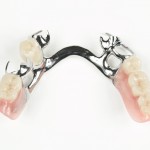
The aim of this study was to assess the cost-effectiveness analysis of two different tooth replacement strategies for partially dentate older patients; partial removable dental prostheses (RDP) and functionally orientated treatment based on the shortened dental arch concept (SDA).
Partially dentate patients aged 65 years and older seeking replacement of missing natural teeth, had a mini- mum of six remaining natural teeth in either arch of good prognosis, could accept routine dental care in a dental chair, could communicate in English and had no medical conditions which precluded routine dental treatment were recruited.
All patients received standardised initial care (oral hygiene instruction, non-surgical periodontal treatment, treatment of caries and replacement of restorations and extraction of teeth with poor prognosis) and where then randomised to the RDP group or SDA group. Patients in the RDP group had restoration of complete arch using cobalt–chromium frameworks used to replace missing teeth. Patients in the SDA group were restored to a shortened arch of 10 occluding pairs of natural and replacement teeth using resin-bonded bridgework (RBB).
All of the RDP and RBB were constructed by the same dental laboratory. All operative treatment was conducted by a single clinician with postgraduate training in prosthodontics.The main outcome measure was oral health–related quality of life (OHrQOL), measured using the short form of the oral health impact profile (OHIP-14). The OHIP-14 was administered at baseline and 6 and 12 months after treatment.
- 132 patients were randomised (65 in RDP group – 67 in SDA group) – mean age 70.18 years (range 65 to 92 years).
- 20 patients (30.8%) were lost from the RDP group and 20 were lost from the SDA group (29.9%) leaving 92 patients for the 12 months recall.
- 5 RBB debonded and were re-cemented over the 12-month (95.5% success)
- 4 patients discontinued wearing their RPDs (all lower RPD with bilateral free end saddles).
- Both groups recorded statistically significant improvements in OHrQoL scores 12 months after treatment.
- Total cost of improvement of improvement in RDP group €586.37 compared with €384.05 for SDA group.
- Cost of achieving the minimally important clinical difference (MID) in OHrQOL of 5 scale points for an average patient in the RDP group at 12 months was €464.64 compared with €252.00 in the SDA group. The cost-effectiveness ratio was therefore 1:1.84 in favour of SDA treatment.
The authors concluded
With an increasingly ageing population, many patients will continue to benefit from removable prostheses to replace their missing natural teeth. From a purely economic standpoint, the results from this analysis suggest that the treatment of partially dentate older adults should be focused on functionally orientated treatment because it is simply more cost-effective.
Comment
As the authors note with increasing longevity, increasing numbers of older people maintaining more teeth and changing attitudes to dental care there is likely to be greater demand to restore missing teeth. Basis this cost effectiveness study on a randomised controlled trial provides some good data. However the dropout rates of 30% (although perhaps not unexpected in this age group) in each group needs to be borne in mind along with the follow-up period is only 12 months when considering the findings.
Links
McKenna G, Allen F, Woods N, O’Mahony D, Cronin M, Damata C, Normand C. Cost-effectiveness of tooth replacement strategies for partially dentate elderly: a randomized controlled clinical trial. Community Dent Oral Epidemiol. 2013 Nov 20. doi: 10.1111/cdoe.12085. [Epub ahead of print] PubMed PMID: 24251386.

[…] Dental Elf – 10th Jan 2014 – Study suggests use of resin-bonded bridgework more cost eff… […]