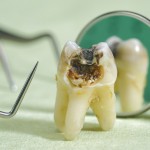
A whole host of studies has looked at the physical consequences of mental illness. Today, it is known that this connection is bidirectional in nature:
For instance, while suffering from a mental illness increases the risks of significant physical/medical comorbidity, including diabetes, heart disease and stroke (Lawrence et al, 2000), it has also been shown that many “primarily medical” conditions increase the risks of mental illness.
Among the most prominent, suffering from diabetes, inflammatory illnesses or cancer is associated with higher chances of depression (Katon, 2011).
However, to this date very little is known about whether these links between “body and mind” also extend to oral health. Poor oral health has been linked with systemic illnesses such as coronary heart disease, diabetes or respiratory disease, which may mediate links with mental health (Arigbede et al, 2012; Humphrey et al, 2008).
In addition, dental hygiene affects eating and speech, and thus has an impact on social and psychological aspect of life (Mirza, 2001). To review the evidence out there, Kisely and colleagues have recently presented a systematic review and meta-analysis (Kisely et al, 2015).
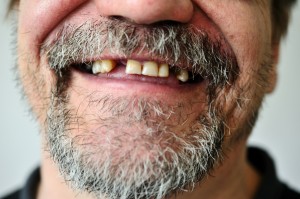
Authors reviewed studies that assessed oral health of people with severe mental illness.
Methods
The authors screened major medical databases for studies that assessed oral health of people with severe mental illness. Total tooth loss (edentulism) and dental decay were taken as proxy of oral health and assessed via mean number of decayed, missing and filled teeth or surfaces.
Results
In total, 25 studies covering 5,076 psychiatric patients and 39,545 non-affected controls were included into the analysis. Odds ratios, mean differences and 95% confidence intervals were calculated.
- People with severe mental illness were 2.8 times more likely than controls to have lost all their teeth (95% CI for Odds ratio: 1.7 to 4.6)
- People with severe mental illness had higher numbers of decayed, missing or filled teeth (mean difference = 5, 95% CI = 2.5 to 7.4)
- People with severe mental illness also had significantly higher surface scores (mean difference = 14.6, 95% CI = 4.1 to 25.1)

People with severe mental illness were 2.8 times more likely to have lost all their teeth, and had more missing, decayed or filled teeth.
Conclusion
The authors concluded:
The increased focus on the physical health of people with SMI should encompass oral health. Possible interventions could include oral health assessment conducted using standard checklists that can be completed by non-dental personnel, help with oral hygiene, management of iatrogenic dry mouth, and early dental referral.

The authors recommended that people with severe mental illness should be given help with oral hygiene.
Limitations
While the authors state that their analyses suggest absence of publication bias for some measures, such analyses were not possible for others due to small numbers of studies.
In addition, there was significant variation among outcome measure scores and assessments. This problem is made worse by an overall “not optimal” study quality that might have compromised internal validity. For instance, established diagnostic criteria for mental illness (e.g. DSM-IV) were used only in a fraction of studies and very often there was no control group. While the authors try to compensate for this by using external controls, there is no guarantee this procedure provides an adequate comparison.

The authors attempted to compensate for their lack of control groups by using external controls, but this process may have provided inadequate comparisons.
Of note, there were sex differences when comparing psychiatric patients and healthy controls: As expected, males were overrepresented in the psychiatric samples, which could have influenced the associations between oral hygiene and mental health. However, separate analyses that included matched groups only revealed similar results. And obviously, there was no blinding of dental assessment which threatens internal validity.
Finally, there was great heterogeneity in the results, which the authors tried to correct for statistically, but which still makes any interpretations tentative.
A Comment from the Dental Elf
The DMFT index (Decayed, Missing and Filled Teeth) that is used in this paper is not particularly sensitive because a tooth can only be ascribed D, M or F. Ideally the DMFT index would be zero. If all teeth are removed/lost or all filled it would be 32.
Essentially the D component represents a treatment need and the M and F components could be said to represent treatment provision. For a decayed tooth, a filling F would be the best option.
