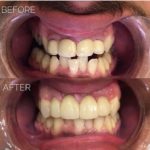
Crown lengthening may be necessary in order to place a restoration and involves the adjustment of the gum and bone level in order to expose more of the tooth prior to restoration. This can be achieved using an apically positioned flap (APF) with or without osseous resection or gingivectomy.
The aim of this review was to assess whether surgical crown lengthening (SCL) produces stable clinical outcomes for restorative treatment.
Methods
Searches were conducted in the Medline, Embase Cochrane Central Register of Controlled Trials and Cochrane Oral Health Group Trials Register. This was supplemented by hand searches of the journals, Journal of Clinical Periodontology, Journal of Periodontology, and Journal of Periodontal Research. English language clinical controlled trials (CCTs) involving SCL procedure that includes APF with osseous resection were considered.
The author selected studies and abstracted data and assessed risk of bias based on the CONSORT statement and the Cochrane risk of bias tool. The primary outcomes were crown length (CL) increase position of gingival margin (PGM), biological width (BW) and bone level changes. Separate meta-analysis were conducted for each outcome.
Results
- 5 controlled clinical trials were included.
- The studies were conducted in India (2); USA (2) and Switzerland (1).
- All 5 studies were considered to be at high risk of bias.
| No. of studies | Range of mean changes in individual studies | Weighted mean difference ( 95%CI) | |
| Crown length | 3 | 1.4 to 3.33 mm | −1.84 (−0.103 to 2.05) |
| Position of gingival margin | 4 | 1.57 to 9.4 mm | 0.87 (0.12 to 1.62) |
| Biological width | 2 | −0.07 to −0.44 mm | −0.11 (−2.21 to 1.99) |
| Bone level changes | 2 | 1.27 to 3.5 mm. | 1.64 (1.26 to 2.03) |
- 2 studies reported significant tissue rebound after SCL
- 2 studies reported outcomes of APF with osseous resection that produced more stable clinical outcomes compared to controls (without APF + ostectomy).
Conclusions
The authors concluded: –
It remains debatable whether SCL produces gingival rebound or re-establishes BW and changes in clinical attachment level; however, further studies with low risk of bias randomized CCTs and long-term follow-up are recommended to reliably assess the restorative outcomes of SCL.
Comments
While a standard methodological approach was taken for this review using a good range of databases only English language papers were included and only a single reviewer was involved. Restricting the searches to English language papers may mean that relevant studies were excluded and use of a single review raises the possibility of personal biases that are reduced using two or more reviewers.
Only a small number of small studies with were included providing limited evidence to address the question. This is further compromised by the quality of reporting of various aspects of the primary publications, eg. the variability of reporting of periodontal parameter or details of surgical technique and none of the studies had a follow up period of longer than 6 months. There is also no reporting of adverse effects or patient relevant outcomes. Further high-quality studies with longer follow up periods are needed using a common outcomes to provide better evidence on the effectiveness of SCL.
An earlier review by Pilalas et al in 2016 also addresses this question and recommends additional research to ‘fill significant voids in our knowledge on several procedural aspects’ related to SCL.
Links
Primary Paper
Al-Sowygh ZH. Does Surgical Crown Lengthening Procedure Produce Stable Clinical Outcomes for Restorative Treatment? A Meta-Analysis. J Prosthodont. 2018 Jun 6. doi: 10.1111/jopr.12909. [Epub ahead of print] Review. PubMed PMID:29876998.
Other references
Pilalas I, Tsalikis L, Tatakis DN. Pre-restorative crown lengthening surgery outcomes: a systematic review. J Clin Periodontol. 2016 Dec;43(12):1094-1108.doi: 10.1111/jcpe.12617. Epub 2016 Oct 25. Review. PubMed PMID: 27535216.
Photo Credits
By AmirAttallah – Own work, CC BY-SA 4.0.
