 35,228 of potential working years of life were lost in individuals with mental illnesses
- The estimated total life years lost due to smoking-related diseases were 192,005
- Nearly 50% or £366m of the indirect mortality costs were associated with individuals with mixed anxiety and depressive disorder
Discussion
In this paper, Wu et al estimate for the first time that there are approximately 3 million smokers in the UK with mental illness, and the direct cost of treatment to the NHS in this population was £719 million in 2010. A study by Callum et al (2011) estimated an annual cost of £200 per general population smoker to the NHS, while Wu et al estimate an annual cost of £320 per smoker with a mental illness.
The authors stress that the estimated economic costs of smoking are almost entirely preventable with the use of smoking cessation interventions. Furthermore, smoking cessation is one of the most cost-effective public health interventions, costing the NHS £220 per quitter (Woolacott et al., 2002; Statistics on Smoking, 2013), although the effectiveness of different interventions vary among individuals with mental illness compared to the general population (RCP, 2013). (Check out our previous blogs on smoking cessation interventions in mental illness).
This is precisely why future research needs to focus on both effective and cost-efficient cessation treatments available for individuals with mental disorders. As individuals with mental illness are known to be as motivated as the general population to quit smoking, but due to mental health problems, may have more difficulties quitting.
Hopefully this study by Wu et al will shine some light on the significant economic costs due to smoking in individuals’ with mental illness, and thus help to inform and influence policy-makers in the reduction of smoking.

Quitting smoking when mentally ill is easier said than done
Links
Wu Q, Szatkowski L, Britton J & Parrott S. Economic cost of smoking in people with mental health disorders in the UK. Tobacco Control. 2014; 0:1-7. [Abstract]
McManus S, Meltzer H, Brugha T, et al. Adult psychiatric morbidity in England, 2007. Results of a household survey (PDF). London: The NHS Information Centre for Health and Social Care, 2009.
The Royal College of Physicians. Smoking and mental health (PDF). London: RCP, 2013.
Callum C, Boyle S, Sandford A. Estimating the cost of smoking to the NHS in England and the impact of declining prevalence. Health Econ Policy Law 2011;6:489–508. [PubMed abstract]
Woolacott N, Jones L, Forbes C, et al. The clinical effectiveness and cost-effectiveness of bupropion and nicotine replacement therapy for smoking cessation:a systematic review and economic evaluation. Health Technol Assess 2002;6:1–245.
Statistics on Smoking: England, 2013. The Health And Social Care Information Centre.


RT @Mental_Elf: New study estimates that UK smokers with mental illness cost the economy £2.34 billion http://t.co/MU03vTYXqj
New study estimates that UK smokers with mental illness cost the economy £2.34 billion: This new study estimat… http://t.co/wxw3B4628d
@Mental_Elf and how much tax do they pay on their cigs?
@Mental_Elf How about showing stats for alcohol &/or drug misuse and mental health and how much they cost the economy?
@Mental_Elf smoking and mental health. There is no scientific value to this study, as there was no measure of the value of smoking to users
@Mental_Elf thanks for covering this #research on #smoking & #mentalhealth by Qi Wu @MHARG_york from @HealthSciYork
I blogged for the @Mental_Elf on the estimated economic costs of smokers with mental illness (£2.34b): http://t.co/Rps3hAeY3q
Today @MegEliz_ looks at the economic cost of smoking in people with mental health disorders in the UK http://t.co/74it0L4vCn
@Mental_Elf @MegEliz_
Lisa Eden liked this on Facebook.
RT @Mental_Elf: People with mental health disorders are much more likely to smoke than those without http://t.co/74it0L4vCn
UK smokers with mental illness cost £2.34 billion http://t.co/7y4iRJjA7W
New study estimates there are approximately 3 million smokers in the UK with mental illness http://t.co/74it0L4vCn
@Mental_Elf I managed to quit this year while fighting depression/anxiety. One of the hardest things I’ve ever had to do.
Mental Elf: New study estimates that UK smokers with mental illness cost the economy £2.34 billion http://t.co/8UMMfmksi3
Vincent Blyth liked this on Facebook.
The Mental Elf liked this on Facebook.
Individuals with mental health problems smoke more heavily than the general population – See more at: http://t.co/W0Gtu8YAIa
Smoking cessation is one of the most cost-effective public health interventions http://t.co/74it0L4vCn
RT @Mental_Elf: People with mental health problems consume 43% of UK tobacco http://t.co/74it0L4vCn
RT @Mental_Elf: Don’t miss: New study estimates that UK smokers with mental illness cost the economy £2.34 billion http://t.co/74it0L4vCn #…
Rat @Mental_Elf: People with mental health problems consume 43% of UK tobacco http://t.co/3K5sBr2o2O via @DrKateLovett
RT @Mental_Elf: Research needs to focus on effective & cost-efficient smoking cessation treatments for ppl with mental disorders http://t.c…
New study: UK smokers with #mentalhealth problems cost economy £2.34 bn http://t.co/UpZRZHwdHZ via @dmcdaid @Mental_Elf
Nicola Davies liked this on Facebook.
Nicola Davies liked this on Facebook.
Vincent Blyth liked this on Facebook.
The Mental Elf liked this on Facebook.
Lisa Eden liked this on Facebook.
If they are smoking just 10 cigarettes a day, they each contribute £877 in tax per annum, so using the figures above are actually benefitting the economy by nearly £1.7 billion per annum! (£877-£320)x 3 million. http://www.thisismoney.co.uk/money/news/article-1633429/Calculator-tax-pay-beer-wine-cigarettes-spirits.html