
This Mental Elf blog relates to issues that are very close to my heart: how best to meet the health needs and improve outcomes for marginalised groups with multiple needs.
Specifically, this blog will give an overview of two papers that featured in a Lancet series on Homelessness, and a review of service responses and outcomes.
What is ‘homelessness’?
Before we delve into this, it is worth considering what is meant by ‘homelessness’. Rather than referring to a specific situation, homelessness is an umbrella term for a range of circumstances where someone lacks a permanent home. These include people:
- who are roofless (no home/accommodation at all)
- in temporary accommodation (e.g. bed and breakfast)
- in other insecure or inadequate housing, such as “sofa surfing” (crashing with acquaintances but with no permanent or legal right to stay)
It is also worth making a point about the use of language to describe people who are homeless. It’s important to distinguish between the person (their identity) and the circumstances in which they find themselves. Therefore, in this blog I will be using the phrase “people who are homeless” as opposed to “homeless people” or “the homeless”. It’s so important to remind ourselves that anyone can become homeless, given a certain set of events. Homelessness is not a “lifestyle choice”. There are also a lot of stereotypes and stigma associated with homelessness, and it’s possible that this stigma could affect the ability of health services to engage with this group.

People become homeless for many varied reasons, when the events of life simply don’t pan out as hoped.
Causes of homelessness
The causes of homelessness are complex and occur as a result of interaction between individual and structural causes:
- ‘Individual causes’ refers to the circumstances that an individual may experience, such as poverty, childhood abuse, being in care, family problems, mental ill-health and/or substance use
- ‘Structural causes’ are ones that exist in society in general, such as a shortage of low-cost housing and lack of low-paid employment. Substance use, in particular, is associated with the cause and persistence of homelessness
In any given night, there are 400,000 people who are homeless in the EU, and 600,000 in the USA. This is a shameful statistic, given that both regions of the world are considered relatively “wealthy”.

The vicious cycle: adversity leads to homelessness, and homelessness causes adversity. Chronic poor health (and mental health) is the norm.
What are the health needs of people who are homeless?
The first paper, by Fazel, Geddes and Kushel (2014), reviews the health needs of people who are homeless. People who are homeless experience high rates of premature death (that is to say, dying much earlier than predicted for the general population). Causes of death relate to high rates of suicide and unintentional accidents. In addition, they experience high rates of infectious diseases, as well as non-communicable diseases (such as diabetes and cancer) as a result of poor diet, smoking and alcohol consumption.
Findings
- People who are homeless are an aging population (in USA the median age is 50 years). They experience problems related to aging (such as cognitive impairment) at a much earlier age. Being older also means experiencing more chronic diseases and conditions such as cardiovascular disease
- Likelihood of dying (mortality) is substantially increased
- Greater risk of infectious diseases, such as HIV, tuberculosis and heart disease
- Lifestyle-related risks increase, such as substance use, suicide, homicide and poisoning
- Poor health (morbidity) is also significantly more likely compared with the general population. This may be compounded by effects of poverty in early life, as well as the impact of being homeless (poor nutrition, heavy smoking, poor access to health care, injuries and substance use).
- Mental health and substance use problems are common and greatly exacerbated by being homeless
- There is wide variability in prevalence of disease within studies, but there is a consistent message that health is significantly poorer for people who are homeless

People who are homeless are an aging population, who are more susceptible to disease and mental health problems.
Recommendations
Health recommendations:
- Screening people who are homeless for infectious diseases
- Local surveys to determine the mental and physical health needs of people in the local area
- Services and treatments need to take into account effects of co-morbid substance use
- Smoking cessation interventions should be available as well as “smoke-free” accomodation
- Homeless accomodation providers to consider providing facilities to store medication (such as a fridge to store insulin), as well as providing more nutritional food (low fat, high fibre etc)
- Health staff should screen for cognitive impairments and head trauma for people over 50 years who are homeless
In terms of policy:
- National/state targets related to health outcomes for people who are homeless
- Surveillance of health in this population
- Consistency in definition of “homelessness” in order to provide more generalisable data
- Strategies for prevention of homelessness during “high risk” periods of transition (leaving the criminal justice system, psychiatric services etc)

