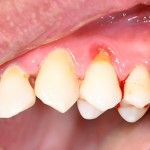
Gingival recession is quite common and a wide range of techniques has been developed to cover exposed roots. The subepithelial connective tissue graft (SCTG) is considered to be the ‘gold standard’ approach and has a good success rate. However, a number of authors have reported on the use of root surface modifiers to improve success rates further. The aim of this review was to evaluate whether different methods of root biomodification could improve clinical outcomes in gingival recessions (Miller Class I and Class II) treated with SCTG.
Methods
Searches were conducted in the Medline, Embase and Central databases with additional hand searches of the Journal of Clinical Periodontology, the Journal of Periodontology, the Journal of Periodontal Research and the International Journal of Periodontics and Restorative Dentistry. Two reviewers independently screened the studies, abstracted data and assess quality and risk of bias.
Randomised controlled trials (RCTs) and controlled clinical trials (CCTs) reporting SCTG for root coverage associated with any form of root surface biomodification were considered. Primary outcomes considered were percentage of root coverage and complete root coverage. Secondary outcomes were Secondary— depth and width of gingival recession, width of keratinized tissue (WKT), gingival thickness, pocket depth, clinical attachment level patient perception of root sensitivity or aesthetics.
Results
- 6 RCTs (3 parallel studies, 3 split mouth) involving a total of 157 patients and 211 recessions were included.
- All studies evaluated Miller class I & II gingival recessions.
- 3 studies were considered to be at low risk of bias, 3 at moderate risk.
- Studies were considered to be too heterogeneous to pool.
- None of the agents evaluated; Citric acid, EDTA (Ethylenediaminetetraacetic acid) , platelet-rich plasma (PRP) lasers or enamel matrix derivative (EMD).
Conclusions
The authors concluded:
Based on the clinical data presently available, the use of root surface modifiers to improve clinical outcomes in Miller Class I and Class II gingival recessions treated with SCTG is not justified. More in vivo studies, and randomized clinical trials with a larger number of patients (allowing for a proper statistical analysis) and extended follow-up periods, are necessary to investigate further the influence of root biomodification in the healing process and the success rate of root coverage on long-term evaluation.
Comments
This review searched 3 major databases and an number of specialist journals and only identified a small number of small studies assessing whether the use of surface modifiers improved outcomes for in Miller Class I and Class II gingival recessions. The results suggest that there is currently no evidence to support their use at present. Earlier this year we looked at a review, which tackled the wider issue of periodontal surgery for localised gingival recessions (Dental Elf – 23rd Jun 2015). That review found that coronally advanced flap alone or with a connective tissue graft was supported by a large body of evidence.
Links
Karam PS, Sant’Ana AC, de Rezende ML, Greghi SL, Damante CA, Zangrando MS. Root surface modifiers and subepithelial connective tissue graft for treatment of gingival recessions: a systematic review. J Periodontal Res. 2015 Jun 11. doi: 10.1111/jre.12296. [Epub ahead of print] PubMed PMID: 26095265.
Dental Elf – 23rd Jun 2015 – Periodontal surgery for localised gingival recessions

@TheDentalElf EDTA tx root surface’s usually done at SCTG.But tunneling technique’s not needed because can’t be done(flapless at that teeth)
Root surface modifiers did not improve outcomes in gingival recessions http://t.co/mRrogInfoE
Gingival recession surgical outcomes not improved with root surface modifiers http://t.co/mRrogInfoE
Root surface modifiers and gingival recession surgery http://t.co/mRrogInfoE
No benefit to gingival recession surgery from with root surface modifiers http://t.co/mRrogInfoE
Don’t miss – Root surface modifiers did not improve outcomes in gingival recessions http://t.co/mRrogInfoE