
When trying to understand more about about mental health problems one of the big questions is: are the results of a study due to how the person is currently feeling or are the results due to a predisposition to how they are feeling now? While often the answer will be a bit of both, researchers can try and tease these apart by using more sophisticated study designs. One way to do this is to recruit the relatives of people with serious mental illnesses, who are at higher risk of developing the illness themselves (1). These people start participating in the study before seeing any mental health professionals and are then seen by the research team over a number of years. Some of these people will subsequently develop an illness and the information gathered allows researchers to try and work out whether any differences between individuals at the start of the study predicts the later development of an illness.

Don’t forget, us elves look beyond the headlines to bring you the full story
Because of the relatively robust nature of this type of study method it can lead to the BBC, STV and others headlining stories like: ‘Depression could be diagnosed before onset, study suggests’ (2). Here at the Mental Elf we like to delve a wee bit deeper to understand studies like this and hopefully can help you understand why this study is really interesting but the findings do not quite match the reporting in the mainstream media.
Methods
People with an established diagnosis of bipolar affective disorder or depression have been found to have differences in brain activations on a range of fMRI tasks. These differences are mainly in emotionally sensitive areas of the brain and have been found even when people are doing tasks that do not seem to require any emotional processing. This study was designed to examine whether these differences are found before a diagnosis can be made or any treatments have been tried.
Researchers in Edinburgh have long experience in running this type of study: both in schizophrenia and bipolar affective disorder. For this study they recruited people who had either a parent, sibling or child with bipolar affective disorder alongside a control group with no family history. Both groups had a psychiatric assessment and were excluded if they had any personal history of mood disorder or psychosis. After two years the majority of participants were reinterviewed by the same psychiatrists. For those who did not attend the second appointment (21%, no significant difference between the groups) their GP provided information about whether they had experienced an episode of mental illness over the preceding 2 years.
At the first assessment all the participants had an MRI scan. This included using fMRI to examine the brain activity associated with the Hayling sentence completion task. This task asks participants to think of an appropriate word to complete a sentence, e.g. He posted the letter without a ____ . The task can be manipulated to make the completion harder: by making the sentence more ambiguous.
58 controls took part in the study. Of the 98 people with a family history of bipolar affective disorder involved, 20 experienced their first episode of depression during the two years between the assessments. Therefore three groups were compared:
- Healthy controls (HC)
- People with a family history who did not experience a clinically significant episode of depression (FH well)
- Those did who experience a clinically significant episode of depression (FH MDD)
The analysis of the data followed standard procedures and was robust. Mood symptoms at the time of scan were taken account of when analysing the task activation patterns, but measures of personality were not.
Results
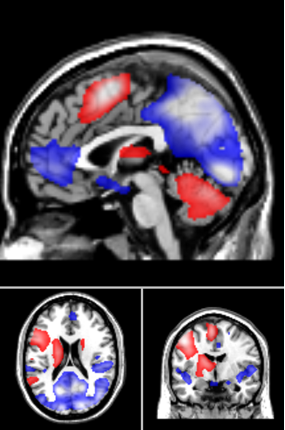
Fig 1: Pattern of activation whilst completing the sentence in the Hayling Sentence Completion Task. Red shows areas that are more active than the rest, blue show areas that are less active.
Clinical and behavioural differences
- As measured by the Hamiliton Depression Rating Scale, the groups differed on baseline depression symptoms (but no participant had enough symptoms to merit a diagnosis of depression).
- Personality traits associated with the development of depression (extraversion, neuroticism and cyclothymia) followed the same pattern: significantly higher in those who developed depression, with the FH well group intermediate between the HC group and the FH MDD groups.
Functional MRI
- All groups completed the task effectively and showed the expected pattern of brain activation whilst doing the task (see figure 1).
- When looking at which parts of the brain were more active as the sentences became more ambiguous and the completion of them got harder, the same areas changed in all the groups.
- Those people who subsequently developed an episode of depression overactivated the insula. This is an area of brain very strongly associated with emotional processing and is normally deactivated whilst doing a non-emotional task.
- Overactivation of the insula was also associated with higher levels neuroticism, extraversion and cyclothymia.
Conclusions
The authors concluded:
These findings suggest that there is a pattern of abnormal brain activation that predicts major depressive disorder in young individuals at high familial risk which is related to trait liability measures of mood disorder but not to current symptomatic state.
And that it can offer interesting insights into the potential biology of depression:
This fits with cognitive models of depression where there is suggested to be a disproportionate allocation of resources to the internal experience of emotional responses, and a withdrawal of responses from higher order cognitive processes involved in the reappraisal of negative emotions.
Summary

Having a family history of bipolar or depression will increase your chances of getting the disease
- Family members of people with bipolar affective disorder have an increased risk of developing both bipolar affective disorder and unipolar depression.
- Those family members who go on to experience an episode of depression have the same personality traits that have been found to predispose to depression generally.
- They also struggle to turn down emotional parts of their brain when doing a hard task.
- These findings are not related to the mood of the person at the time of doing the task.
- This study looked at people who are at high genetic risk of bipolar affective disorder who developed depression. Some of these people will go on to receive a diagnosis of bipolar affective disorder and whether the findings here relate to a general risk of depression or to depression in bipolar affective disorder (and whether depression is the same in these conditions) needs more research.
- Unfortunately the mainstream media reporting was wrong: this study can not be used to diagnose depression before it starts but does suggest that there are personality and brain imaging changes that increase the chances of a person with a family history of bipolar having an episode of depression.
Links
Whalley HC, Sussman JE, Romaniuk L, Stewart T, Papmeyer M, Sprooten E, Hackett S, Hall J, Lawrie SM, McIntosh AM. Prediction of Depression in Individuals at High Familial Risk of Mood Disorders using Functional Magnetic Resonance Imaging. PLOS ONE. 2013; 8 (3).
Depression could be diagnosed before onset, study suggests. BBC News Edinburgh, Fife and East Scotland, 6 Mar 2013.



Brain imaging suggests that differences in emotional processing are present before developing depression: When… http://t.co/iOoGuTn8a2
@andrewwatson28 blogs @PLOSONE study of fMRI to predict depression in ppl w/ high familial risk of mood disorders http://t.co/arThMslxFS
V interesting study on emotional processing predispositions in #depression on @Mental_Elf by @andrewwatson28 http://t.co/4g13yY2dHx
Did @BBCScotlandNews misreport the research about diagnosing depression before onset? http://t.co/O8sf3uLulb @senseaboutsci
Brain imaging suggests that differences in emotional processing are present before developing depression – The Mental http://t.co/lAP4C5BSWe
Don’t miss: brain imaging suggests differences in emotional processing are present b4 developing depression http://t.co/O8sf3uLulb
RT @Mental_Elf: Brain imaging suggests emotional processing differences are present before developing depression http://t.co/ChrY2xRxSu