
If you’ve ever been laid up in a plaster cast, you will know how frustrating and painful a fracture can be. For us elves there is the added complication of making plaster casts small enough, and trying to keep them clean and dry in the woodland.
For some people the risk of fractures is greatly increased, and this risk generally increases with age. Osteoporosis is a common condition of greater than normal rates of bone loss, and the degradation of some of the internal structuring and scaffolding of the bones. This leads to a higher risk of fractures and all of the associated complications in terms of morbidity and mortality.
People with schizophrenia have long been thought to be at increased risk of osteoporosis and its precursors; osteopaenia and low bone density. However, as with many of these types of studies research is lacking, or lagging behind other areas. Putative mechanisms for this are:
- Increased prevalence of unhelpful lifestyle factors in patients with schizophrenia such as smoking, physical inaction, excess alcohol use and vitamin D deficiency
- Increased prolactin levels due to antipsychotic medications
Two recent population studies have shown that people with schizophrenia are at higher risk of hip fractures, and had worse long term outcomes than controls (Howard, 2007; Sørensen, 2013). All of this has prompted the current study, a meta-analysis by Stubbs et al, which examines overall bone density in more detail.
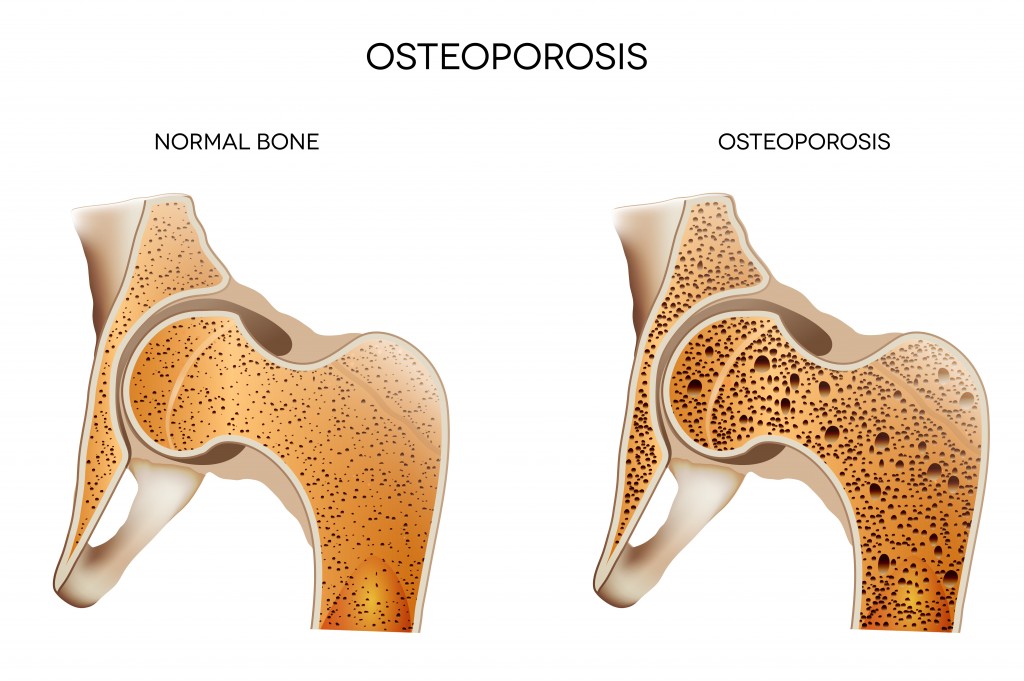
Osteoporosis affects around 3 million people in the UK.
Methods
Stubbs and his colleagues undertook a systematic review of the literature pertaining to schizophrenia and low bone mass, using the usually recognised guidelines (MOOSE and PRISMA in this case). Using the usual on-line sources and databases, they searched for the terms “(osteoporosis or osteopenia or osteo* or bone mineral density or DXA or DEXA or bone) AND (schizophrenia or schizo* or psychosis).” From this, they included articles in any language which measured bone density in patients with a diagnosis of schizophrenia, although some also included small numbers of patients with schizoaffective disorder. They looked ideally for a clear measure of bone density coming from dual-energy X-ray absorptiometry (DXA) scan results or from quantitative ultrasound (QUS). Because they anticipated the groups and studies to vary considerably (high heterogeneity) they adjusted their statistical methods to account for this.