The missing component M could be an indication of previous orthodontic treatment (a tooth being removed to make space to reduce crowding). The only possible treatment option would be:
- Tooth badly broken as a result of trauma
- Extensive tooth decay – too bad to restore
- Extensive gum disease – too much supporting tissue lost
- Patient unable or unwilling to pay for more extensive (expensive) treatment to restore tooth
Any one of these last three (2-4) could be down to an inability to access (or interact) with dental services regularly. This could be down to patient factors or service factors; either or both not appreciating the needs and or implication of dental care for this client group.
Summary
While limited in many ways, this paper provides some interesting information about the connection between mental illness and poor oral hygiene.
More specifically, it raises awareness that people with mental disorders may be at a particularly high risk of dental problems. As such, the authors suggest that this patient group be recognised as particularly vulnerable and that screening for oral health be part of a more thorough assessment of psychiatric patients.
Links
Kisely, S., Baghaie, H., Lalloo, R., Siskind, D., & Johnson, N. W. (2015). A systematic review and meta-analysis of the association between poor oral health and severe mental illness. Psychosomatic Medicine, 77(1), 83–92. doi:10.1097/PSY.0000000000000135 [Abstract]
Arigbede, A. O., Babatope, B. O., & Bamidele, M. K. (2012). Periodontitis and systemic diseases: A literature review. Journal of Indian Society of Periodontology, 16(4), 487–91. doi:10.4103/0972-124X.106878
Humphrey, L. L., Fu, R., Buckley, D. I., Freeman, M., & Helfand, M. (2008). Periodontal disease and coronary heart disease incidence: a systematic review and meta-analysis. Journal of General Internal Medicine, 23(12), 2079–86. doi:10.1007/s11606-008-0787-6 [Extract]
Katon, W. J. (2011). Epidemiology and treatment of depression in patients with chronic medical illness. Dialogues in Cinical Neuroscience, 13(1), 7–23.
Lawrence, D., Jablensky, A. V, Holman, C. D., & Pinder, T. J. (2000). Mortality in Western Australian psychiatric patients. Social Psychiatry and Psychiatric Epidemiology, 35(8), 341–7. [Extract]
Mirza, I. (2001). Oral health of psychiatric in-patients: A point prevalence survey of an inner-city hospital. Psychiatric Bulletin, 25(4), 143–145. doi:10.1192/pb.25.4.143




RT @Mental_Elf: Poor oral health and severe mental illness: what are the links? http://t.co/EEy4H5WFdl
Low self esteem due to appearance, which may cause social isolation, which may lead to depression or addiction to cope. Just guessing
@Mental_Elf Possibly to do with how grown up people feel about dentists? Need to make childhood experiences better…xx
Poor oral health and severe mental illness: what are the links?: Helge Hasselmann summarises a recent systemat… http://t.co/PIJ5i4v5OL
Argument for CCGS to commission dentistry? MRT“@Mental_Elf: Poor oral health and severe mental illness: what r links http://t.co/tPawoYsZNE“
We’ve joined forces with @TheDentalElf today, for a blog about severe mental illness & poor oral health http://t.co/EEy4H5WFdl
People with #mentalhealth problems are particularly vulnerable to dental problems http://t.co/udeoUVzkLW @Mental_Elf @TheDentalElf
@Sectioned_ @Mental_Elf @TheDentalElf Dental Health should be a priority
@Sectioned_ @Mental_Elf @TheDentalElf I have known dentists observe reductions in bone/tooth density likely from use of the medications
@MickBramham @Sectioned_ @Mental_Elf @TheDentalElf In the depths of alcoholism & depression I convinced myself to bourbon cleaned my teeth
@Mental_Elf @TheDentalElf Sounds like an interesting collaboration!
Irene Trilla liked this on Facebook.
The Mental Elf liked this on Facebook.
New SR finds ppl w/ severe mental illness were 2.8 times more likely to have lost all their teeth http://t.co/EEy4H5WFdl
@Mental_Elf statistics gone mad methinks!
