
Patients with chronic somatic diseases face distinct challenges in accessing mental health services. Physical limitations in particular make it difficult for these people to travel to a clinic to receive face-to-face therapy.
As a consequence, even if studies showed that cognitive behavioral therapy (CBT) may be an effective intervention for chronic somatic conditions, there are doubts over whether it could be implemented on a large scale. An alternative is internet-based cognitive behavioral therapy (ICBT), which has been shown as efficient for various psychological conditions. Usually, ICBT takes the form of an online self-help intervention, guided by a therapist.
In a recent meta-analysis published in the Journal of Medical Internet Research, van Beugen and collaborators analysed the effectiveness of guided ICBT in chronic somatic conditions.
Methods
The authors included randomised clinical trials (RCTs) or equivalence trials in which CBT was provided using the Internet as the principle means of communication, and under guidance from a therapist. Studies were included if they focused on adults with an existing chronic somatic condition (for instance, a condition expected to last a year of longer, which limits what the patient can do and/or requires ongoing medical care). Studies were excluded if the main focus of the intervention was achieving lifestyle changes, such as increasing levels of exercise.
Outcomes were grouped in three categories, considered relevant for this patient group:
- General psychological outcomes of depression, anxiety, and distress
- Disease related physical outcomes related to symptom severity, such as pain, fatigue or headache
- Disease-related outcomes concerning the impact of a chronic somatic condition on daily life such as disease-specific distress and disease-specific quality of life
Included studies were assessed for methodological quality, using the following criteria from the Risk of Bias Assessment tool developed by Cochrane Collaboration: selection bias (adequate randomization and concealment of allocation), performance bias (blinding of subjects and study personnel), detection bias (blinding of outcome assessors), reporting bias (handling of missing data), and attrition bias (reasons for withdrawal in all conditions).
For studies comparing ICBT with a passive control condition (defined as a waiting list, treatment as usual or treatment that is theorized as not leading to changes in the outcomes of interest), the authors considered only between-group results. For equivalence trials, in which the comparison intervention is considered to be as effective as an active, established treatment, and for studies with three-arms, both between-group effects and main effects were reported. When it was possible, intent-to-treat (ITT) results were used. In these analyses, all randomized patients are analyzed regardless of adherence to the study protocol.
Effect sizes (ES) were calculated as standardized mean differences by subtracting the difference in means in the ICBT group from the difference in means in the control group and dividing the result by their pooled standard deviation. Values of 0.20, 0.50 and 0.80 correspond to small, moderate and respectively large ES.
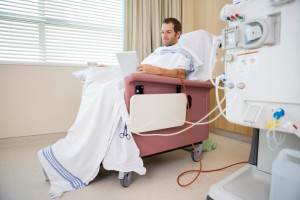
Patients with chronic physical problems might have difficulties accessing face-to-face therapy, so internet-based interventions might be promising alternatives.
Results
23 studies met the inclusion criteria and were included in the meta-analysis. Patient populations included chronic pain, headache, tinnitus, irritable bowel syndrome, diabetes, breast cancer, epilepsy, neurological disorders and a heterogenous patient population.
- Drop-out rates were high (around 18%) and differed widely across studies, ranging from 2 to 57%. This was particularly true in the ICBT groups
- Overall, the quality of the included studies was suboptimal, and for many of the bias criteria assessed, there was incomplete information:
- There was adequate concealment of allocation of participants in the treatment groups in only 35% of the studies, with the rest having a high risk of selection bias or simply not reporting information about this
- Interestingly, none of the included studies reported adequate blinding of participants, personnel and outcome assessors
- More than half of the studies had incomplete outcome data and did not conduct intent-to-treat analysis, which would have reduced risk for this type of bias
- Barely one third of the studies had been previously registered on portals like clinicaltrials.gov, leaving uncertainties about the risk of selection bias
- The effects of ICBT versus a passive control group were small and significant for general psychological outcomes, ranging from 0.17 to 0.21
- For disease-related physical outcomes, the results were highly variable. We also noted that with the exception of pain, the other physical outcomes resulted from the combination of a very small number comparisons (most times 2 or 3), rendering results very unstable
- For disease-related impact on quality of life, small but significant effects were found for disease-related distress, and large effects for disease-specific quality of life. However, in the latter case, again only 3 comparisons contributed to this effect, making it unstable
- Three equivalence trials compared ICBT to an active CBT control condition (face-to-face group therapy, online stress management without CBT, and ICBT with added telephone contact) and found no differences on any of the considered outcomes.

