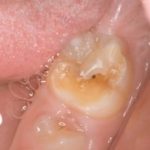
Enamel hypomineralisation results from an alteration in the n the transition or maturation stage of amelogenesis or the secretion stage. Molar incisor hypomineralisation (MIH) can affect one or more of the first permanent molars and permanent incisors and a similar enamel defect can be seen in second primary molars called hypomineralised second primary molars. Wide variation has been reported in the literature and a number of diagnostic criteria have been used.
The main aim of this review was to assess the worldwide prevalence of hypomineralised second primary molars.
Methods
A review protocol was published on PROSPERO. Searches were conducted in the Medline/PubMed, Scopus, Web of Science and OpenGrey databases. Cohort, case-control, and cross-sectional studies reporting on enamel defects in children and published in English were considered. Two reviewers independently selected studies with two teams of reviewers extracting data and assessing risk of bias using a modified version of the Newcastle-Ottawa Scale. Meta-analysis was undertaken to provide a pooled prevalence of hypomineralised second primary molars (HSPM).
Results
- 37 papers involving 26,805 patients were included.
- 32 papers presented data on child prevalence and 23 on tooth prevalence.
- Studies were conducted between 1979 and 2020 in Africa, Asia, Australia, Europe, and South/ North America.
- The overall pooled prevalence
- child level of HSPM = 6.80% (95%CI: 4.98% to 8.86%) [32 studies].
- tooth level of HSPM = 4.08% (95%CI: 2.80% to 5.59%) [23 studies].
- Higher levels of HSPM were reported in studies using the EAPD or MIH/HSPM index
- child level of HSPM = 7.54% (95%CI: 5.48% to 9.89%).
- tooth level of HSPM = 65% (95%CI: 2.96% to 6.70%).
- 15 studies provided information of HSPM characteristics with demarcated opacities being the most common presentation at child and tooth level.
Conclusions
The authors concluded: –
there was a broad variation in the prevalence reported that may be attributed to differences in the study population. The present meta-analysis showed a HSPM prevalence worldwide of 6.8% on a child level and 4.1% on a tooth level. There is a need for more standardised information to be provided on the type of HSPM defect, presence of sensitivity, and respective treatment needs. Further research is also required in certain countries where no prevalence data exist. Determining the prevalence of HSPM will inform early detection and management strategies according to the defect severity.
Comments
The reviewers published their protocol and followed a typical systematic review approach. They have searched four major databases and have identified a good number of papers from a wide range of countries. However, the decision to include only English language papers may have excluded some relevant studies. A majority of the included studies were cross-sectional (29) with 7 cohort and one randomised controlled trial. It has been suggested that 5 years of age is the optimal age for the diagnosis of HSPM, but this varied across the studies as did other characteristics including environmental factors, socio-economic characteristics, study methodology including training and calibration of examiners, examination conditions and diagnostic criteria used. As a result, the pooled estimates had a high level of heterogeneity. It is easy to agree with the reviewers call for more standardised information on HSPM and widespread agreement on diagnostic criteria as the review demonstrates the influence of this on prevalence data.
Links
Primary Paper
McCarra C, Olegário IC, O’Connell AC, Leith R. Prevalence of hypomineralised second primary molars (HSPM): A systematic review and meta-analysis. Int J Paediatr Dent. 2021 Aug 25. doi: 10.1111/ipd.12892. Epub ahead of print. PMID: 34432910.
Other references
Dental Elf – Hypomineralised enamel blogs