In order to improve outcomes for people who are homeless, the authors recommend change in policy and more thorough implementation of health strategies.
What does the evidence say about the most effective way to meet health needs?
In the second paper, Hwang and Burns 2014 provide a narrative outline of the findings of a literature review of the evidence for specifically tailored models of health care for people who are homeless.
Fazel, Geddes and Kushel (2014) drew attention to the fact that despite high levels of health need, people who are homeless don’t seem to engage and access health care, and disproportionately use accident and emergency services instead, compared to general population. So, given this fact, Hwang and Burns examined whether specifically tailored interventions for people who are homeless were more effective in improving health, homelessness and other outcomes compared with standard care.
Findings
- Primary care: service users in the USA rated the quality of care within comprehensive and specialised services substantially higher than those within mainstream health services
- Mental health: specific mental health services targeting people who are homeless show improved outcomes (including reduction in hospital bed use and decrease in psychiatric symptoms), as well as increased engagement
- Two key outcomes are the reduction of homelessness and service use costs. An effective approach for achieving this is permanent supported housing with case management, which allows alcohol consumption for people with chronic alcoholism and frequent admissions to emergency departments
- Medical respite, to allow time to recuperate and receive follow-up care, has been shown to reduce re-admission
- Any substance use treatment (compared with no treatment) seems to reduce substance use. There is a debate regarding the goal of interventions, ie harm reduction or abstinence
- In terms of homeless young people, the evidence is weak. Such research has focused on improving short-term outcomes, such as substance use or risky sexual behaviour
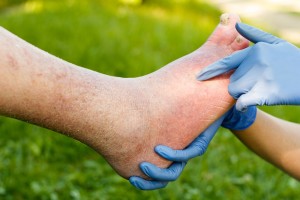
Service users rated the quality of care within comprehensive and specialised services higher than those within mainstream services.
Conclusions
The central message coming from this paper is the importance of the quality of the relationship between the service provider and the person who is homeless. This relationship is critical in order to engage people. Workers will need to adapt what they do to meet the specific needs of this group, as well as being aware of the range of services available in their local area.
A comprehensive approach, encompassing services beyond health care, is vital. In some cases, assertive outreach approaches will be required rather than expecting people to independently access the services. Mental health services should be accessible as part of a broader service, providing accommodation and general physical health care. The authors note the paradox that the likelihood of receiving care is inversely related to the complexity and need of the person, and therefore they urge practitioners to use any contact as productively as possible.

In order to improve the health of people who are homeless, housing and employment must also be involved.
Discussion
People become homeless usually as a result of adversity in their lives, as well as lack of opportunity for work and affordable housing. Being homeless has significant impact on health and well-being, and can lead to premature death. Mental ill-health and/or substance use is highly prevalent in people who are homeless.
Evidence suggests that health outcomes, as well as outcomes for housing and employment (recovery outcomes), can be improved by:
- specifically-tailored health interventions that are designed to be comprehensive and multi-disciplinary
- assertive engagement strategies
- intensive case management
The challenge for tackling homelessness, and the impact of homelessness, is that it requires a comprehensive policy drive, involving all of the public sectors: health, social care, housing, criminal justice, education and employment. There are a number of third sector initiatives pushing forward the multi-agency approach at national policy level and at local levels, including:
- Making Every Adult Matter has been established to help local areas form a comprehensive strategy, working in partnership for people with multiple needs (including homelessness)
- Homeless Link is a consortium of charities, focusing on lobbying for policy change to improve outcomes for people who are homeless.
Links
Fazel S, Geddes JR, Kushel M. The health of homeless people in high-income countries: descriptive epidemiology, health consequences, and clinical and policy recommendations. Lancet. 2014 Oct 25;384(9953):1529-40. doi: 10.1016/S0140-6736(14)61132-6. [Abstract]
Hwang SW Burns T. Health interventions for people who are homeless. Lancet. 2014 Oct 25;384(9953):1541-7. doi: 10.1016/S0140-6736(14)61133-8. [Abstract]
Homelessness series. The Lancet. October 2014. [Including podcast]


