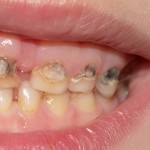
Caries is a very common childhood problem and sadly results in pain and infection which for many may be chronic in nature. Chronic pain has been shown to affect cognitive function in children so may affect both school attendance and performance.
The aim of this review was to assess the evidence on the possible influence of oral health on school performance and school attendance in children and adolescents.
Methods
Searches were conducted in the Medline, Scopus, Web of Science, ScienceDirect and LILACS databases. Clinical trials and observational (cohort, case‐ control and cross sectional) studies in participants under 18 years of age that assessed oral health status and school performance and/or school attendance published in any language were considered. Study selection data abstraction and risk of bias assessment was conducted independently by 3 reviewers with disagreements being resolved by discussion with a 4th reviewer. Study quality was assessed using the Newcastle-Ottawa scale. Odds ratios (OR) and 95% confidence intervals (CI) were calculated and meta-analysis used to obtain pooled adjusted estimates between oral health measures and school performance and school attendance.
Results
- 18 studies (1 Cohort, 1 case control, 16 cross-sectional) were included
- Sample sizes ranged from 312 – 65680 participants.
- A majority of the studies were considered to be of moderate quality.
- 15 studies contributed to the meta-analysis
- Children with one or more decayed teeth had 44% higher probability of poor school performance than caries‐ free children; OR=1.44 (95%CI; 1.24‐ 1.64) [5 studies,3205 children].
- Poor school performance was significantly associated with poor paternal perception of children’s oral health; OR= 1.36 (95%CI;1.16 ‐1.57) [5 studies, 30995 children].
- Children with decayed teeth had significantly higher odds of having poor school attendance than those without dental caries; OR = 1.57 (95%CI; 1.08‐ 2.05) [5 studies, 4416 children].
- Parents of children with poor school attendance were more likely to report poor oral health of their child; OR = 1.35 (1.14- 1.57) [3 studies].
Conclusions
The authors concluded: –
The currently available evidence suggests the need for high‐quality longitudinal studies to ascertain whether poor oral health influences school performance and school attendance. The use of reliable information from school records regarding school performance and school attendance and valid oral health measures are paramount to reach more definitive conclusions on this subject. In addition, socioeconomic status and family structure are important aspects to be considered in future studies.
The findings from the present meta‐ analysis provide grounds for the harmful effect of untreated dental caries and poor subjective oral health on the child’s and adolescent’s inadequate school performance and poor school attendance. Effective public health approaches to reduce oral diseases are available and can impact on the Target 2A of the Millennium Development Goals: complete a full course of primary schooling.
Comments
This review has undertaken an extensive literature search to identify studies for inclusion. All the included papers are observational which is to be anticipated but with the exception of 2 they are all cross-sectional which needs to be taken into consideration when interpreting the findings, a point highlighted by the authors. They also point out that only just over half of the studies (61%) took into account socio-economic status and only one considered family structure. The included studies also involve a broad age range from 2-18yrs.
So while this review suggests a 44% higher probability of poor school performance in children with caries these findings should be interpreted cautiously because of the limited quality of the evidence. High quality prospective studies are needed to clarify the impact of oral health status on school attendance and performance.
Links
Primary Paper
Rebelo MAB, Rebelo Vieira JM, Pereira JV, Quadros LN, Vettore MV. Does oral health influence school performance and school attendance? A systematic review and meta-analysis. Int J Paediatr Dent. 2018 Oct 26. doi: 10.1111/ipd.12441.[Epub ahead of print] Review. PubMed PMID: 30367538.
Original review protocol on PROSPERO
