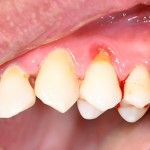
The aim of this review was to assess the clinical efficacy of periodontal plastic surgery procedures in the treatment of localized gingival recessions (Rec) with or without inter-dental clinical attachment loss (iCAL).
Methods
Searches were conducted in Medline, The Cochrane Database Trials Register, Embase and the journals; Journal of Clinical Periodontology, Journal of Periodontology, Journal of Periodontal Research, International Journal of Periodontics and Restorative Dentistry and PERIO without language restrictions.
Only randomised controlled clinical trials (RCTs), including split-mouth model, for the treatment of single gingival recession of at least 6 months duration were considered. A wide-range of periodontal surgery procedures including combination techniques were considered ( see table)
| Coronally Advanced Flap (CAF); |
| CAF plus Connective Tissue Graft (CAF+CTG) |
| CAF plus Guided Tissue Regeneration (GTR) procedures for root coverage (CAF+GTR) |
| CAF plus Enamel Matrix Derivative (CAF+EMD) |
| CAF plus Acellular Dermal Matrix (CAF+ADM) |
| CAF plus porcine Collagen Matrix (CAF+CM) |
| CAF plus Platelet Concentrate Graft (CAF+PCG) |
| CAF plus Human Fibroblast-Derived Dermal Substitute (CAF+HF-DDS) |
| CAF plus Bone Graft Substitute (CAF+BGS) |
| CAF plus Platelet-Rich Fibrin Membrane (CAF+P-RFM) |
| CAF plus Semilunar Coronally Positioned Flap (CAF+SCPF) |
| Double Papilla Flap (DPF) plus CTG (DPF+CTG) |
| Semilunar Coronally Positioned Flap (SCPF) |
| Laterally Positioned Flap (LPF) |
| Free Gingival Graft (FGG) |
The primary outcome was complete root coverage (CRC). Secondary outcome variables included recession reduction (RecRed) and keratinized tissue (KT) gain. Two reviewers independently abstracted data an conducted risk of bias assessment using the Cochrane risk of bias tool.
Results
- 51 trials (53 papers) involving a total of 1574 patients and 1744 recessions were included.
- 30 different comparisons were identified and 80 meta-analyses were performed.
- Coronally Advanced Flap (CAF) was associated with higher probability of CRC and higher amount of RecRed than Semilunar Coronal Positioned Flap (SCPF).
- The combination CAF plus Connective Tissue Graft (CAF+CTG) or CAF plus Enamel Matrix Derivative (CAF+EMD) was more effective than CAF alone in terms of CRC and RecRed.
- The combination CAF plus Collagen Matrix (CAF+CM) achieved higher RecRed than CAF alone.
- In addition, CAF+CTG achieved CRC more frequently than CAF+EMD, SCPF, Free Gingival Graft (FGG) and Laterally Positioned Flap (LPS).
- CAF+CTG was also associated with higher RecRed than Barrier Membranes (CAF+GTR), CAF+EMD and CAF+CM.
- GTR was not able to improve the clinical efficacy of CAF.
- Studies adding Acellular Dermal Matrix (ADM) under CAF showed a large heterogeneity and not significant benefits compared with CAF alone.
- Multiple combinations, using more than a single graft/biomaterial under the flap, usually provide similar or less benefits than simpler, control procedures in term of root coverage outcomes.
Conclusions
The authors concluded: –
CAF procedures alone or with CTG, EMD are supported by large evidence in modern periodontal plastic surgery. CAF+CTG achieved the best clinical outcomes in single gingival recessions with or without iCAL.
Comments
The authors have conducted an extensive search of the literature identified 51 trials assessing periodontal surgery procedures for localised gingival recession. A large number of procedures have been suggested for the management of this type of recession and 30 separate comparisons were identified. However, overall the studies are relatively small and the numbers that could be included for each comparison is also small and this should been taken into consideration when interpreting these findings. In addition only 8% of the included studies provided outcomes at more than 5 years.
Links
Cairo F, Nieri M, Pagliaro U. Efficacy of periodontal plastic surgery procedures in the treatment of localized facial gingival recessions. A systematic review. J Clin Periodontol. 2014 Apr;41 Suppl 15:S44-62. doi: 10.1111/jcpe.12182. Review. PubMed PMID: 24641000.

Periodontal surgery for localised gingival recessions? http://t.co/dkDYX6Remp
Localised gingival recession surgery which technique? http://t.co/dkDYX6Remp
Localised gingival recession surgery using Coronally Advanced Flap supported by evidence. http://t.co/dkDYX6Remp
@TheDentalElf Is the method used#12blade along tooth cervical inserted free gingiva made partial thickness then outside to attached gingiva?
@ChenDeirdre – That level of procedure detail is not provided in the review paper http://t.co/dkDYX6Remp
Coronally Advanced Flap alone or with connective tissue graft for localised gingival recession. http://t.co/dkDYX6Remp
Which technique of gingival recession surgery for best clinical outcomes? http://t.co/dkDYX6Remp
[…] Dental Elf – 23rd Jun 2015 – Periodontal surgery for localised gingival recessions […]
[…] Dental Elf – 25th Jun 2015 – Periodontal surgery for localised gingival recessions […]
[…] Dental Elf – 23rd Jun 2015 – Periodontal surgery for localised gingival recessions […]