Data was then taken from each study by two of the authors independently on the following domains:
- Study region
- Patient setting
- Sociodemographic data of patients and controls
- Presence of known risk factors for low bone mass
- Smoking rates
- Type of antipsychotic medication and its duration
- Duration of schizophrenia
- History of fractures
- Pre- or post-menopausal (females)
- Serum blood measures – prolactin, osteocalcin, vitamin D
Overall the authors used a robust and recognised method to gather the data necessary for their study. The main difficulties in applying this were that only a small number of studies were found, and these studies varied from one another considerably. There is a danger where this happens in that the subsequent analyses lead to multiple different comparisons of sub-sets of the data. In this case they took the above factors and compared each of the three disease states (osteoporosis, osteopaenia and low bone density) for each one. With so many comparisons it is possible that findings due to chance alone slip by, depending on the level of statistical significance reached. Indeed the authors later comment that some of the associations initially made lost statistical significance once a Bonferroni correction was applied.
Results
What they found were 19 suitable studies (out of an initial 529 identified) reporting on 3,038 patients with a diagnosis of schizophrenia compared with 1,531 controls (only 8 studies included had control groups). The authors looked at the results for each illness state separately and then looked at the studies where patients were compared to controls.
Low bone mass
- When analysed as a whole nearly 52% of the schizophrenia patients had low bone density (Confidence Interval (CI) 43.05 to 60.3%) and the statistical tests done by the authors showed that publication bias was unlikely to be significantly affecting this outcome
- Factors associated with lower bone mass in the patient group were:
- Older age
- Higher BMI
- Postmenopausal females
- Being male, the duration of illness, antipsychotic use and high prolactin levels did not appear to affect the findings
- Those in Europe and Asia had higher rates than in North America
- Those in in-patient settings were almost twice as likely to have low bone mass than those in out-patient settings
- In-patient settings 60.3% (CI 49.6 to 70.1%)
- Out-patient settings 32.9% (CI 21.6 to 46.7%)
Osteoporosis
- 13.2% (CI 7.8 to 21.6%) of those with schizophrenia were found to have osteoporosis
- Older age, male gender and postmenopausal female status were more likely to be affected
- Again, it did not appear that prolactin raising antipsychotics or high prolactin levels played a part, neither did BMI, length of illness or smoking status
- North Americans faired better, as did those who were not in in-patient care at the time of the studies
Osteopaenia
- Likewise there were high rates amongst those with schizophrenia 40.0% (CI 34.7 to 45.4%)
- This time, being male and being a smoker was associated with higher prevalence
- Being in a study where all participants were on antipsychotics raised the risk compared to studies where only some patients were prescribed these drugs
Compared to controls
- Those with schizophrenia (n=746) had a statistically significantly higher risk (almost double) of developing low bone density (OR 1.9, CI 1.3 to 2.77, p <0.001) compared to controls
- Statistically significant higher risk was seen for osteoporosis (OR 2.86, CI 1.27 to 6.42, p =0.01)
- The risk for osteopaenia was not statistically significant (OR 1.33, CI 0.93 to 1.90, p = 0.1)
- The results were the same no matter whether it was DXA or other scanning modalities used to examine the participants

This meta-analysis by Stubbs et al finds two and a half times risk of osteoporosis in those with schizophrenia.
Conclusions
These findings add to the established literature and show that one in two people with schizophrenia will have low bone mass, almost twice the rates of their age and gender matched peers.
The authors comment that the low number of studies suggests that this has so far been an under-researched area, and more work is needed. They draw attention to some of the limitations of their study (the low numbers, inconsistent findings regarding the risk factors) and accept that there is inconclusive data to determine the putative mechanisms by which those with schizophrenia develop problems more frequently.
In terms of recommendations for clinical practice:
- Clearly it is worth considering the inclusion of screening those with schizophrenia for reducing bone density
- Vitamin D supplements may be appropriate (this may be the explanation for lower rates in North American patients)
- Smoking cessation advice would seem a sensible way to reduce the risk
- Physical activity programmes, particularly for those in in-patient settings, may be of help
- Protocols for the multidisciplinary team to monitor and help educate patients regarding their particular risk factors
Further work is always needed, and particularly here where the number of studies is relatively small and shows inconsistent results. Stubbs and his colleagues have helped to raise the profile of this problem for those with schizophrenia, allowing clinicians and patients alike to make better choices to reduce their chances of low bone density leading to falls and fractures.

