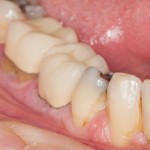
Indirect restorations provide either partial (inlays, onlays, veneers) or full coverage restorations (crowns or fixed partial dentures) to restore tooth form and function resulting from disease or trauma. While tooth preparation and cementation are essential steps for indirect restoration, they may damage pulp vitality.
The aim of this review was to investigate the incidence of and influential factors on pulp necrosis and periapical pathosis of vital teeth following indirect restorations.
Methods
A protocol was registered with the PROSPERO database. Searches were conducted in the CINHAL, Cochrane Library, Embase, Medline/PubMed and Web of Science core collection, supplemented by a search of Google Scholar (first 300 results) and the Open Grey database. Clinical trials (randomised [RCT] and non- randomized[nRCT]) and cohort studies of indirect dental restorations (single-unit and/or fixed partial dentures [FPD]) with an endodontic diagnosis of teeth were considered. Two reviewers independently screened and selected studies assessing methodological quality using the using the Joanna Briggs Institute (JBI) quality appraisal checklist and the Newcastle–Ottawa Quality Assessment Scale (NOS). Data was extracted by two independent reviewers and overall incidences of pulp necrosis and periapical pathosis following indirect restorations were calculated using a random effects model. The GRADE approach was used to assess the certainty of the evidence.
Results
- 37 studies (5 RCTs, 32 cohort) involving 11,615 teeth were included.
- 4 of the RCTs were considered to be at low risk of bias and one at moderate risk.
- 16 of the cohort studies were considered to be at low risk of bias and 16 at moderate risk.
- Pulp necrosis was reported in all studies and periapical pathosis in 15 studies.
- Meta-analysis for overall incidence of pulp necrosis and periapical pathosis are shown in table below.
| No. of studies (teeth) | Incidence % (95%CI) | |
| Pulp necrosis | 37 (11,615) | 5.02 (3.70 to 6.52) |
| Periapical pathosis | 15 (5,376) | 3.63 (2.05 to 5.63) |
- Meta-analyses for influential factors on incidence of pulp necrosis are shown in the table below.
| No. of teeth | Pulp necrosis incidence % (95%CI) | ||
| Assessment method | |||
| Subjective | 3181 | 3.91 (1.86 to 6.66) | |
| Objective | 6581 | 5.66 (3.71 to 7.99) | |
| Radiographic | 1853 | 4.95 (2.43 to 8.29) | |
| Temporary cement | |||
| Eugenol‐based | 7043 | 3.34 (1.66 to 5.58) | |
| Eugenol‐free | 639 | 5.77 (3.72 to 8.24) | |
| Temporisation duration | |||
| ≤ 2 weeks | 1907 | 1.47 (0.81 to 2.31) | |
| > 2 weeks | 2280 | 4.25 (1.28 to 8.85) | |
| Impression material | |||
| Polyether | 2985 | 4.02 (2.47 to 5.92) | |
| Polyvinyl siloxane | 636 | 3.17 (1.55 to 5.34) | |
| Restoration material | |||
| Ceramic | 460 | 5.59 (1.55 to 5.34) | |
| Porcelain‐fused‐to‐metal | 1980 | 5.71 (2.89 to 9.12) | |
| Permanent cement | |||
| Resin | 738 | 3.37 (1.90 to 5.23) | |
| Glass ionomer cement | 182 | 5.33 (2.56 to 9.03) | |
| Zinc phosphate | 1387 | 4.92 (3.85 to 6.20) | |
| Post-treatment follow‐ up | |||
| ≤ 5 years | 5532 | 3.53 (2.10 to 5.31) | |
| 6–10 years | 2443 | 5.53 (3.74 to 7.64) | |
| > 10 years | 3640 | 6.74 (2.82 to 12.18) | |
| Clinical expertise | |||
| Undergraduate students | 1604 | 5.68 (2.16 to 7.49) | |
| General practitioners | 2113 | 4.44 (2.16 to 7.49) | |
| Prosthodontists | 3834 | 1.87 (0.84 to 3.31) | |
- The certainty of evidence for all outcomes was assessed as low.
Conclusions
The authors concluded: –
With a low-level of evidence, this study indicated that the incidence of pulp necrosis and periapical pathosis in vital teeth following indirect restorations was relatively low. Moreover, single-unit and multiple-unit restorations had the same level of impact on pulp necrosis, although single-unit restorations demonstrated a lower incidence of periapical pathosis than FPD. Many factors can influence pulp necrosis and periapical pathosis, although not all have been examined in this work. Thus, these factors must be carefully considered when planning indirect restorations.
Comments
The authors preregistered a protocol for the review and conducted and searched a wide range of databases. Thirty two of the 37 included studies were of a cohort design, and it is unclear whether they were prospective or retrospective and they are more likely to suffer from attrition and selection bias which should be taken into consideration when assessing the findings. Individual meta-analyses for a range of potential influential factors were conducted which included fewer studies and teeth so should also be interpreted cautiously.
Links
Primary Paper
Al-Manei KK, Alzaidi S, Almalki G, Al-Manei K, Almotairy N. Incidence and influential factors in pulp necrosis and periapical pathosis following indirect restorations: a systematic review and meta-analysis. BMC Oral Health. 2023 Apr 2;23(1):195. doi: 10.1186/s12903-023-02826-1. PMID: 37009911; PMCID: PMC10069144.
Review protocol on PROSPERO
Other references
Dental Elf – 7th Oct 2014
Composite resin restorations: no good evidence to assess impact on dental pulp
Dental Elf – 21st Jul 2021
Dental Elf – 1st Aug 2012