Dry mouth is a common side effect of psychopharmaca, isn’t it? MT @Mental_Elf more likely to have lost all teeth http://t.co/1qsGJuBgad
Systematic review concludes that ppl w/ severe mental illness have more missing, decayed or filled teeth http://t.co/EEy4H5WFdl #parity
http://t.co/f8V1z748nO… http://t.co/FDhqps0PBM
Not a clear cut link. Yes some with oral hygiene problems do occur with mental health. Some occur because of medication. I did take NSAID’s for osteoarthritis but was NOT prescribed lanzaprazole for 10 years even though I had been suffering acid reflux. Hence my teeth had become damaged and had to be removed. I now wear dentures. I don’t suffer any mental health problems thankfully.
Good talk betw @Mental_Elf @TheDentalElf @Sectioned_ @MickBramham about severe mental illness & poor oral health http://t.co/JZMplVWtnq
Mental Elf: Poor oral health and severe mental illness: what are the links? http://t.co/Ef4e6BRImg
Poor oral health and severe mental illness: what are the links? http://t.co/Np0t7fxKy1 via @sharethis
Don’t miss: Poor oral health and severe mental illness: what are the links? http://t.co/EEy4H5WFdl #EBP
“Slechte mondgezondheid en #EPA: wat is het verband” via @Mental_Elf http://t.co/zvl038DJSk #yam
Read the Anonymous Press http://t.co/UwgCne5OkK
[…] Poor oral health and severe mental illness: what are the links? […]
Studies don’t seem to recognise the link between childhood trauma and poor oral health. I can’t stand having someone close to my face let alone touching my mouth and issues with general self neglect common with depression mean that I rarely brushed my teeth. They’re now breaking off to the gum line and I’m in pain most days. I tried my gp for help. Was told I just need to see a dentist and was prescribed codeine. 2 yrs on and still no dentist but am addicted to codeine.
[…] Poor oral health and severe mental illness: what are the links? […]
Please look at saliva content as reason for decay – as well as neglect or absence of dental facilities. I have PTSD which typically has high CRP and low alpha 1 antitryspin https://www.sciencedirect.com/science/article/pii/0003996995000895 whether it cause or effect I do not know . I am on several PTSD forums and the rates of failed root canals is excessively high in PTSD support groups – I wonder if given increased failure rates we should be advised for root canal or tooth removal – I am suffering now with removal of 100% of my root canal teeth which have failed and dry socket which I suspect is related to the brutality of tooth removal when older due to denser bone and preexisting anaerobic infection which was not treated because of passive antibiotic prescription protocols – I think we need a complete seperate set of protocols for people so prone to infection and root canal failure – with 20-20 hindsight I would never have had root canal work done post my diagnosis with PTSD as they seem doomed to 100% failure and caused gum and bone issues -which could have been avoided with extraction instead of root filling.
Very interesting. Fifty five ish years ago I broke a front tooth root. I just left it alone. Recently my mental health took a big hit and then tooth fell out. The socket was badly infected. I have just completed the first part of having an implant and that included antibiotics and a strong mouth wash. My mental health has be completely reset to (my) normal that I remeber all those years ago. I have a medical- biochemistry background.
@ben_hr @Mental_Elf Being denied urgent healthcare I need strikes at the heart of my vitality that I’m consumed by depression & despair
@ben_hr @Mental_Elf Would love to see more research into this.
@adventurensw Is urgent health care or dental care that’s being denied? @ben_hr @Mental_Elf
@CalamityJane_66 @ben_hr @Mental_Elf health – surgery. My dental is ok
@CalamityJane_66 @ben_hr @Mental_Elf If I was in UK, my surgery is wholly sponsored by government nothing to pay. Now it’s surgery or bust
@adventurensw Sorry, I was just replying to @ben_hr RT of @Mental_Elf’s research into links between oral health and mental illness
@CalamityJane_66 @ben_hr @Mental_Elf ok
@CalamityJane_66 @ben_hr @Mental_Elf In mental illness they neglect personal care sometimes & oral care unaffordable without work