RT @Mental_Elf: Addressing the health needs of people who are homeless http://t.co/npWdCxlBH6
Addressing the health needs of people who are homeless: Liz Hughes reviews two recent Lancet papers about the … http://t.co/H3WScEQjUr
Morning @OxPsychiatry @seena9 We’ve blogged about your #homelessness paper in @TheLancet http://t.co/qdcKU3U8pN Pls share & comment
@Mental_Elf @OxPsychiatry @seena9 @TheLancet
But #RejectedFather and #PND are not included as #Tags even though #CommonRootCause #Trigger
@Mental_Elf @OxPsychiatry @TheLancet v. helpful overview. Key message is that when public services are cut, homeless health will suffer
@Mental_Elf @OxPsychiatry @TheLancet Blog highlights how health, social and housing services need integration to tackle multimorbidity
http://t.co/uWs02hEubj @chadwick_ruth the story continues
@Mental_Elf addressing the health needs of the homeless: what does the evidence say http://t.co/XOusIJG6hS
Addressing the health needs of people who are homeless http://t.co/nvWl3QASXy via @sharethis @TheQNI @ManchesterCCGs
The Mental Elf liked this on Facebook.
Addressing the #health needs of people who are #homeless http://t.co/KIyUUGRvqV A review of the #evidence from @Mental_Elf
Carina Kirby liked this on Facebook.
Today @LizHughesDD reviews 2 papers about health needs of ppl who are homeless and best ways to meet these needs http://t.co/qdcKU3U8pN
@Mental_Elf @LizHughesDD @MHARG_york @HealthSciYork interesting review highlighting important relationship between #health & #homeless
Blog on @Mental_Elf on our review of homelessness health in @TheLancet http://t.co/7seh3bakJ4
Kehksha Azam liked this on Facebook.
Pls RT @Shelter @HomelessLink @naehomelessness Addressing the health needs of people who are #homeless http://t.co/qdcKU3U8pN
@Mental_Elf @Shelter @HomelessLink @naehomelessness Both articles are free to read (w/reg) @TheLancet. First one: http://t.co/NQZgL4dSnr
@Mental_Elf @Shelter @HomelessLink @naehomelessness @TheLancet second one: http://t.co/NzcgtpSfAv
In any given night, there are 400,000 people who are homeless in the EU, and 600,000 in the USA http://t.co/qdcKU3U8pN
Meeting the health needs of people who are homeless http://t.co/4ycVnYORlC by @LizHughesDD via @Mental_Elf
Christina Armstrong-Graham liked this on Facebook.
RT @Mental_Elf: People who are homeless experience high rates of premature death, infectious disease, diabetes & cancer http://t.co/qdcKU3U…
RT @LizHughesDD: @Mental_Elf blog- homeless older population, long term conditions, heavy smoking. Hard to treat & manage http://t.co/M790p…
RT @LizHughesDD: Drugs and alcohol, & mental health a sigificant problem that can both lead to, and be exacerbated by #homelessness http://…
June Dunnett liked this on Facebook.
Rosemary Callahan liked this on Facebook.
RT @Mental_Elf: People who are homeless have an increased risk of substance use, suicide, homicide & poisoning http://t.co/qdcKU3U8pN
Relationships are key to addressing health needs of #homeless people – great blog from @Mental_Elf http://t.co/jguEVn7pS8
New research recommends screening people who are homeless for infectious diseases http://t.co/qdcKU3U8pN
.@Shelter @HomelessLink What policy changes are required to improve health outcomes for people who are homeless? http://t.co/qdcKU3U8pN
interesting blog @Mental_Elf, you might also like our research on the issue of #homeless #health http://t.co/YneGIzRkfD
New study stresses the importance of the relationship between the service provider and the person who is homeless http://t.co/qdcKU3U8pN
@Mental_Elf just noticed you are sometimes in Bristol. Would you like to come to my book launch next weds?
RT @Mental_Elf: Specific mental health services targeting people who are homeless show improved outcomes http://t.co/qdcKU3U8pN
RT @LizHughesDD: @Mental_Elf blog Homelessness & health- can’t address w/o housing & work @MEAMcoalition @HomelessLink @OllieHilbery http:/…
In order to improve the #health of people who are #homeless – #housing & #employment must also be involved http://t.co/qdcKU3U8pN
Donna Sheppard liked this on Facebook.
Raluca Lucacel liked this on Facebook.
RT @DrugScope: MT @EmpManPaul: Meeting the health needs of people who are homeless, references @MEAMcoalition work http://t.co/kyLEHx8fY9 v…
RT @Mental_Elf: Don’t miss: Addressing the health needs of people who are homeless http://t.co/qdcKU3U8pN #EBP
TY @Mental_Elf: blog http://t.co/zNAz0QaZn7 of our review of health of #homeless @thelancet http://t.co/UmDTb4ZmdV @seena9
Lucy Riddett liked this on Facebook.
Addressing the health needs of people who are homeless http://t.co/B3wuwBRf0X via @sharethis
“Addressing the health needs of people who are homeless” #zorgbehoeften #daklozen http://t.co/UQSlxgIMKZ
Addressing the health needs of people who are #homeless http://t.co/XSNcOiVlkx
http://t.co/X55AjGhpbR
Most popular blog this week? It’s @LizHughesDD on the health needs of people who are #homeless http://t.co/npWdCwMpHu
Addressing the health needs of people who are homeless
http://t.co/cHz9n1xvqr via @Mental_Elf
Outreach & quality service key to address the health needs of people who are #homeless http://t.co/gumYxiU9Bm @Mental_Elf @LizHughesDD
I often hear an argument that little work can be done therapeutically when such basic needs are unmet…. I think Liz is right that an approach needs to be comprehensive. It is sometimes an easy option for a stretched mental health service to put the responsibility all on wider systemic factors, and then abdicate involvement. I think therapeutic work can be successful alongside other professionals, which also has the added benefit of increasing shared awareness amongst professionals regarding the multifarious nature of mental health etc.