
There has been a depressing familiarity about the findings of reports into the quality of healthcare for people with learning disabilities, all highlighting concerns about treatment in NHS hospitals, poor communication, incorrect assumptions about quality of life and poor understanding by healthcare professionals.
Most recently, Tuffrey-Wijne et al looked at factors affecting promotion of safer environments for patients with learning disabilities in NHS hospitals and found a lack of effective systems for sharing information, poor coordination of accountability and responsibility for support to patients with learning disabilities and a need for better establishment of learning disability liaison nurse roles.
This month saw the publication by the Royal College of Psychiatrists, Royal College of General Practitioners and the Health Quality Improvement Partnership of the feasibility study of a national audit of learning disabilities.
The aims were to look at the acceptability of data collection methods and the role that audit data could play in raising the standard of care and to make recommendations for how a future national audit could be conducted.

Two key questions addressed: could an audit generate reliable data and would it be effective way of driving improvement?
Two key questions were addressed:
- Would a national clinical audit be able to generate reliable data about the quality of care provided by healthcare organisations to people with learning disabilities
- Is a national clinical audit an effective way of driving improvement within NHS organisations
The findings of this study and feedback collected from study sites and stakeholders indicate that the answer to both questions is yes.
Method
What they did was to work with 12 primary care practices to examine data for 794 people with learning disabilities. They also worked with nine acute general hospitals and seven mental health services and audited 176 case notes. In addition, each secondary care service provided information on systems they used to identify and flag people with learning disabilities, what they were doing in relation to reasonable adjustments, arrangements they had for liaison with specialist staff, and information on staff training.
The researchers consulted people with learning disabilities and carers, and carried out surveys with 614 staff and 141 service users and carers.
Findings
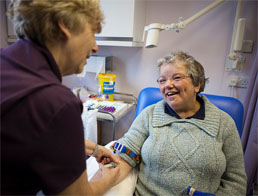
Low uptake of annual health checks in study practices mirrored national levels, along with substandard recording of health action plans
They found in the primary care practices they worked with that there was a low uptake of annual health checks which mirrored national levels, as well as substandard recording of health action plans.
In secondary care services, they found difficulties in identifying people with learning disabilities and making the reasonable adjustments and issues relating to learning disability were not included in mandatory training programmes
In relation to the need for an audit, there was good support from all stakeholders.
All primary and secondary care sites said they would be willing to take part in a national audit but called for such an audit to complement existing or upcoming quality improvement initiatives in learning disabilities support.
They identified a number of challenges
- Limited time and competing priorities
- Engaging primary care services throughout the audit cycle (e.g. sign up, access to and sharing of data; use of data for ongoing quality improvement, commissioning level engagement for success
- Identifying patients in secondary care services – each service had to identify 15 eligible patients for case note audit. In the absence of an agreed flagging system they had to rely on community teams, learning disability liaison nurses and ICD-10 coding.
- The need to consider both physical and mental health irrespective of the care setting, in line with ‘parity of esteem’
The audit team also point out that the audit work fits with other national priorities for learning disabilities in the NHS, as well as reflecting the Care Quality Commission’s Essentials Standards of Quality and Safety.
Conclusion and comment
It is clear from the work of the audit team that some of the issues identified in previous reports could be addressed by a national audit and audit methodology could be used to identify and measure progress against agreed standards nationally and locally. There was clearly also a good deal of support from all stakeholders, including those working in primary and secondary health care services.
The audit feasibility team developed 28 criteria were developed for primary care and 21 standards for secondary care and recommend ways in which services could be recruited, based on their experience. It was difficult to recruit practices into the feasibility study and there is no doubt that this would be an issue in a national audit, but linking to NHS priorities and CQC requirements could positively influence that participation.
However, whilst the initial response from NHS England has been to welcome the findings, the decision has been not to support a clinical audit, but rather to proceed with a National Learning Disability Mortality Review.
Dominic Slowie, (National Clinical Director for Learning Disability) was also keen to point out that insights from the feasibility study would incorporated into the ongoing development of the Learning Disability Self-Assessment Framework.
Given the concerns about lack of progress on the key recommendations of the Confidential Inquiry, it remains to be seen whether this approach will have the necessary support to bring about the change that is so clearly needed.

NHS England have welcomed the findings, but do not support a national clinical audit, but rather national learning disability mortality review
Link
National Audit of Learning Disabilities Feasibility Study, prepared by Aarti Gandesha, Pamela Gallagher, Alan Quirk and Mike Crawford from the Royal College of Psychiatrists; and Megan Lanigan and Umesh Chauhan from the Royal College of General Practitioners.
Reference
Identifying the factors affecting the implementation of strategies to promote a safer environment for patients with learning disabilities in NHS hospitals: a mixed-methods study, Tuffrey-Wijne I et al., in Health Services Delivery Research, 2013;1(13)

Learning Disability National Audit – feasibility study and recommendations and future plans http://t.co/cyFg64TyIO