The benefits of ICBT (over control conditions) for disease-related physical outcomes were widely variable.
Conclusions
The authors conclude that:
The current review indicates that ICBT interventions improve both psychological and disease-related physical outcomes in patients with chronic somatic conditions, with small-to-medium effect sizes.
They also emphasize that:
(…) interventions of longer duration may be more effective on psychological outcomes such as depression, which implies that tailoring the duration of interventions to specific problems may be appropriate.
Unfortunately, this is a flawed meta-analysis with a number of very important limitations (highlighted below). It is my belief that not only do these limitations preclude drawing any clear conclusions from this data, but also that the authors are offering an overly positive interpretation of their results, insufficiently acknowledging the serious effects of these limitations.
Limitations
- Most of the included studies had either a high or an unclear risk of bias for most of the criteria considered, which casts serious doubts about the validity of their reported results. It is particularly disturbing that studies conducted using the Internet rarely employ trial pre-registration
- Publication bias was not analyzed at all. The authors argued that studies with negative results were also included in the meta-analysis, which they claim might represent a mitigating factor for the risk of publication bias. However, this is not really a valid argument and the authors could have resorted to a number of methods to at least give some indication regarding the presence of publication bias
- What the authors defined as passive and active control conditions is also very problematic and this raises doubts about the entire set of results. For instance, considering care as usual as a passive control condition is extremely debatable. On the other hand, considering Internet stress management as an active condition is also questionable
- The authors examined many different outcomes and the number of comparisons contributing for most of these outcome categories is very small (in most cases, 2 or 3 comparisons), implying that the reported results in these cases are very unstable and should probably not be interpreted at all

Important limitations of this meta-analysis include studies with high or uncertain risk of bias, not examining publication bias and reporting many different outcomes.
Links
Van Beugen S, Ferwerda M, Hoeve D, Rovers MM, Spillekom-van Koulil S, van Middendorp H, Evers AW. (2014) Internet-based cognitive behavioral therapy for patients with chronic somatic conditions: a meta-analytic review. J. Med. Internet Res. 16, e88.


@Mental_Elf Like many icbt / ccbt outcome studies, high drop out, minimal effect sizes. Therapy is about human relationships, not just info.
RT @Mental_Elf: Internet-based CBT for chronic somatic conditions http://t.co/qUUoOJtaKl
Internet-based CBT for chronic somatic conditions: problematic meta-analysis offers an overly enthusiastic app… http://t.co/Rnv1YH9uUU
The Mental Elf liked this on Facebook.
Internet-based CBT for chronic somatic conditions: problematic meta-analysis offers an overly enthusiastic appraisal http://t.co/mo5R5BXj7e
My new blog for the Mental Elf criticizes a meta-analysis on ICBT for chronic somatic disorders http://t.co/J1ilBLitu1
Today @Zia_Julia critically appraises a review of Internet-based #CBT for people with chronic #somatic conditions http://t.co/VmIiv1xZhS
Kehksha Azam liked this on Facebook.
Step away from the pointless and highly heterogeneous meta-analysis. Step away. http://t.co/icYdfzc01Z
New meta-analysis finds benefits of ICBT (over control) for disease-related physical outcomes were widely variable http://t.co/VmIiv1xZhS
@Mental_Elf @NeilOConnell #Its all about what’s in the jelly in our heads
New MA says ICBT helps with chronic somatic conditions. Our blog says hang on, it’s too early to tell http://t.co/VmIiv1xZhS
Mental Elf: Internet-based CBT for chronic somatic conditions: problematic meta-analysis offers an overly… http://t.co/g6xzrfPpLZ
‘Sue Mario liked this on Facebook.
Don’t miss: Internet-based CBT for chronic somatic conditions http://t.co/VmIiv1xZhS #EBP
“@Mental_Elf: Don’t miss: Internet-based CBT for chronic somatic conditions http://t.co/MJUxAS6dsp #EBP” too much positive spin on IBT
RT @Iain_caldwell: Internet-based CBT for chronic somatic conditions: problematic meta-analysis offers an overly enthusiastic appraisal htt…
Angie Lock liked this on Facebook.
Christina Armstrong-Graham liked this on Facebook.