With a two-fold risk of low bone density, should we be more proactive in screening patients with schizophrenia?
Links
, , , , , , , . (2014) A meta-analysis of prevalence estimates and moderators of low bone mass in people with schizophrenia. Acta Psychiatrica Scandinavica 2014 pp1-17. [Abstract]
Howard L, Kirkwood G, Leese M. Risk of hip fracture in patients with a history of Schizophrenia. Br J Psychiatry 2007;190:129–134.
Sørensen HJ, Jensen SOW, Nielsen J. Schizophrenia, antipsychotics and risk of hip fracture: a population based analysis. Eur Neuropsychopharmacol 2013;23:872–878. [PubMed abstract]

RT @Mental_Elf: Schizophrenia and osteoporosis: sticks and stones may break my bones http://t.co/QsESF9Erbc
Schizophrenia and osteoporosis: sticks and stones may break my bones…: Chris Pell summarises a recent meta-ana… http://t.co/ppWr8e8n8C
Osteoporosis is increased in ppl w schizophrenia http://t.co/z8jJ2iEIjv review by @Mental_Elf our our paper @mndsci @DavyVancampfort
More evidence that mental health and physical health should be considered together, from @Mental_Elf http://t.co/D8EOCj8awD
Olivia Cialdi liked this on Facebook.
.@BrendonStubbs @_alexjmitchell @DavyVancampfort We’ve blogged about your MA on low bone mass & schizophrenia http://t.co/bia6jOWmBk Pls RT
Lower bone mass in ppl w #schizophrenia blog by @Mental_Elf http://t.co/z8jJ2iEIjv @FGaughran @Davidiris1 #schizophreniaawarenessweek
@BrendonStubbs @Mental_Elf @FGaughran high risk of future bone disease highlighted by Brendon Stubbs and colleagues
“@Mental_Elf: Schizophrenia and osteoporosis: sticks and stones may break my bones http://t.co/YcXikfZtKG” Great piece by @egosyntonically
Nice one Chris @egosyntonically “@Mental_Elf: Schizophrenia and osteoporosis: sticks and stones may break my bones http://t.co/LMFh36l6Zv”
Today @egosyntonically on meta-analysis of prevalence estimates & moderators of low bone mass in ppl w/ schizophrenia http://t.co/bia6jOWmBk
Susan Munro liked this on Facebook.
The Mental Elf liked this on Facebook.
People with schizophrenia have a 2.5 times increased risk of osteoporosis http://t.co/bia6jOWmBk #schizophreniaawarenessweek
Schizophrenia and osteoporosis http://t.co/oGA7SEJcqK
Maz Taylor liked this on Facebook.
June Dunnett liked this on Facebook.
Hampshire Healthcare Library Service liked this on Facebook.
Nancy Johnson-Schoenecke liked this on Facebook.
With a two-fold risk of low bone density, should we be more proactive in screening patients with schizophrenia? http://t.co/bia6jOWmBk
Schizophrenia and osteoporosis: sticks and stones may break my bones… http://t.co/YxjA7xyuz8
Mental Elf: Schizophrenia and osteoporosis: sticks and stones may break my bones… http://t.co/5Y4v4WY4bY
RT @Mental_Elf: Osteoporosis affects around 3m people in UK, but why are people with schizophrenia more susceptible than most? http://t.co/…
Don’t miss: Schizophrenia and osteoporosis – sticks and stones may break my bones… http://t.co/bia6jOWmBk #schizophreniaawarenessweek
My @Mental_Elf blog from yesterday on schizophrenia and osteoporosis: http://t.co/eLs1xhnRuy in case you missed it.
Schizophrenia and osteoporosis: sticks and stones may break my bones… http://t.co/HuCSwfqNxL via @sharethis Is there not a lithimum link
Brendon Stubbs liked this on Facebook.
Carina Kirby liked this on Facebook.